
Book An Appointment
Physician Assistants
Physical & Occupational Therapists
KneeMRI ScansNon-OperativePhysiatry
Physical Therapy
Podiatry
Spine
Sports Medicine
TraumaUrgent Care
X-Ray Imaging


A lumbar epidural injection delivers medicine directly to your lower back to help reduce inflammation—the swelling and irritation that can occur around spinal nerves. By calming this inflammation, the injection can ease pain in the low back, buttock, or leg. In some cases, the injection also serves as a diagnostic tool, helping your provider confirm the precise source of your pain. While this treatment may not eliminate all pain for every person, it often lowers pain and inflammation enough to break the cycle of pain and immobility. When pain limits your activity, healing can slow down, and muscles can weaken. Reducing pain can help you move more comfortably, participate in physical therapy, and support your overall recovery. The level of relief varies from person to person. Some people may need more than one injection to experience meaningful improvement. Your provider will work with you to determine the best treatment plan for your specific needs. An injection can also be used for diagnosis. In a procedure known as a selective nerve block, medicine is used to briefly numb one or more specific spinal nerves. If your pain improves significantly after the injection, it confirms that the targeted nerve area is likely involved in your pain. If there is no change, your pain may be coming from another part of your spine or a different area of your body entirely. Understanding a few basics can make the procedure feel less overwhelming. Your lower back, or lumbar spine, is made of a stack of bones called vertebrae. These are separated by soft, cushion-like disks. Good preparation helps ensure your procedure day goes smoothly. Follow these steps: When you arrive, you will sign consent forms and may complete short surveys about your pain. Your provider might perform a brief physical exam. An IV line may be placed in your arm so that fluids or medication can be given if needed. Complications are uncommon, but it is important to be aware of the risks. These can include infection, bleeding, a spinal fluid leak causing a spinal headache, nausea, or nerve injury. Your provider will discuss any specific risks related to your condition and answer your questions. You may receive medicine through the IV to help you relax. Monitors will be placed to track your heart rate, breathing, and blood pressure. You will lie on your stomach or side on a procedure table. Your lower back will be cleaned with an antiseptic and covered with sterile towels. A local anesthetic is used to numb the skin at the injection site. Using fluoroscopy (a real-time X-ray) for guidance, the provider will carefully guide the epidural needle to the target area. A small amount of contrast dye may be injected to confirm the medicine will reach the correct spot. Finally, a local anesthetic for numbing, a corticosteroid to reduce inflammation, or both, will be injected into the epidural space or around the specific nerve root. You will rest in a recovery area for up to an hour for observation. Before you leave, you may be asked to complete another short pain survey. Some temporary side effects can occur, but they usually fade within a few days. These may include a temporary increase in pain, headache, flushing, or trouble sleeping. Steroid injections can also cause a temporary rise in blood sugar levels. Gentle walking is encouraged, but avoid strenuous activity for the first day or two. Even if you feel better right away, do not perform tasks that could strain your back. Remember, a diagnostic injection may provide only brief pain relief, while a therapeutic injection can take up to two weeks to reach its full effect. It is common to feel more pain at first, followed by gradual improvement. Once your provider says it is safe, gentle exercises and good body mechanics can help prevent pain from returning. Body mechanics refers to how you stand, sit, and move during daily tasks. Stop if you feel new or lasting pain during exercise and contact your provider. Your injection is one part of a larger plan for your back health. Keep talking with your provider about how you feel and what matters most to you. Simple lifestyle habits can also support your progress and reduce future flare-ups:Quick-Start Checklist
What Is a Lumbar Epidural Injection?

How Injections Can Ease Pain
Using Injections to Find the Pain Source
Your Lower Back
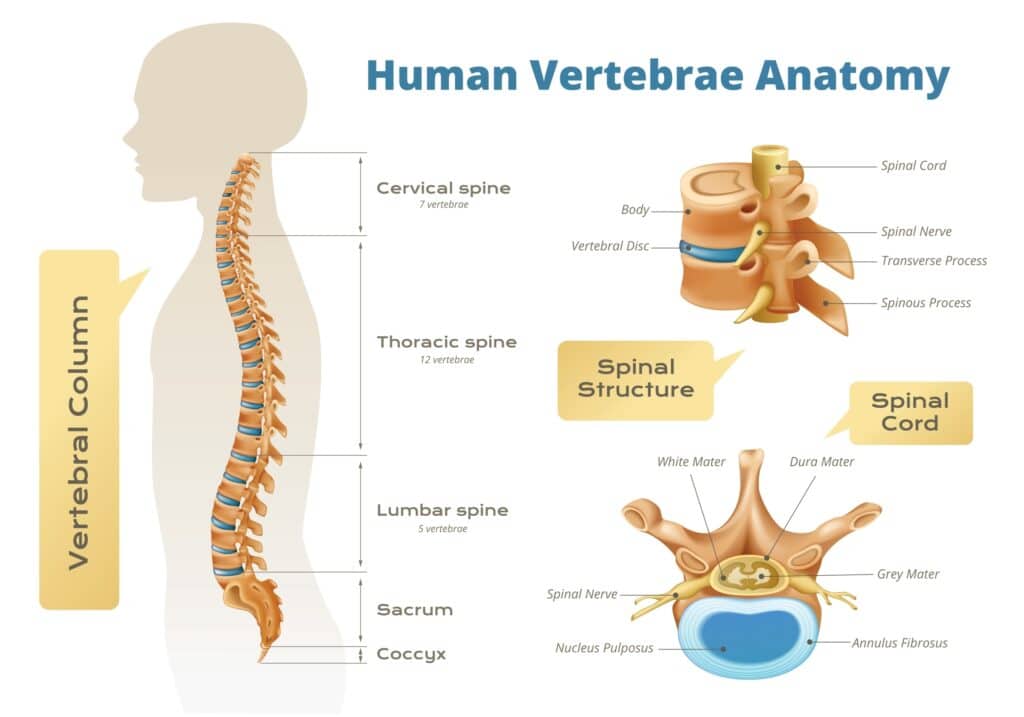
Preparing for Your Appointment
The Day of the Procedure
Checking In
Risks and Possible Complications
What Happens During the Injection
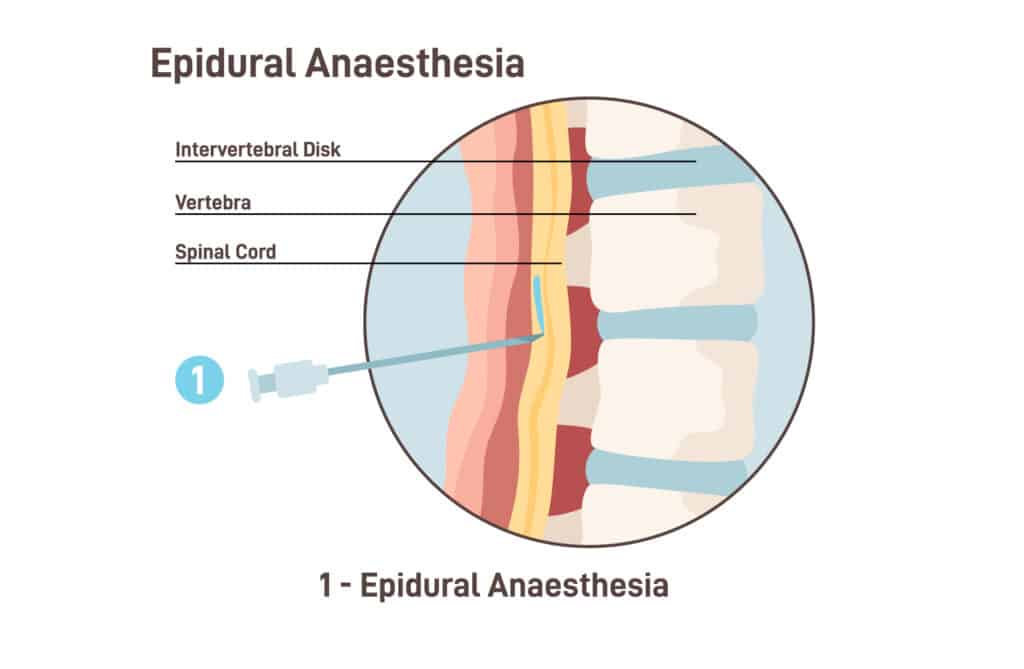
After the Injection
Immediate Recovery
Care at Home

Build Strength and Protect Your Back

Pelvic Tilt

Partial Sit-Up
How to Lift Safely
Quick Summary

© 2025 Princeton Orthopaedic Associates. The contents of PrincetonOrthopaedic.com are licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. Copying without permission is strictly forbidden. Privacy Policy | Accessibility