
Book An Appointment
Physician Assistants
Physical & Occupational Therapists
KneeMRI ScansNon-OperativePhysiatry
Physical Therapy
Podiatry
Spine
Sports Medicine
TraumaUrgent Care
X-Ray Imaging

Trigger finger, also called stenosing tenosynovitis, happens when a finger or thumb catches, clicks, or locks as you try to bend or straighten it. We explain why it occurs, the most common symptoms, how doctors diagnose it, and the treatment options that help you get back to comfortable hand use.
If you feel a pop in your palm or need to use your other hand to straighten a finger, you are not alone. This condition is common, often treatable without surgery, and very responsive to early care.
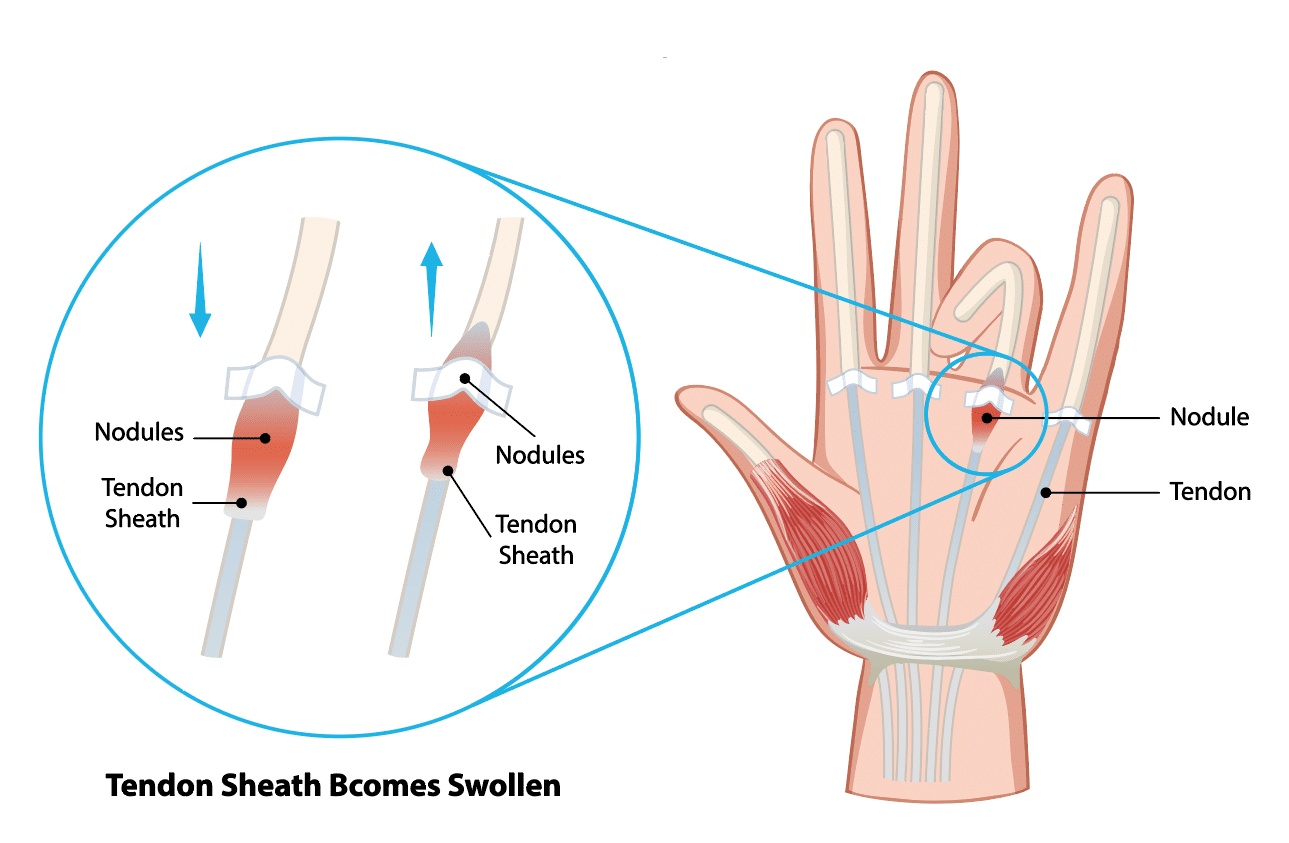
Your flexor tendons glide through tunnels in the palm called pulleys. With trigger finger, the tendon lining and the A1 pulley at the base of the affected finger or thumb become irritated and thickened. That narrowing makes the tendon catch as it moves, which creates clicking or locking.
Most people notice symptoms gradually, developing over days or weeks rather than all at once. At first, you may feel stiffness when you wake up, which improves as you use your hand. You might also notice a dull ache at the base of the finger near the palm, and a tendency for the finger to catch or click as you move it.

Several factors can irritate or swell the tendon and its sheath, which tightens the space the tendon needs to glide.
Diagnosis relies on what you tell the clinician and a careful examination of the hand. The doctor checks for tenderness over the A1 pulley, watches how the finger moves, and may feel a small lump along the tendon. Imaging tests are not usually needed unless the exam is unclear.
Many people improve without surgery, especially when care starts early. The goals are to calm irritation, help the tendon glide smoothly, and reduce stress on the pulley. You may change how you use your hand, rest the affected finger with a removable splint, and work with a therapist. In some cases, a corticosteroid injection helps reduce swelling and catching.
If symptoms persist, the finger locks frequently, or injections and splinting do not help, surgery can be a good option. The procedure is called an A1 pulley release. The surgeon widens the tight opening at the base of the finger so the tendon can glide smoothly again.
Your care plan is tailored to how your hand feels, your medical history, and what you want to return to doing. The plan explains options from less invasive treatments to surgery and describes what to expect at different stages. You and your clinician work together to choose the best path for you.
| Situation | First Steps | If Symptoms Persist |
|---|---|---|
| Mild clicking and morning stiffness | Activity changes, splinting, ice, hand therapy | Consider corticosteroid injection |
| Frequent triggering that interferes with work or self-care | Corticosteroid injection and targeted therapy | Discuss surgical release |
| Locked finger or long-standing symptoms | Prompt evaluation by a hand specialist | Surgical release is often recommended |
After treatment, moving the hand in a steady, gentle way helps the tendon glide smoothly and reduces stiffness. Whether you had nonsurgical care or surgery, follow the recommended exercises and gradually return to daily tasks. Protect the palm from heavy pressure until it feels comfortable and strong again.
Schedule an evaluation if any of the following apply:
Princeton Orthopaedic Associates treats trigger finger with careful evaluation and a plan that fits your goals. The team offers nonoperative options first and uses precise surgical release when needed. If your finger catches, clicks, or locks, you can regain comfortable hand use. Call to schedule an appointment to begin.

Please contact us! We'd love to help.
If you have pain, please contact us and schedule an appointment. We have urgent care facilities all over New Jersey for your convenience.
This blog post is meant to be informative and should not act as a self-diagnosis tool. If you’d like to see one of our doctors, please contact us here.
Shoulder labrum tears can cause deep shoulder pain, clicking, or a sense that the joint might slip. You'll learn what the labrum does, how tears happen, the most common symptoms, how we diagnose the problem, and which treatments can help you return to daily activities and sports safely. By understanding what causes labrum tears and the steps involved in evaluation and treatment, you can ask informed questions, set realistic goals, and participate actively in recovery with your care team.
The shoulder labrum is a rim of cartilage that lines the shallow socket of the shoulder joint, called the glenoid. It deepens the socket, cushions the joint, and helps your ligaments and biceps tendon keep the ball of the shoulder centered.
When the labrum tears, the joint can feel painful or unstable. Some people notice catching, clicking, or a drop in strength when lifting, pushing, or reaching overhead.
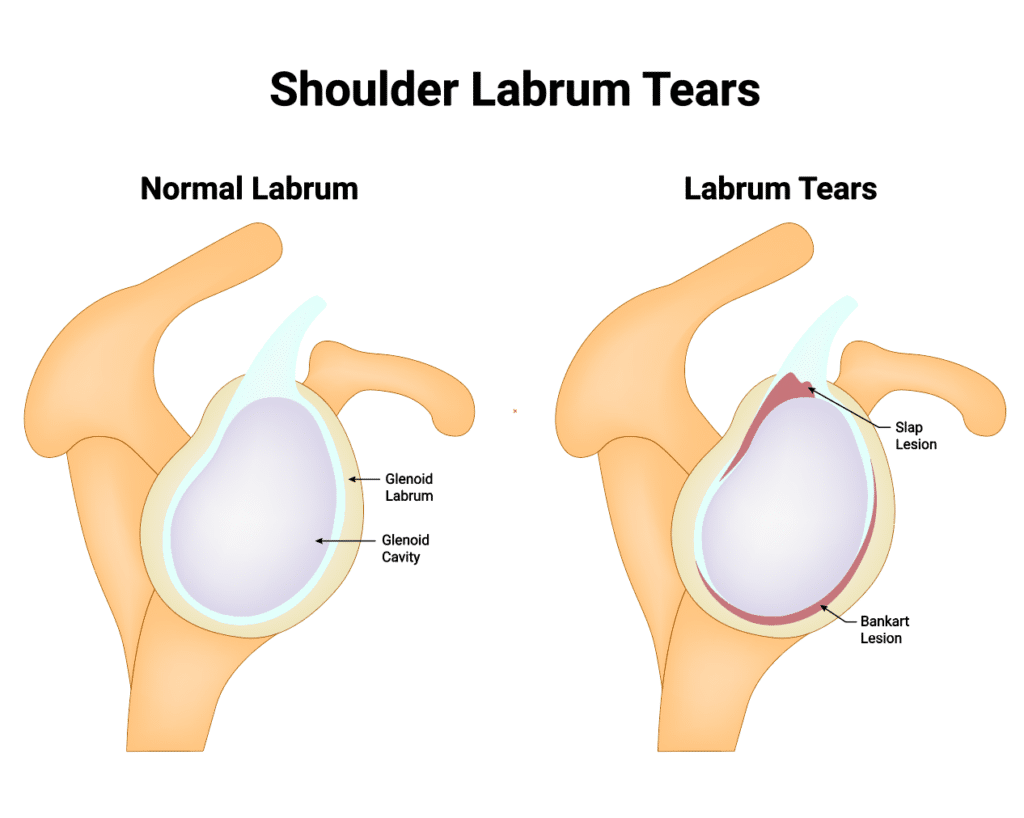
Several patterns of tearing can occur depending on where the labrum is injured and how the injury happened.
| Type | Location | Typical Cause | Common Symptoms | Typical Treatment Approach |
|---|---|---|---|---|
| SLAP Tear (Superior Labrum Anterior to Posterior) | Top of the socket where the biceps tendon attaches | Overhead sports, falls on an outstretched arm, wear-and-tear | Pain with overhead use, clicking, reduced throwing power | Physical therapy, activity modification; arthroscopic repair or biceps procedures when needed |
| Bankart Tear | Front-lower portion of the labrum | Shoulder dislocation or subluxation | Instability, repeated dislocations, apprehension with abduction/external rotation | Rehab to restore control; arthroscopic Bankart repair for recurrent instability |
| Posterior Labral Tear | Back portion of the labrum | Forceful pushing, blocking, falls, repetitive loading | Deep posterior pain, clicking, pain with pushing or bench press | Rehab focused on scapular/rotator cuff control; arthroscopic repair if instability persists |
Symptoms can vary depending on the type of labrum tear and your level of activity, but several signs are common across many cases. People may notice deep shoulder pain during lifting or overhead work, a sensation of catching or grinding within the joint, and reduced strength when pushing or throwing. Some experience night pain or reduced range of motion compared with the other shoulder. These patterns help guide evaluation and treatment choices.
Diagnosis starts with a detailed history and a hands-on exam that includes specific tests to stress different parts of the labrum and shoulder. We assess shoulder blade position, rotator cuff strength, and signs of instability.
Imaging often includes X-rays to evaluate the bones and joint alignment. An MRI, sometimes with a small amount of contrast dye in the joint, can help show the labrum and associated soft-tissue injuries.
Many labrum tears improve without surgery, especially when pain is the main issue and the shoulder is stable.
If pain or instability persists despite focused rehab, arthroscopic surgery may be recommended. Through small incisions, your surgeon can evaluate the labrum and repair or trim damaged tissue as appropriate.
Recovery depends on the type of tear, the procedure performed, and your sport or job demands. The general ranges below are common starting points that your surgeon and therapist will personalize.
| Phase | Typical Timeframe | Focus |
|---|---|---|
| Sling/Protection | 2-4 weeks after debridement; 4-6 weeks after repair | Protect healing tissue, gentle hand/elbow motion, pain control |
| Early Motion | Weeks 2-8 after debridement; Weeks 4-10 after repair | Restore range of motion under guidance, avoid provocative positions |
| Strength & Control | Months 2-4 | Scapular and rotator cuff strength, posture, gradual load |
| Return to Sports/Work | 3-4 months for non-contact after debridement; 4-6+ months after repair | Progressive sport-specific drills; throwing programs may take longer |

If shoulder pain, clicking, or instability is limiting you, we’ll examine your shoulder, review imaging when needed, and create a plan that fits your goals. Most people start with focused rehab, and when surgery is the best path, your team will guide you each step of the way.
Schedule an evaluation with Princeton Orthopaedic Associates to get moving comfortably again.

Please contact us! We'd love to help.
If you have pain, please contact us and schedule an appointment. We have urgent care facilities all over New Jersey for your convenience.
This blog post is meant to be informative and should not act as a self-diagnosis tool. If you’d like to see one of our doctors, please contact us here.
Iliotibial band syndrome, or more commonly called the IT Band, is a common source of aching on the outside of the knee or thigh. Below, you’ll learn what the iliotibial band is, why it gets irritated, how symptoms show up in daily life and sport, and the treatments that help you return to comfortable movement.
Whether you run, cycle, walk for exercise, or spend long hours sitting, this condition can affect how your hip and knee work together. The good news is that most people improve with a plan that reduces irritation and restores strength and mobility around the hip and knee.
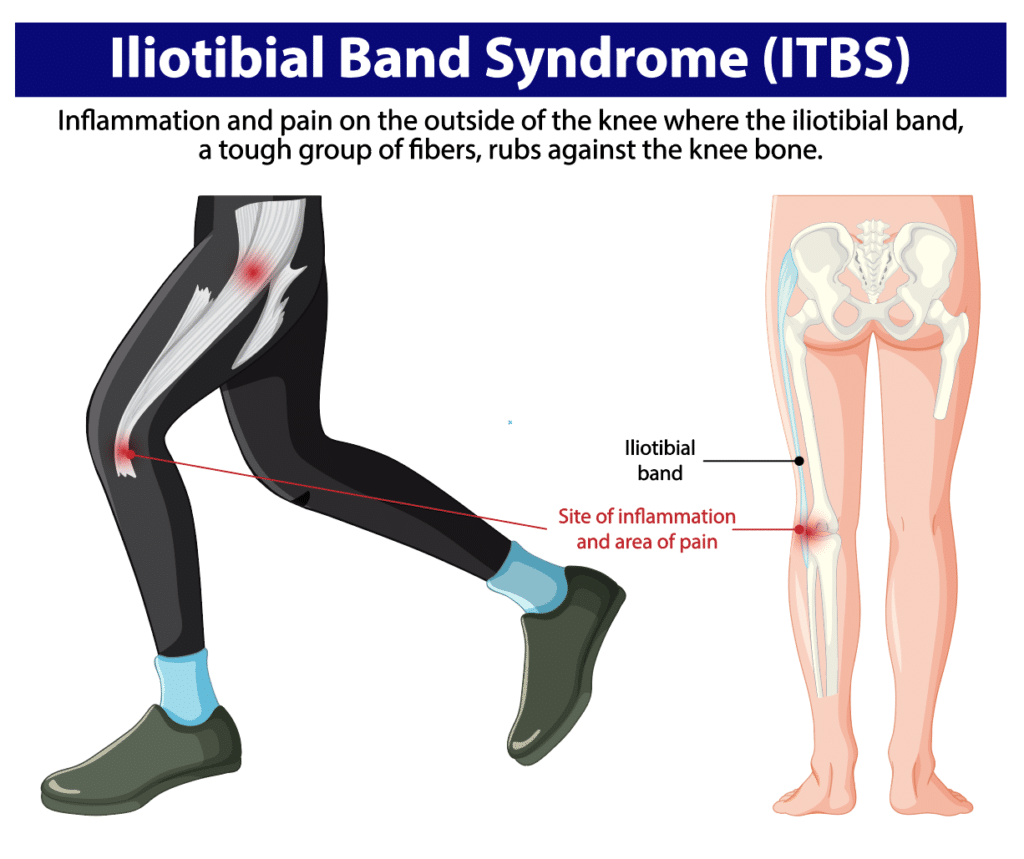
The IT band is a thick, fibrous band that supports the outside of your thigh. It connects muscles near the hip to the shinbone and helps stabilize the knee during walking, running, and standing.
Symptoms arise when tissues deep to the IT band (such as a fat pad or bursa) are compressed against the lateral femoral epicondyle during repetitive knee flexion and extension. This compression leads to irritation and pain on the outer knee, and may be felt higher up the thigh or into the hip.
Symptoms often begin gradually and worsen with repetitive flexion and extension of the knee, such as during running, cycling, or climbing stairs. People commonly describe a mix of pain on the outer knee, tightness along the outside of the thigh, tenderness when the outer knee is touched, and discomfort that changes with movement. The pain can flare with activity but may ease with rest, and occasional stiffness after sitting is not required for the diagnosis.
Symptoms often begin gradually and tend to worsen with repetitive activities. People describe:
IT band irritation usually stems from how the leg moves and how much load it is asked to handle. Multiple factors can combine to create friction near the outer knee.
A sports medicine or orthopaedic clinician typically diagnoses IT band syndrome through your history and a focused exam. They’ll check tender areas along the outer knee and hip, assess hip and core strength, and look for tightness in surrounding muscles.
Imaging is not always needed. X-rays or an MRI may be ordered when symptoms are atypical, severe, or to rule out other causes of outer knee pain such as arthritis, meniscus problems, or stress injuries.
Most people recover with a stepwise approach that calms irritation and corrects the movement issues that caused it.
For persistent pain, a clinician may consider a carefully selected corticosteroid injection in the area of irritation (often image-guided). Injections should be used judiciously as part of a broader rehab plan. Surgery is rarely needed and is considered only when symptoms fail to improve after a thorough course of nonoperative care.
Healing time varies based on how long symptoms have been present, training demands, and how consistently you follow your plan. These general ranges are common:
| Stage | Typical Timeframe | What to Expect |
|---|---|---|
| Early | Several weeks | Pain reduces with activity changes, icing, and basic mobility work. |
| Established | 1 to 3 months | Strength and movement retraining restore tolerance for daily life and sport. |
| Recurrent or Chronic | Longer than 3 months | More comprehensive rehab and training plan adjustments are needed. |
Prevention means keeping movement balanced and building strength around the hip and knee. A simple plan can help avoid flare-ups: gradually increase activity, vary routes, stretch key muscles, and choose footwear that fits your needs. Regular rest breaks and listening to your body are important to prevent irritation from returning.
Schedule an evaluation if pain lasts more than a week, returns when you resume activity, or changes how you walk or run. Early guidance helps you recover faster and reduces the risk of the problem becoming chronic.
| Specialty | Best For | Notes |
|---|---|---|
| Sports Medicine | Activity-related knee and hip pain; nonoperative care | First stop to confirm diagnosis and plan treatment |
| Physiatry | Movement analysis and musculoskeletal pain | Addresses posture, gait, and functional limitations |
| Orthopaedic Surgery | Persistent or complex cases | Coordinates imaging or advanced options if needed |
| Physical Therapy | Strength, flexibility, and gait retraining | Guides a graded return to activity and long-term prevention |
IT band syndrome can interrupt training and make everyday tasks frustrating, but it is highly treatable. With the right mix of activity changes, targeted strengthening, mobility work, and expert guidance, you can ease pain and return to the activities you enjoy.
© 2025 Princeton Orthopaedic Associates. The contents of PrincetonOrthopaedic.com are licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. Copying without permission is strictly forbidden. Privacy Policy | Accessibility
