
Book An Appointment
Physician Assistants
Physical & Occupational Therapists
KneeMRI ScansNon-OperativePhysiatry
Physical Therapy
Podiatry
Spine
Sports Medicine
TraumaUrgent Care
X-Ray Imaging


That familiar ache at the front of your knee can make simple tasks feel hard. You might try to ignore it, only to notice it again on stairs or during a short walk. You do not have to live with those limits. There are clear steps you can take to understand the cause and start feeling better. This guide walks you through what to expect and how to move forward. Note: This article is educational and not a substitute for care from a medical professional. Only your doctor can diagnose and treat a medical condition. Pain in the front of the knee often begins with a problem involving the patella, also called the kneecap. The goal of care is to reduce pain, improve movement, and get you back to your normal activities. The goal of care is to reduce pain, improve movement, and get you back to your normal activities. What we cover: The kneecap is a small triangular bone that sits at the front of your knee joint. It works with muscles, ligaments, and bones to help you bend and straighten your leg. Cartilage is the slick, cushioning tissue that covers bone ends. It reduces friction and spreads pressure during movement. Front view: The patella looks like a small, rounded shield. Back view: The underside of the kneecap is covered by smooth cartilage. This surface helps the patella glide easily against the thighbone. Top view: The kneecap sits in a groove on the thighbone, often called the track. As you bend and straighten your leg, the kneecap slides up and down in its track on the thighbone. Position matters. Even a slight shift off the track can lead to pain or tissue irritation. Muscles and ligaments act like a system of pulleys to guide the patella. When the quadriceps, retinacula, and patellar tendon pull in balance, the kneecap stays centered and glides smoothly. Pressure is spread evenly across the back of the kneecap. Injury, tightness, weakness, or imbalance can change how tissues pull on the kneecap. If the patella drifts off its track, pressure becomes uneven. Over time, that can irritate cartilage and cause pain or stiffness. Even small tracking issues can create uneven pressure at the back of the kneecap. That can make daily movements like walking or going down stairs uncomfortable. Here are frequent causes of patella pain. Sometimes the cartilage on the back of the kneecap or in the groove of the thighbone is damaged. Damaged cartilage does not spread pressure evenly. Uneven pressure wears down the cartilage even further. This often leads to pain and stiffness. Since cartilage has little blood supply, it has a limited ability to heal. Sometimes a muscle or ligament in the knee is pulled the wrong way. Or the kneecap may be pushed too hard. Then the kneecap may move partly out of the groove (subluxation). It may even move completely out (dislocation). This can happen without warning. You may feel sudden, sharp pain or your knee may give out. Patellar tendinitis, often called jumper's knee, occurs when the quadriceps muscles are overused or tight. During movement, the patellar tendon absorbs more shock than usual. The tendon becomes irritated or damaged. This results in pain during motion or even when you are resting. Plica bands are tissue fibers that some people have near the kneecap. They usually cause no problems. But sometimes they can become irritated and inflamed. They may snap or catch on the end of the thighbone. This can cause wear and tear on the cartilage at the end of the bone. A careful evaluation helps pinpoint the reason for your knee pain. Many people see an orthopaedist, a physician who specializes in bones, muscles, and joints. Your care team will partner with you to find the cause and shape a plan that fits your goals. Your doctor will ask about your symptoms, when pain occurs, and which activities make it worse. You will also discuss past injuries, prior knee problems, and your activity level or sports. Your clinician will look for swelling, tenderness, and how your kneecap moves as your leg bends and straightens. They will also test the stability of the joint and the strength and flexibility of nearby muscles. Findings from other joints can help explain movement patterns that stress your kneecap. Tell Me Where It Hurts Imaging and procedures can clarify what is happening inside the knee. Treatment depends on the cause of your pain and your personal goals. Most people start with nonsurgical care, which includes rehabilitation and anti-inflammatory medicine such as ibuprofen or aspirin if appropriate. A physical therapist often guides your exercises. Surgery may be considered if symptoms are severe or do not improve with rehab. If surgery is needed, you will review potential risks and the recovery plan. Rehabilitation continues after healing to rebuild motion and strength. Whether you want to run again or simply walk to the corner store without pain, physical therapy can help you get there. Your therapist begins with an evaluation, then works with you to calm pain and swelling. As symptoms improve, your plan progresses to flexibility and strengthening around the knee. This balanced approach reduces stress on the kneecap and supports long-term function. Your therapist will see how your kneecap tracks and which movements increase pain. They will check your range of motion, test muscle strength, and assess stability. They may also look at your hips, ankles, and feet to find patterns that affect your knee. Pain relief and swelling control are the first priorities. Once your knee is calmer, you will begin to restore a pain-free range of motion. Your therapist will guide you in the clinic and give you strategies to use at home. Your care team may suggest one or more of the following: Swelling, tight muscles, or early scar tissue can limit how far your knee bends or straightens. These options can help restore motion: Always warm up and stretch before strengthening. Stop any exercise that causes pain and review it with your therapist or doctor. This stage begins with flexibility work to reduce pressure on the kneecap. It then progresses to strengthening so the knee is supported during daily activity. Follow your therapist's instructions for settings and repetitions. Stop any exercise that causes pain and talk with your therapist or doctor. Move slowly and avoid bouncing during stretches. Knee flexion with a towel: Sit with both legs extended and your foot flexed. Loop a towel around your heel and pull gently, sliding your heel toward your hips while keeping it on the surface. Hold the stretch across the front of your knee for about 10 seconds, then return. Hamstring stretch: Sit tall with one leg straight. Bend the other leg so the sole of your foot rests against your mid-thigh. Reach toward your ankle while keeping your knee, back, and neck straight. Feel the stretch at the back of your thigh. Calf stretch: Face a wall about two feet away. Step one foot forward, keeping the back knee straight and the front knee bent. Lean toward the wall with both heels flat. Repeat with the back knee slightly bent to target a different calf muscle. Always warm up and stretch before strengthening. Stop any exercise that causes pain and review it with your therapist or doctor. Electrical stimulation for quadriceps: A small device can help your quad muscles contract. As the unit activates, add your own muscle squeeze to increase the contraction. Your therapist may have you use the unit during certain exercises. Straight leg raise: Sit with one leg straight and the other bent. Point the toes of your straight leg toward the ceiling. Lift that leg a few inches, hold briefly, then lower with control. Repeat with the toes turned slightly out to target inner thigh muscles. Hip pulls with band or pulley: Stand with one leg about a foot from a wall and the other leg attached to tubing behind you. Pull the attached foot forward while keeping the knee straight but not locked. Return slowly to the start. Point your toes straight ahead unless your therapist guides otherwise. Leg press: Start with your knee bent to about 90 degrees. Press until the leg is almost straight, then return with steady control. Avoid locking the knee at the top. Hamstring curls: Lie on your stomach. Bend one knee as far as is comfortable, then slowly lower. Keep your back relaxed and avoid arching. Wall slide: Stand with your back against a wall, feet about 18 inches away and hip-width apart. Slide down into a near-sitting position, keeping hips above knee level. Hold for about 20 seconds, then slide back up. Repeat with toes slightly turned out to recruit inner thigh muscles. Once flexibility and strength have improved, it is time to prepare for real-life activities. These drills help you handle stairs, walking on varied terrain, and quick changes in direction. Your therapist will tailor choices to your goals. Warm up and stretch before these activities, and do not lock your knees. Stop any exercise that causes pain and discuss it with your therapist or doctor. Climbing: Use your hands for balance only. Keep your hips over your knees and your back straight. Start with 5 to 10 minutes and slowly increase time and step height. A stair-climbing machine can build strength with lower impact. Walking: If you are on a treadmill, begin with low speed or resistance. Walk with a natural stride. Start with about 20 minutes and gradually add speed, incline, and time. When walking outside, choose soft, even surfaces to lower injury risk. Side-to-side steps: With knees slightly bent, step sideways while keeping toes forward. Avoid twisting at your waist or knees. Start with 2 to 3 minutes and build up as tolerated. Jumping and landing: Keep your knees bent to absorb shock. Begin with 2 to 3 minutes and increase slowly. A trampoline helps you practice absorbing impact while bearing weight. A shuttle device lets you work on rebounding and landing without full body weight. These drills build quickness and coordination for daily life and recreation. Always stretch before and after. Rehab does not end when you return to daily routines. Your therapist may ask you to keep training a few times each week. Ongoing strength and flexibility work helps protect your knee and lowers the chance of future injuries. Surgery is considered when pain severely limits your activity or when a well-run rehab program does not provide enough relief. Some procedures are arthroscopic, which uses tiny incisions and a camera to work inside the joint. Others require open surgery. Your surgeon will explain how to prepare and discuss potential risks and complications. These procedures aim to improve how the patella tracks through its groove. Lateral release: The surgeon releases part of the retinaculum, the tight tissue on the side of the knee, to reduce the pull that tugs the kneecap out of position. A plica band may also be released if it is causing pain. Quadriceps transfer: Part of a quadriceps muscle is detached and reattached to a new spot on the kneecap to balance forces from the upper leg. Patellar tendon realignment: The attachment of the patellar tendon and a small piece of the underlying bone are moved to a new position and secured with screws. This shifts the line of pull so the kneecap tracks better. If cartilage is damaged, smoothing or stimulating new coverage can help. Debridement: Damaged cartilage is trimmed to create a smoother surface between the kneecap and thighbone. Burring to bone: When cartilage is worn to bare bone, the surgeon may lightly burr into the bone to reach the blood supply. This stimulates growth of a fibrous covering in the area. After surgery, rest is key while the knee begins to heal. Your knee may be bandaged, wrapped, or iced to control swelling. A brace can protect the joint, help restore range of motion, and support healing. Keep your leg elevated above your heart to reduce swelling. You will likely use crutches at first and may be given light exercises to begin gentle movement. A structured rehabilitation plan usually follows to rebuild strength and function. Consistency is the secret. Sticking with your exercise program during and after rehab maintains strength and flexibility around the kneecap. That support helps you stay active and reduces the chance of future knee problems.Quick-Start Checklist
Is Front-of-Knee Pain Getting You Down?
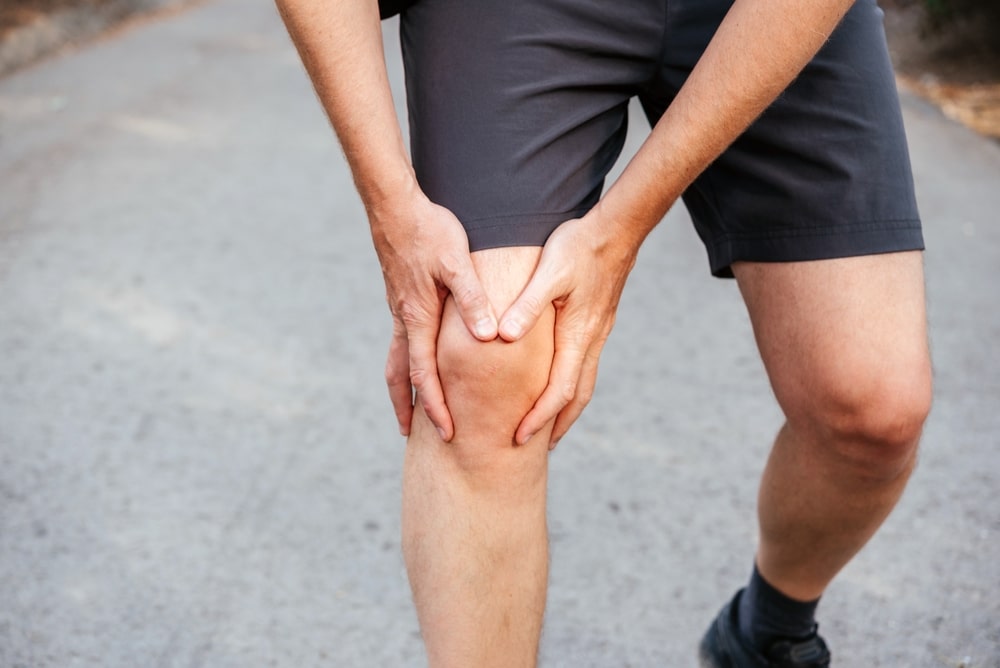
How Patella Pain Is Treated
How the Kneecap and Knee Work
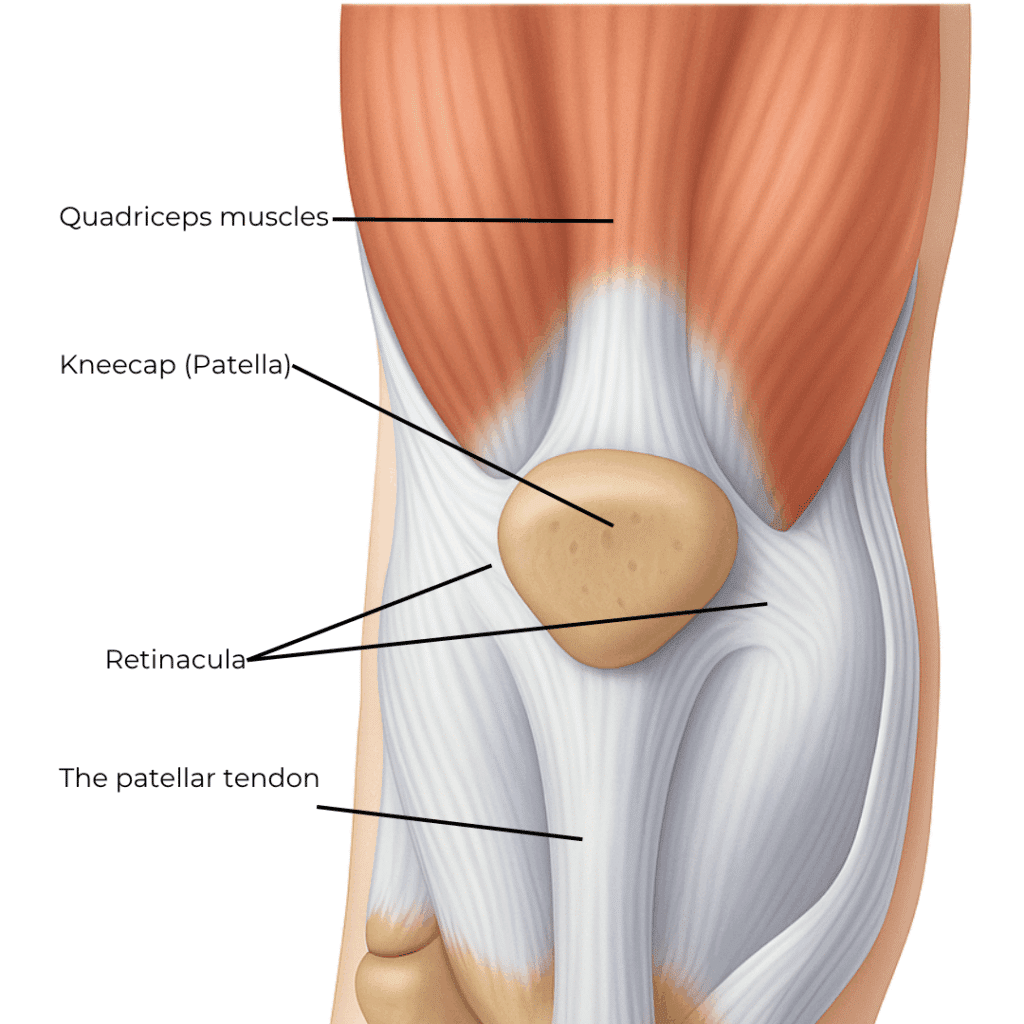
The Kneecap Up Close

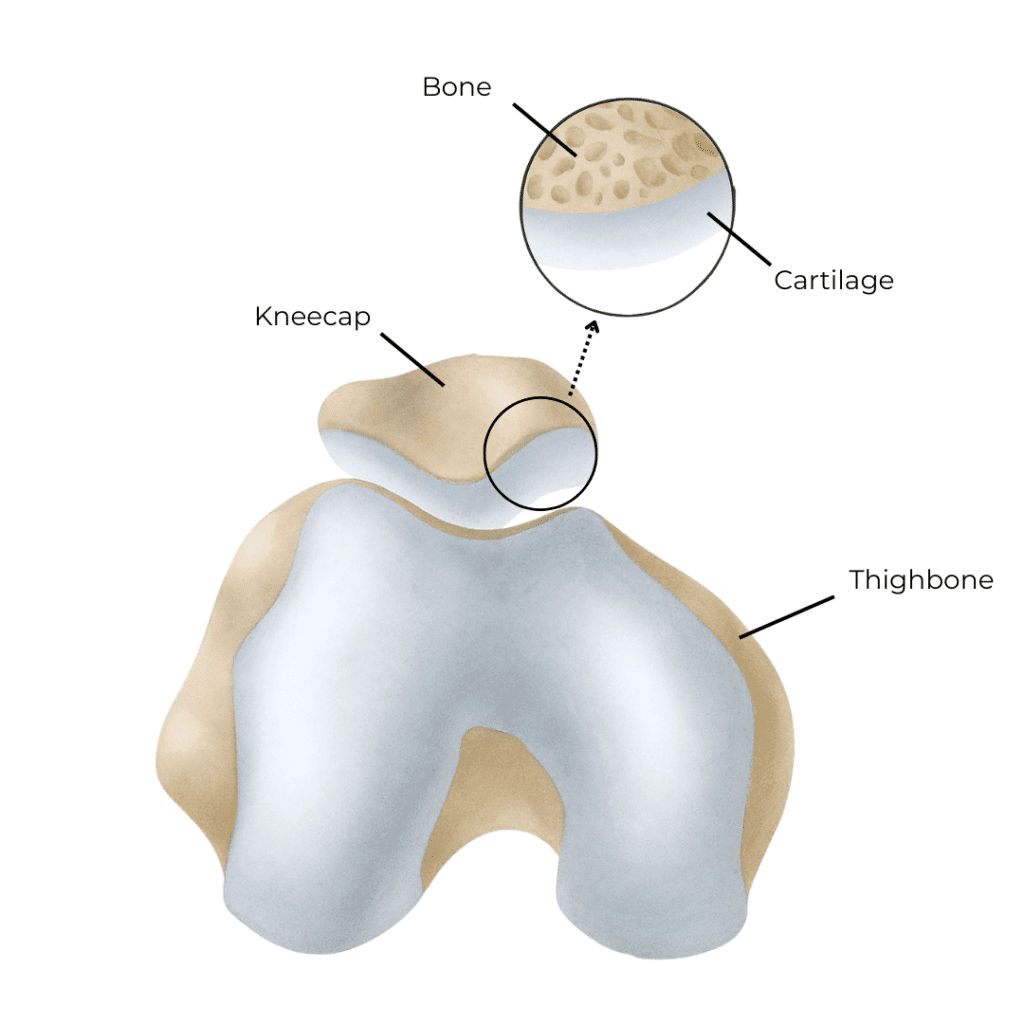
The Kneecap in Motion
When the kneecap is on track
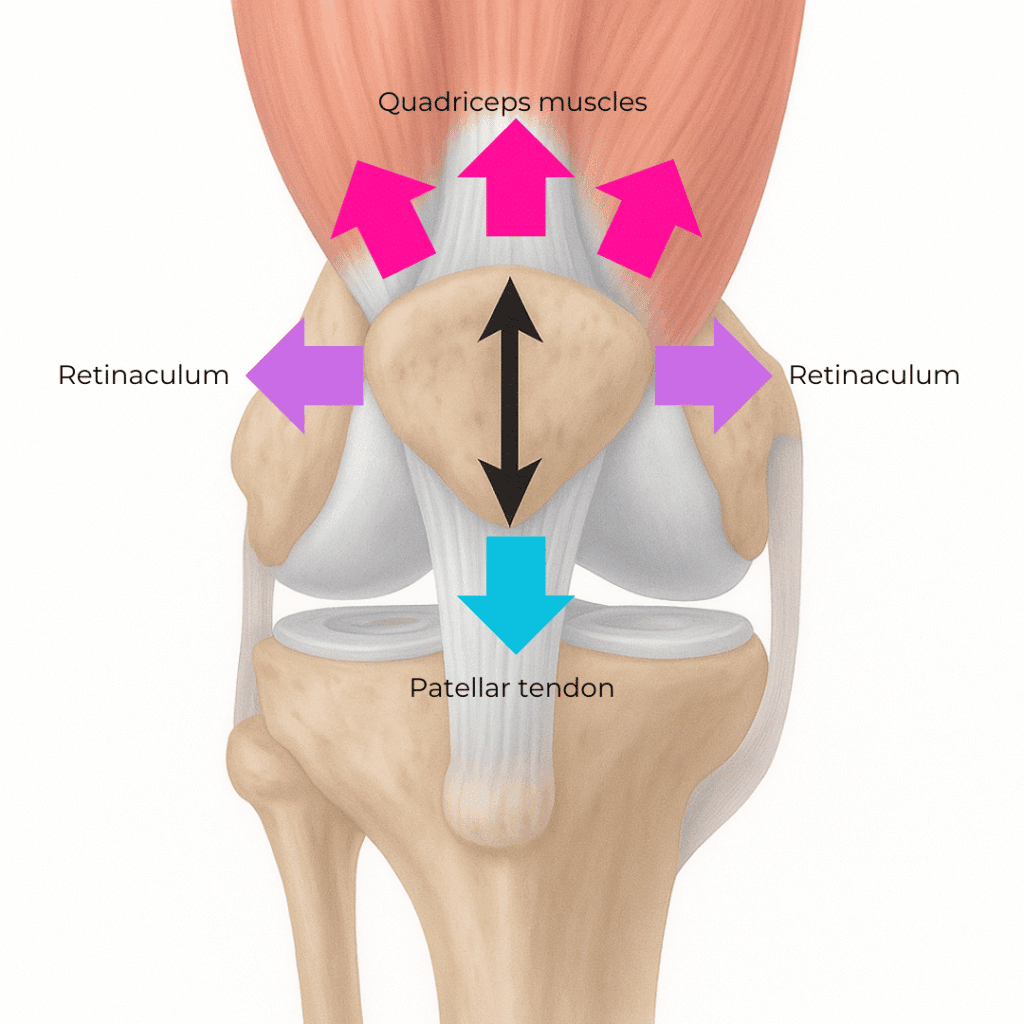
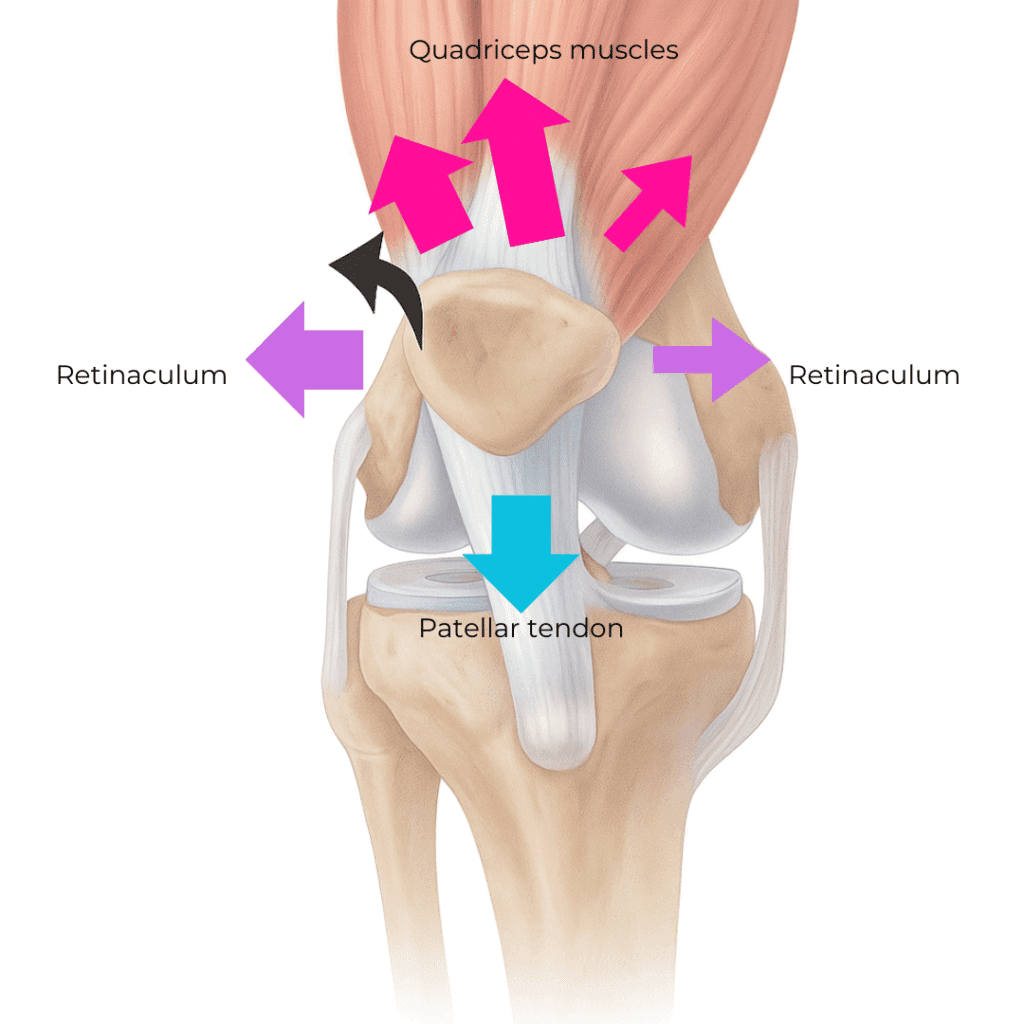
When the kneecap moves off track
Common Kneecap Problems

Cartilage Damage
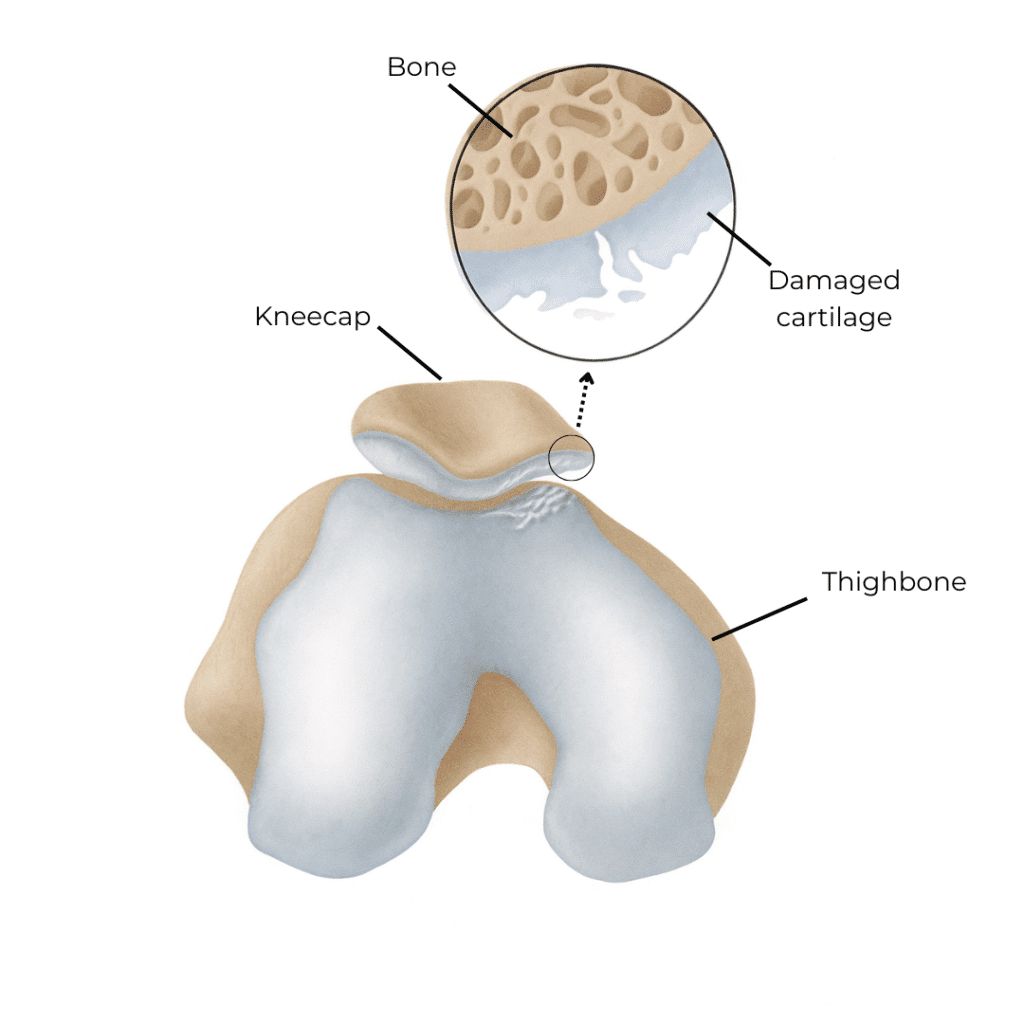

Dislocation
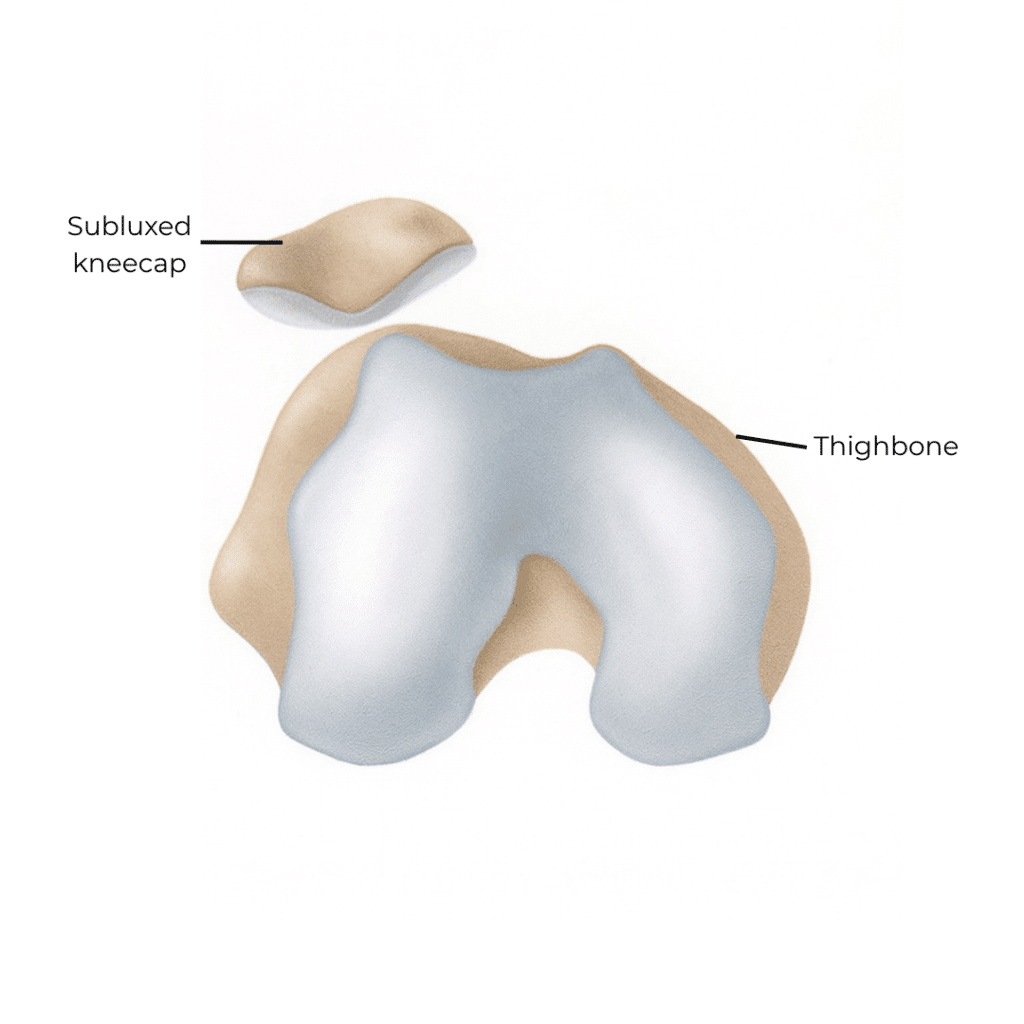
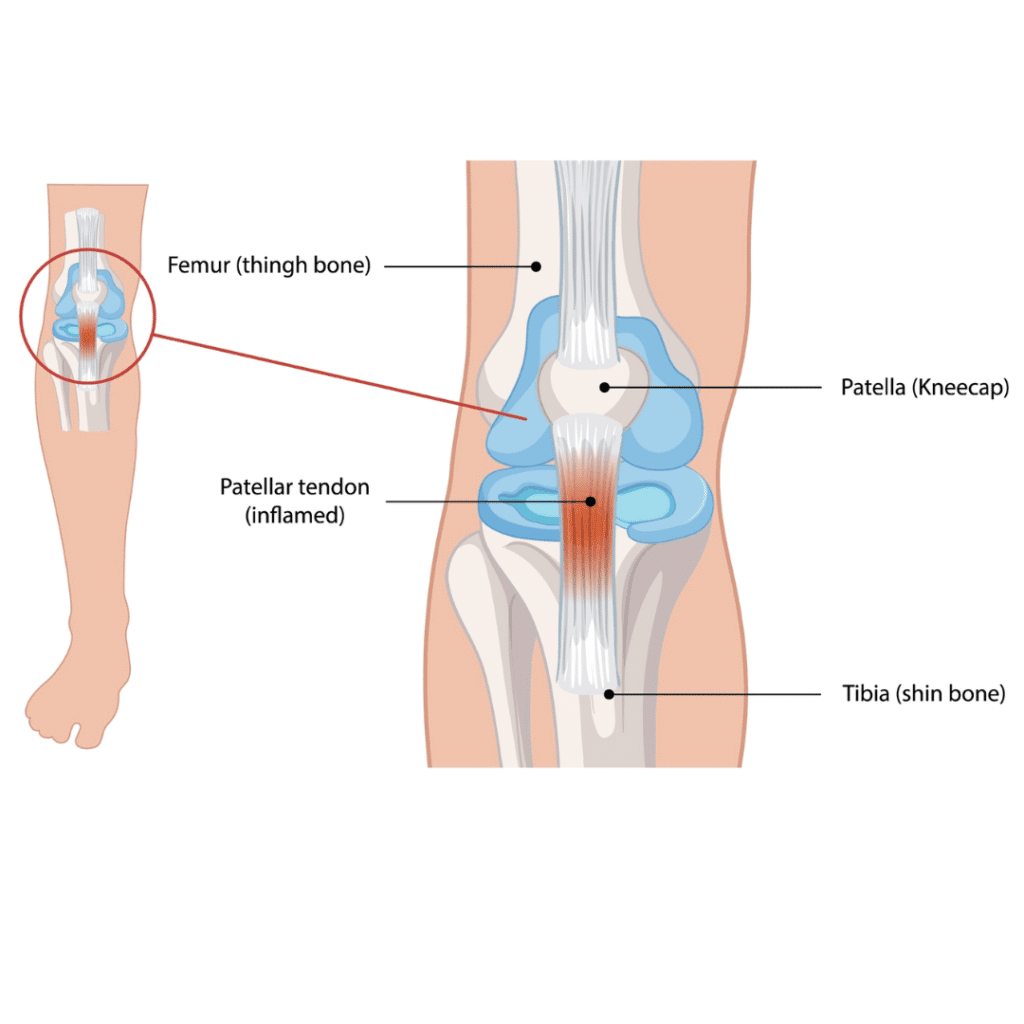
Patellar Tendinitis
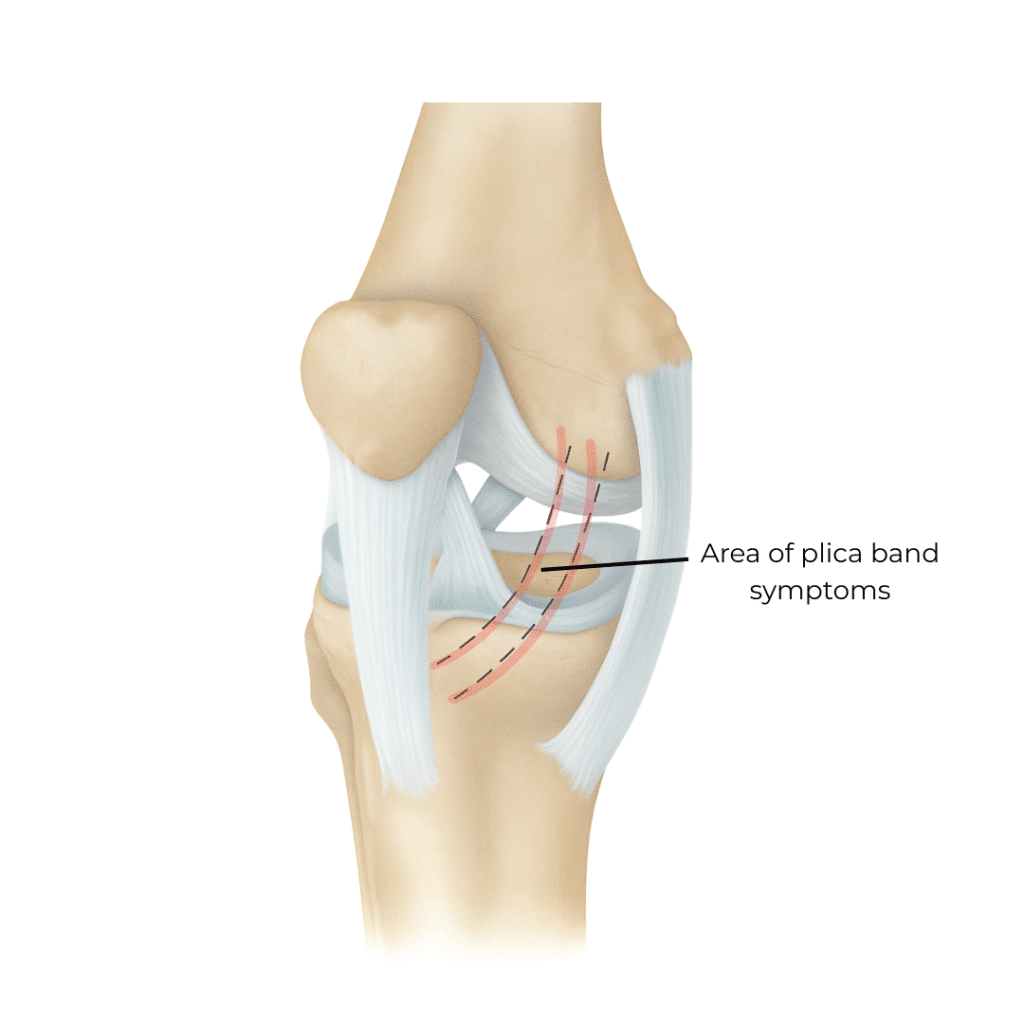
Plica Band Syndrome
Getting a Clear Diagnosis

Your Medical History
A Focused Knee Exam
Creating a simple pain map can help. Mark an X where you feel pain and an O where you notice mild discomfort. Bring that map to your visit so you can point out the exact areas that trouble you.Tests That May Be Used
Planning Your Treatment
Rehabilitation and the Physical Therapist's Role
Your Physical Therapy Exam
Your 3-Stage Rehab Program



Stage 1: Starting to Heal
Reducing Pain and Swelling
Improving Range of Motion
Developing Strong Muscles
Stage 2: Improving Your Knee's Function
Warming Up

Muscle-Loosening Stretches



Developing Strong Muscles





Stage 3: Practicing Everyday Moves
Relearning Daily Moves




Increasing Your Agility
From Rehab to Real Life
Kneecap Surgery
Kneecap Realignment
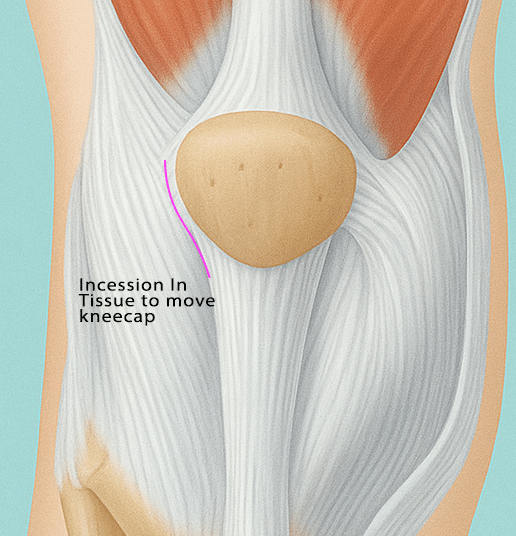
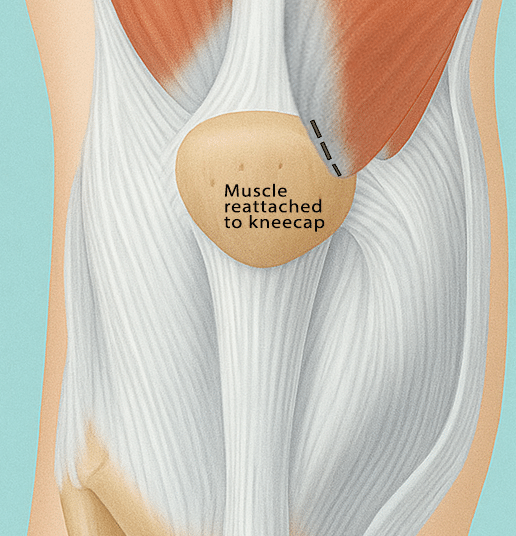
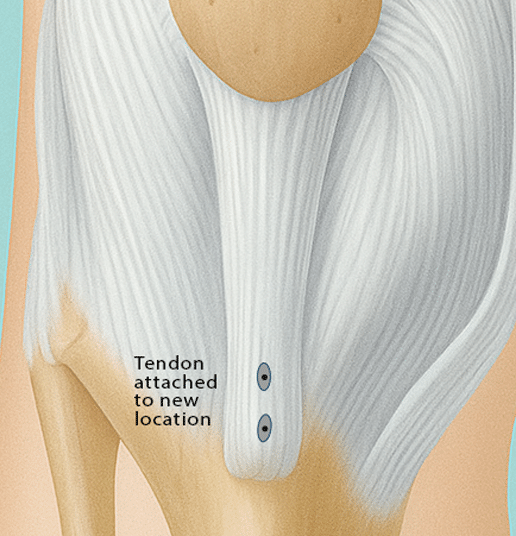
Cartilage Procedures


Recovering From Surgery
Quick Summary
© 2025 Princeton Orthopaedic Associates. The contents of PrincetonOrthopaedic.com are licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. Copying without permission is strictly forbidden. Privacy Policy | Accessibility