
Physician Assistants
Physical & Occupational Therapists
KneeMRI ScansNon-OperativePhysiatry
Physical Therapy
Podiatry
Spine
Sports Medicine
TraumaUrgent Care
X-Ray Imaging

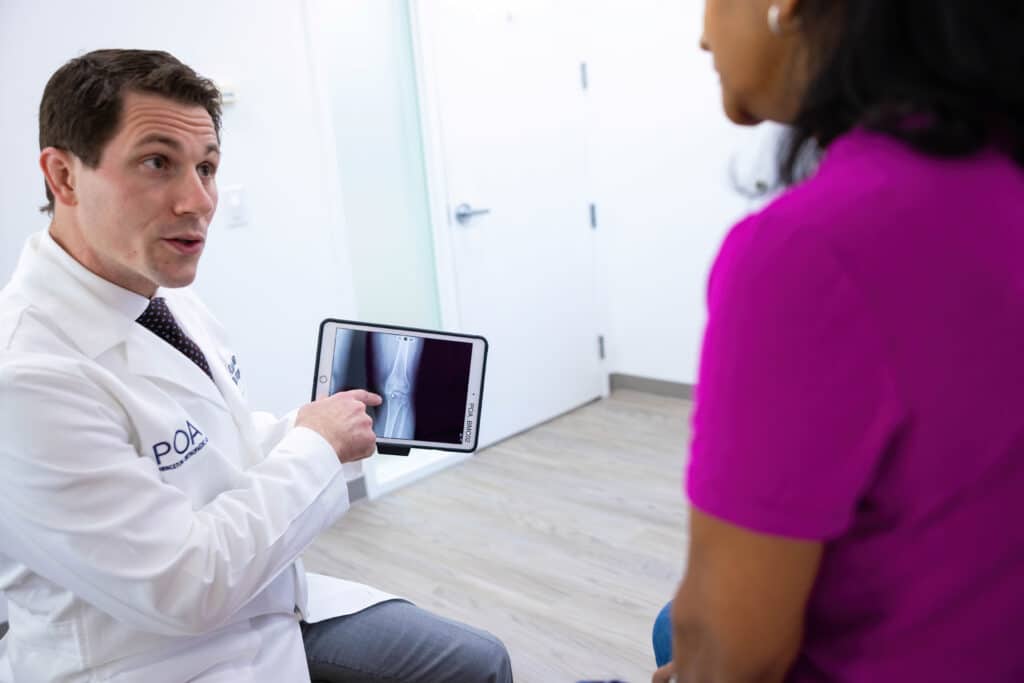
People with knee arthritis often come into the office with a common question. When is the right time to have my joint replaced? Although that varies from person to person, my answer is usually the same. When you have tried everything else, and it is bad enough, it is getting in the way of living your life." Knee replacement surgery can be an extremely effective tool to manage debilitating arthritis. It is, however, still a surgery. With all surgeries, there are risks, so we always exhaust every conservative option, and we attempt to manage those risks before ever moving forward.
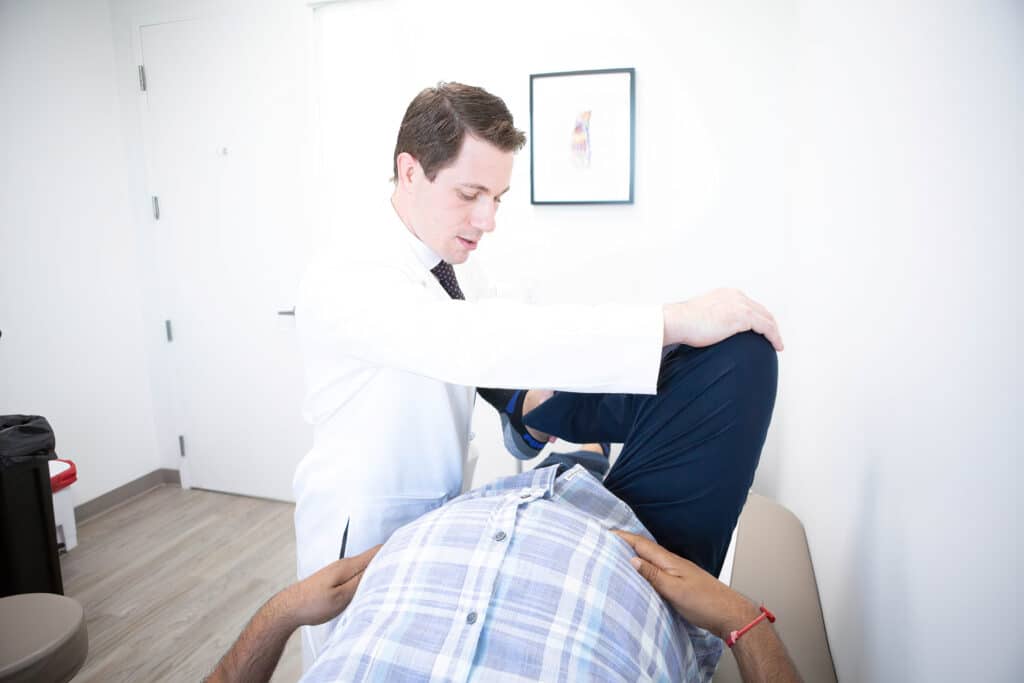
The most common complaints I get in the office include joint swelling, pain in the knee, tightness, balance issues, clicking and popping, weakness, and loss of range of motion, so these are all hallmarks of progressive arthritis of the knee. These should be evaluated by an appropriate orthopedic surgeon to determine the proper steps for you. Joint arthritis should always be managed stepwise, starting with conservative treatments first. These include the following:
1. Exercise. Exercise is great for the knee joint and can improve your function and decrease your pain. You can do this on your own with directed activities or under the guidance of a skilled physical therapist. As arthritis progresses, it can cause stiffness of the joint, leading to loss of range of motion. Pain can cause you to guard and use your muscles less fluidly, resulting in weakness. Breakdown of the joint can also lead to stability issues resulting in the sensation that one may fall. Optimizing range of motion, strength, and balance can ultimately improve the feeling of your knee and delay the need for a joint replacement in the setting of knee arthritis.
2. Weight Loss. One of the most reliable strategies to improve the pain in your knee and decrease the progression of arthritis is weight loss. Every pound of bodyweight you carry is equivalent to 4 pounds of force on the joint. What does that mean? That means that 10 pounds of weight loss are like taking a 40-pound weight off your leg. That being said, weight loss can be very challenging in arthritis. It can be challenging to find a way to exercise with a painful joint. The best strategies include low-impact exercise such as walking, swimming, and bicycling. It can also be helpful to solicit the help of a registered dietician or nutrition specialist in determining the correct foods to eat. Decreasing the overall number of calories consumed daily can be a fast track to weight loss. The quickest way to do this; avoid drinking your calories. Sipping more water and tea and avoiding sugared or artificially-sweetened drinks can allow the pounds to fly off. Finally, in extreme circumstances, you may require a bariatric surgical intervention to decrease the amount of daily caloric intake and facilitate weight loss.
3. Medication. Several medicines can also be used to manage swelling and pain safely. We often recommend that over-the-counter medications be tried first. These include Tylenol (acetaminophen) and nonsteroidal anti-inflammatories (NSAIDs). These include ibuprofen, Advil, Motrin, and Aleve. You can take these drugs safely to decrease the overall amount of joint pain one is dealing with and facilitate better function. You should monitor prolonged use under the care of a physician. Please discuss this with your doctor before taking it for more than one month's time. Narcotics and illicit drugs are very rarely the answer. While these drugs can manage acute pain, they are poor medications at managing chronic pain. We strongly recommend against taking opiate pain medications to control your osteoarthritis.
4. Injections. Injections can be an excellent tool for decreasing joint pain and improving your day-to-day life. Different injections are often employed in arthritis, with other functions and durations of use. The first-line treatment is usually a steroid (cortisone) shot. Intraarticular corticosteroid injections can decrease the swelling of the joint and improve pain and function. While these are not permanent solutions, they can have a lasting effect on many people, especially mild arthritis. Viscosupplement injections (hyaluronic acid) - while these come by several names, including gel shots (chicken fat), lubricant shots, viscosupplementation injections can be a great tool to decrease their joint pain. While not a solution for everyone, these shots can be very effective and can be taken every six months to improve the overall function in the joint and decrease pain. Discuss this with your doctor. Platelet-rich plasma and stem cell injections have become a new viable option for treatment. While these are still in investigation, they show some promising effects in joint pain and may ultimately be used as a mainstream form of therapy. However, insurance companies do not cover this form of injectable medication and may be an out-of-pocket cost for the individual. The merits of these injections should be discussed with your physician and weighed in light of the individual's degree of arthritis and age.
Surgery is the last option. When conservative options have been tried and exhausted, and the pain and loss of function affect your quality of life, surgery may be the last option on your plate. The main things to do before having surgery are to get healthy. Losing bodyweight not helps decrease the pain of the joint but also speeds your recovery and improves the longevity of a joint replacement. Also, managing your chronic conditions like blood pressure issues, diabetes, and unhealthy habits such as smoking should be optimized before choosing an elective surgery, as this may decrease your chance of complications and once again improve your overall outcome.
When it is ultimately time to consider a joint replacement, a partial or total knee replacement may suit you. This should be decided with your x-rays with your treating orthopedic surgeon. In general, we use minimally-invasive techniques, avoiding damage to the knee joint muscles. Additional technologies are utilized in the appropriate scenarios, including custom-made knee instrumentation, navigation, and robotic surgery. While not necessary for all surgeries, this can be helpful in complex systems and unique cases. Finally, joint replacement has come far enough to be performed as an outpatient procedure. Young and healthy individuals with moderate-to-severe knee arthritis may be eligible candidates to complete their joint replacement and go home the same day. Please talk to your doctor about any questions regarding your knee arthritis.

© 2023 Princeton Orthopaedic Associates. The contents of princetonorthopaedic.com are licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. Copying without permission is strictly forbidden.