
Book An Appointment
Physician Assistants
Physical & Occupational Therapists
KneeMRI ScansNon-OperativePhysiatry
Physical Therapy
Podiatry
Spine
Sports Medicine
TraumaUrgent Care
X-Ray Imaging


The shoulder moves more than any other joint in your body, which makes it incredibly versatile but also vulnerable to injury. When the joint is pushed beyond its normal limits, it can become unstable, leading to pain and a lack of confidence in your arm. With the right diagnosis and a consistent treatment plan, most people can regain strength, stability, and full function. A stable shoulder perfectly balances freedom of motion with precise control. Bones, cartilage, ligaments, and tendons all work together, allowing you to reach, swing, and lift comfortably. Tendons connect muscles to bone, enabling movement, while ligaments connect bone to bone, providing support. The shoulder is a shallow ball-and-socket joint. The ball is the humeral head (the top of the upper arm bone), and the socket is the glenoid (part of the shoulder blade). A rim of tough, flexible cartilage called the labrum surrounds the glenoid, deepening the socket for a better fit. Smooth cartilage covers the ball to reduce friction. The joint capsule is a sleeve of ligaments that encloses the joint, connecting the humeral head to the glenoid. It is a static stabilizer, meaning it helps keep the ball centered in the socket at rest and during movement. The biceps tendon also attaches to the top of the glenoid and labrum, assisting with stability. The rotator cuff is a group of four muscles and their tendons that span from the shoulder blade to the humeral head. These tissues guide motion and keep the ball aligned in the socket. Because they actively control movement, they are known as dynamic stabilizers. Symptoms of instability often appear in specific arm positions, like reaching overhead or behind your back. You may notice: Instability frequently follows an injury that forces the ball out of the socket. A full slip is a dislocation, while a partial slip is a subluxation. Both can damage the labrum and stretch or tear the joint capsule. Your provider will gather a full picture of your symptoms to determine the cause of your instability. This includes a medical history, a focused shoulder exam, and imaging tests. Treatment aims to reduce pain and improve stability so you can use your arm safely. Plans often start with physical therapy and may include surgery if instability continues. Therapy focuses on strengthening the rotator cuff and the muscles around the shoulder blade. The goal is to improve dynamic stability and control, allowing your shoulder to move without slipping. Sticking with your program is key to achieving the best results. If therapy doesn't fully restore stability, or if you plan to return to high-demand activities, your surgeon may recommend surgery to repair the damaged tissues. The procedure often involves tightening the joint to prevent future slipping. Your team will discuss the potential for a slight loss of flexibility as a tradeoff for improved stability. If surgery is your best option, it will be performed at a hospital or surgical center. Your surgeon will choose the best approach for your specific injury. All surgeries carry some risk. Your team will work to minimize them, but potential issues include infection, anesthesia-related risks, injury to blood vessels or nerves, stiffness, and recurrence of instability. Following your post-operative instructions is critical for protecting the repair and ensuring proper healing. Contact your surgeon's office right away if you experience: Physical therapy after surgery is essential for restoring motion, strength, and function. Your therapist will guide you through a phased program, teaching you how to move safely and avoid stressing the repair. Only begin exercises when your surgeon or therapist says it is safe. Pendulum Exercise: Lean forward, supporting yourself with your non-injured arm. Let the injured arm hang down and use your body to create small, gentle swings in circles, forward-and-back, and side-to-side. Broom or Cane Stretch: Lie on your back holding a cane. Use your good arm to gently push the injured arm upward to a comfortable height. Hold briefly and return. Wall Walk: Stand facing a wall. Place your fingers on the wall and slowly walk them up as far as is comfortable. Hold, then walk them back down. Internal Rotation with Band: Secure an exercise band in a doorway. Stand with your injured side toward the door, elbow bent at 90 degrees and tucked at your side. Pull the band across your body. External Rotation with Band: Stand with your injured side away from the door, elbow bent at 90 degrees and tucked at your side. Pull the band away from your body. Wings: Stand tall with your arms at your sides. Keeping your elbows straight, slowly lift your arms out to the sides toward shoulder level. Lower with control. Use this list to prepare for your procedure and a smooth recovery.Understanding and Treating Shoulder Instability

Key Steps in Your Recovery
How a Healthy Shoulder Works
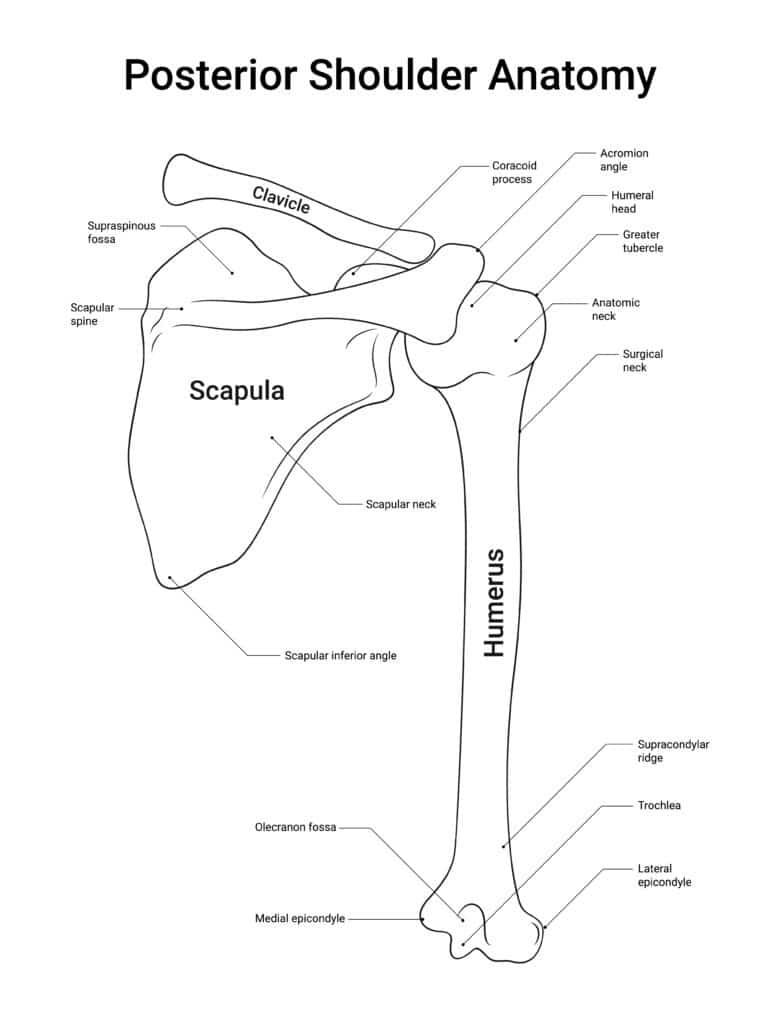
Bones and Cartilage
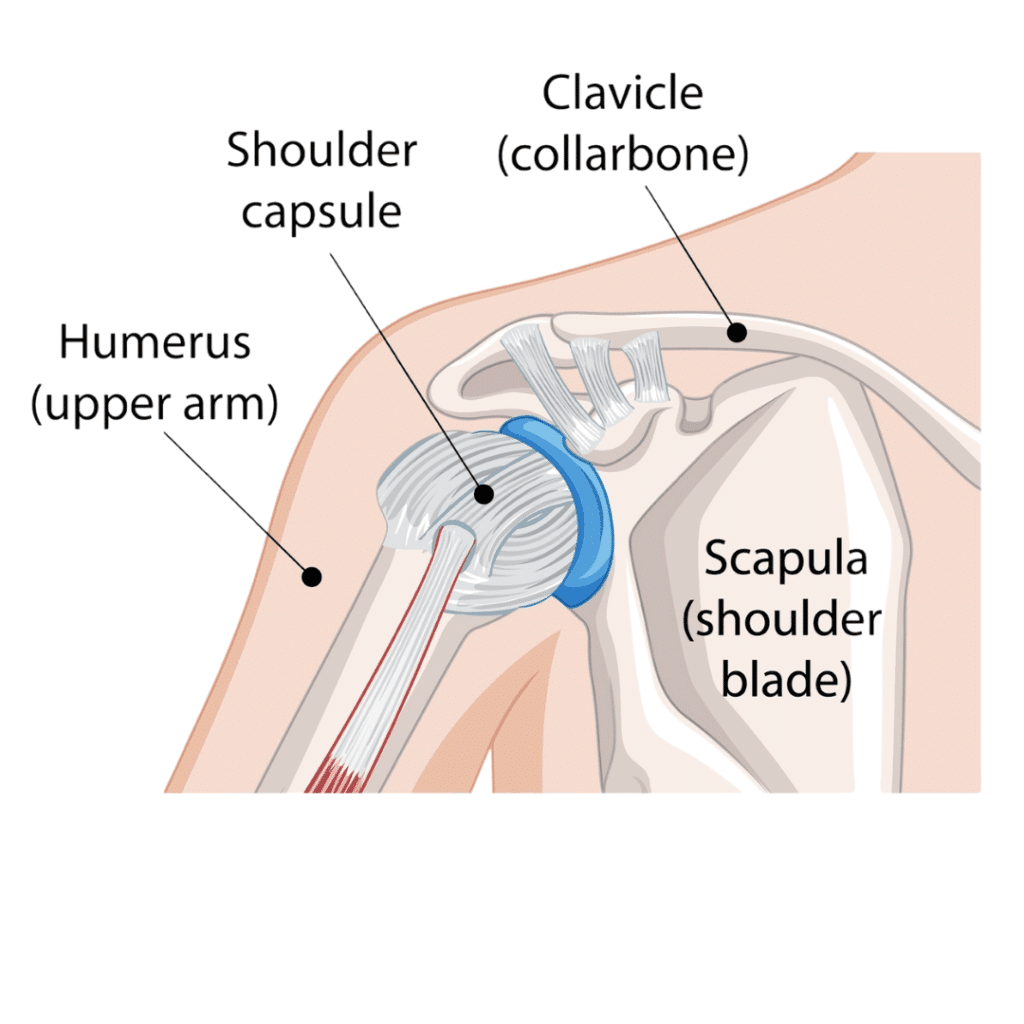
The Capsule and Other Stabilizers
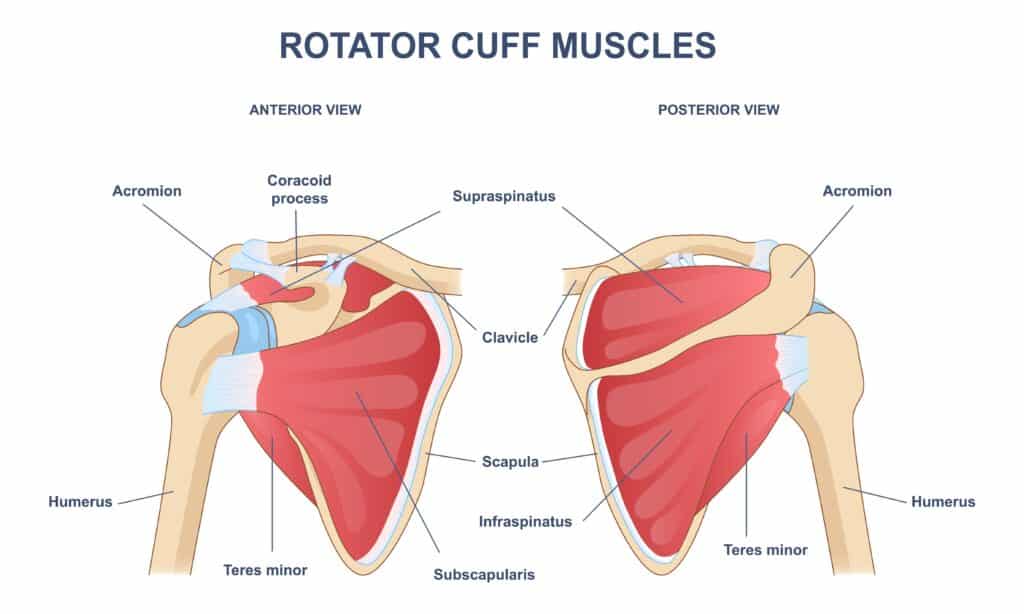
The Rotator Cuff
Signs and Causes of Shoulder Instability

What Makes a Shoulder Unstable?
Common Structural Injuries
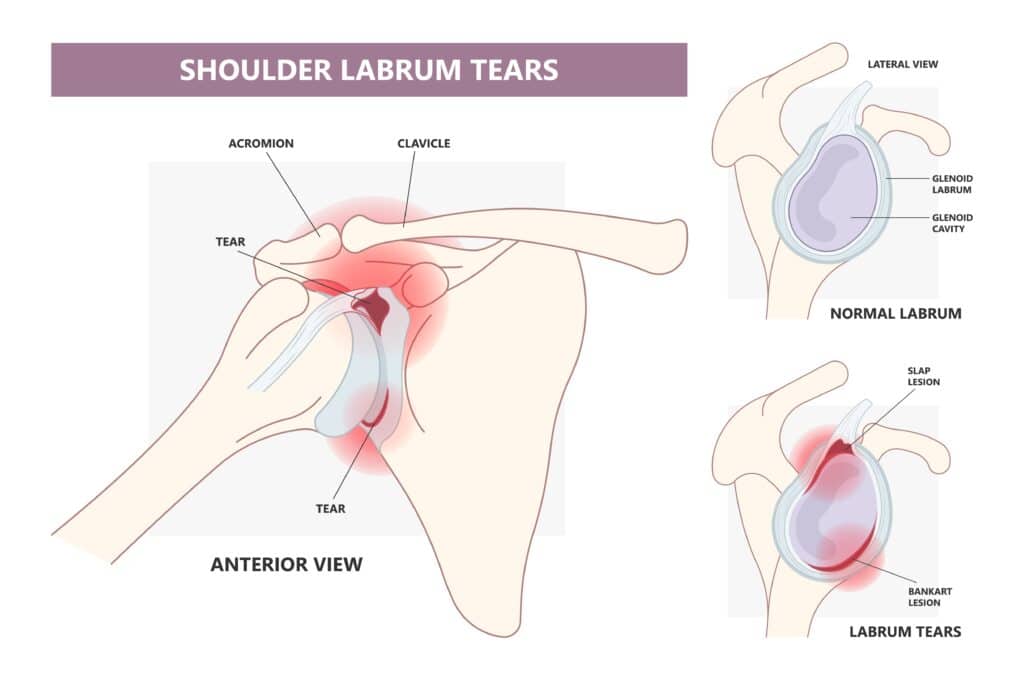
Getting a Diagnosis
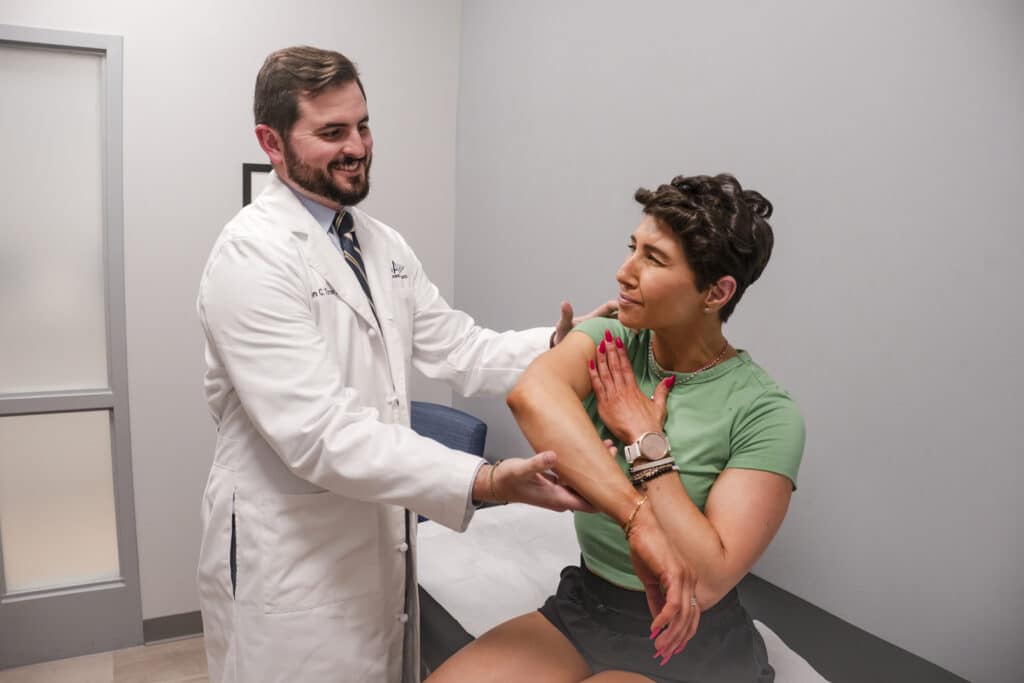
Building Your Treatment Plan
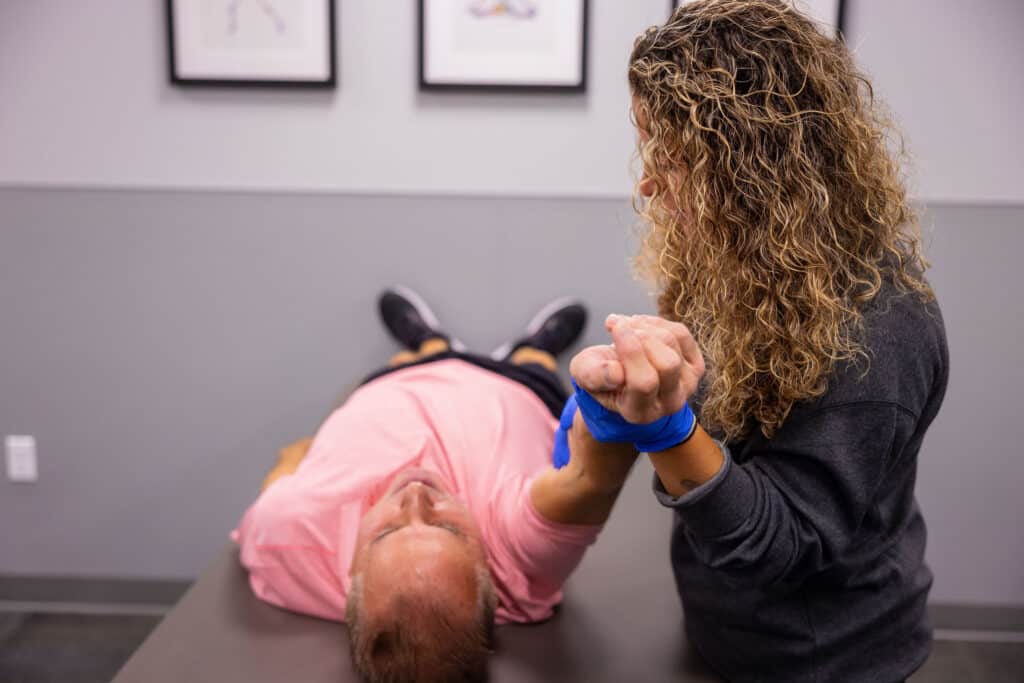
Physical Therapy
Surgery
What to Expect with Surgery
Common Surgical Repairs
Repairing a SLAP Tear
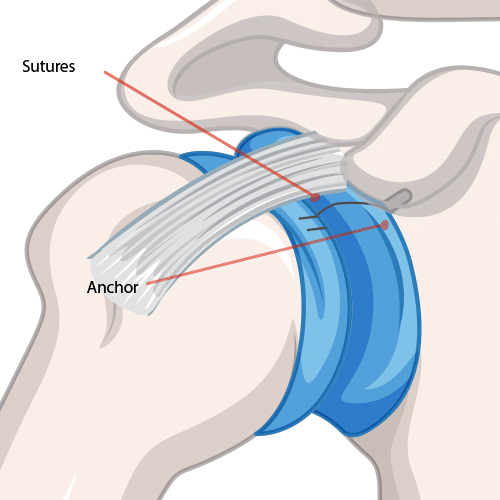
Repairing a Bankart Tear
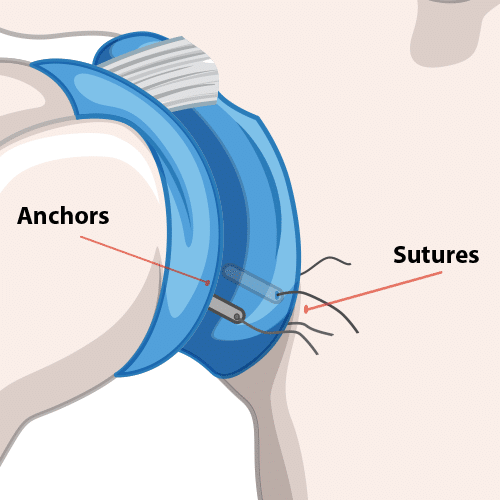
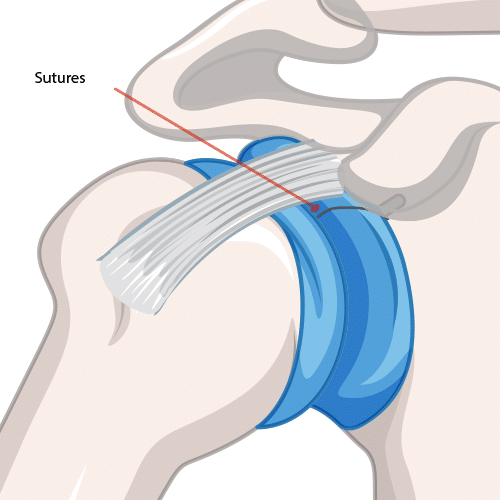
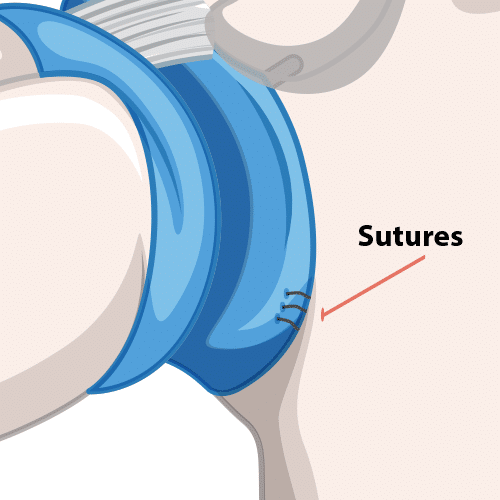
Open Repair
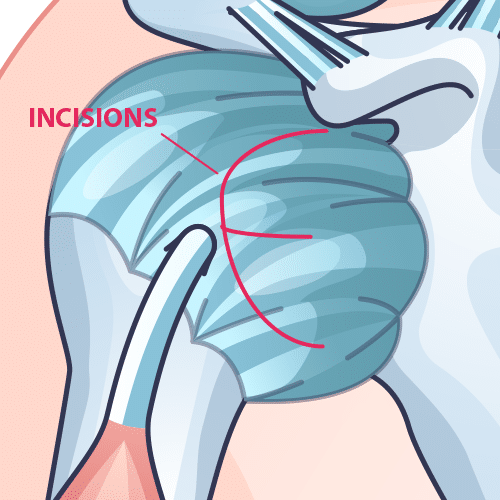
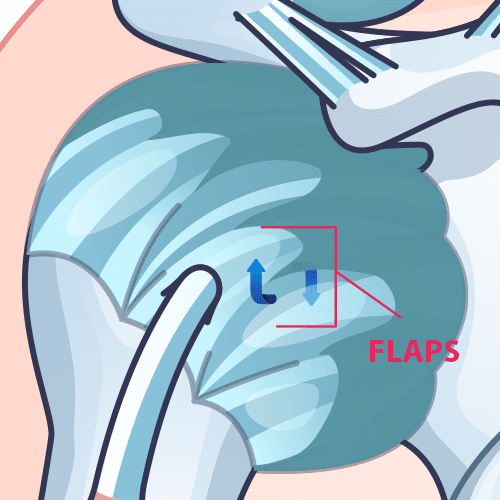
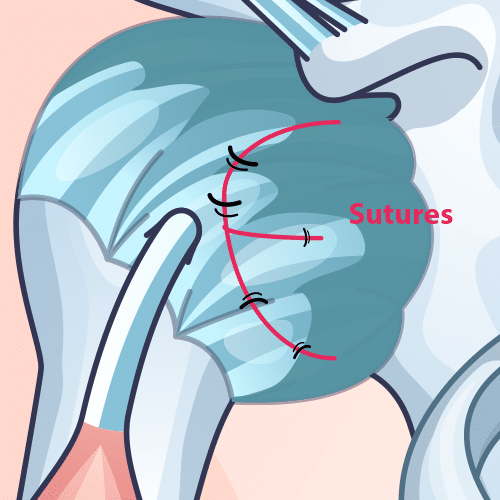
Arthroscopic Repair

Possible Risks and Complications
Your Recovery After Surgery
At Home Care
When to Call Your Surgeon

Rehabilitation and Exercises
Early Motion Exercises
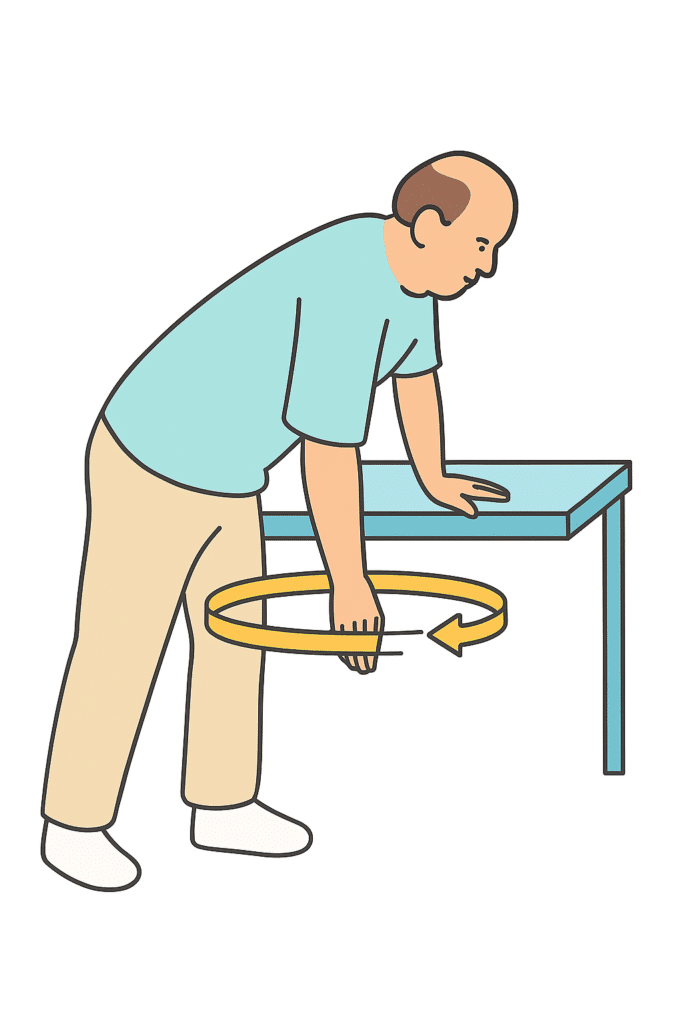


Strengthening Exercises
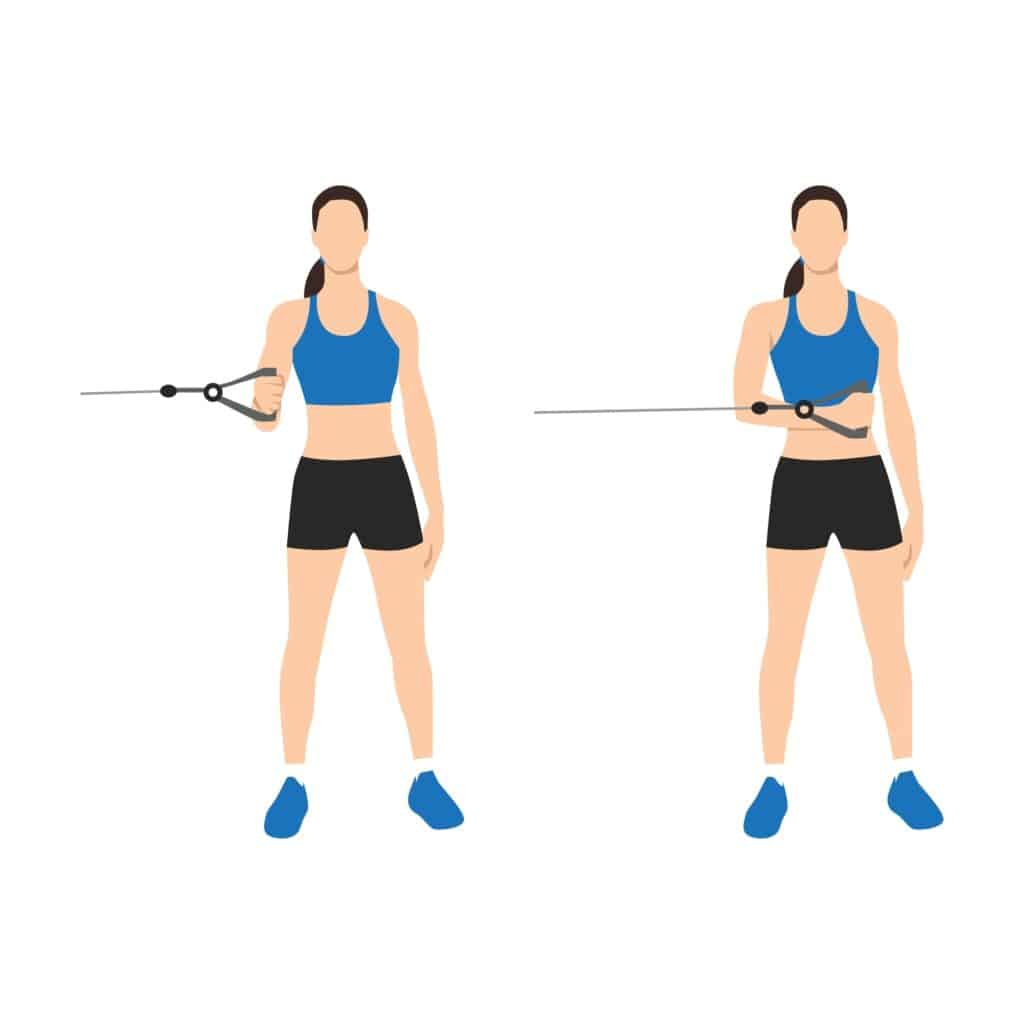
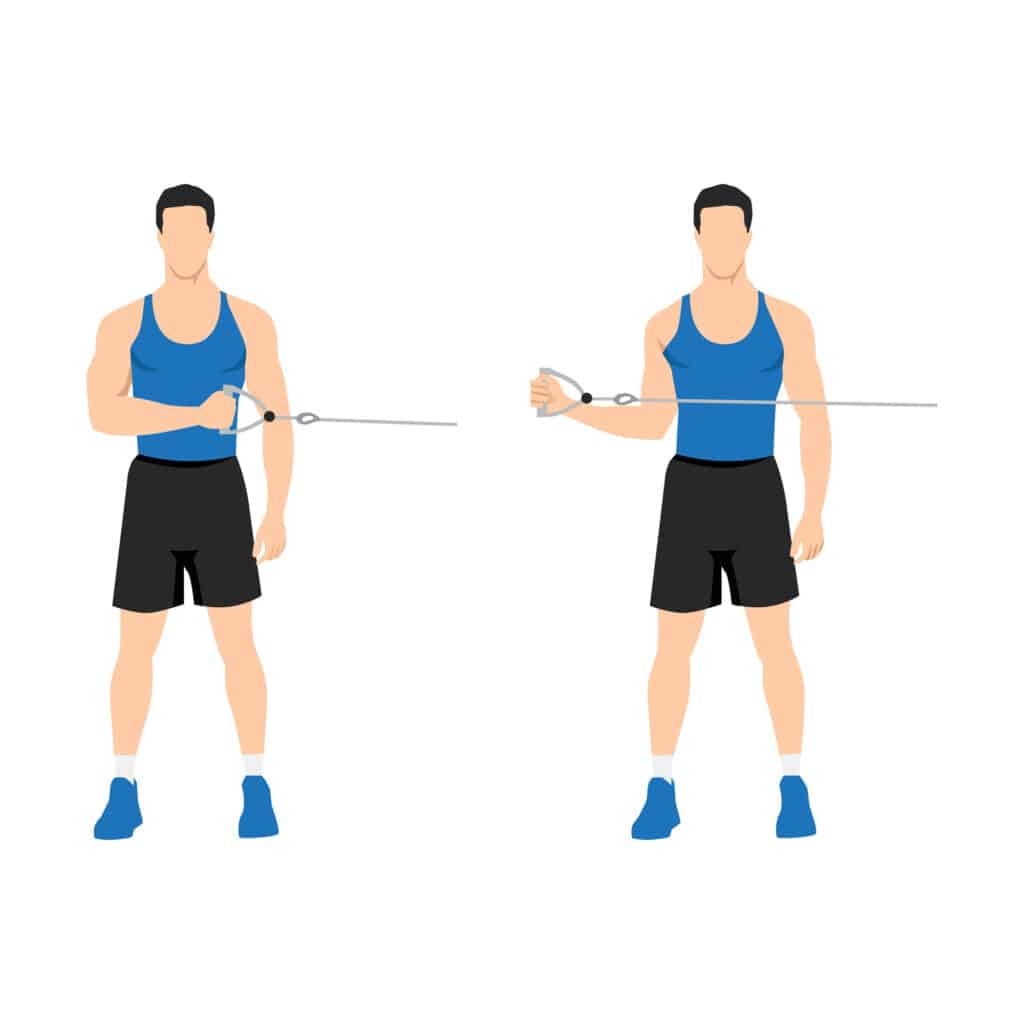

Surgery Checklist
Before Surgery
After Surgery
© 2025 Princeton Orthopaedic Associates. The contents of PrincetonOrthopaedic.com are licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. Copying without permission is strictly forbidden. Privacy Policy | Accessibility