
Book An Appointment
Physician Assistants
Physical & Occupational Therapists
KneeMRI ScansNon-OperativePhysiatry
Physical Therapy
Podiatry
Spine
Sports Medicine
TraumaUrgent Care
X-Ray Imaging

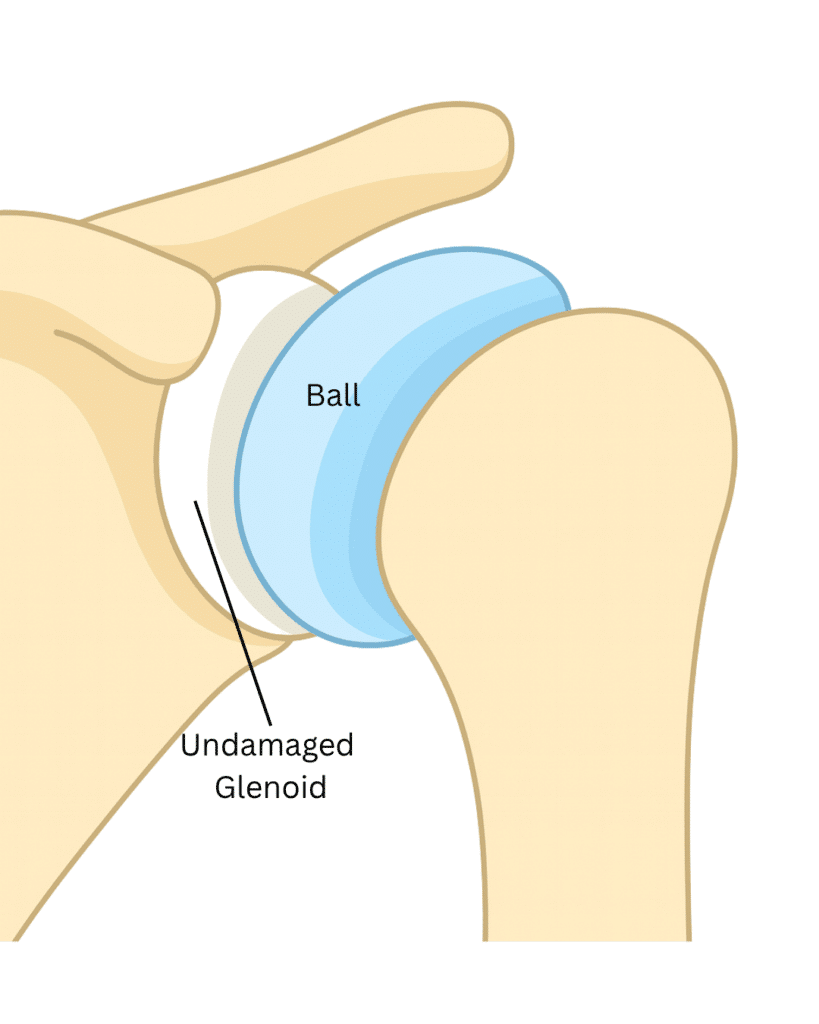
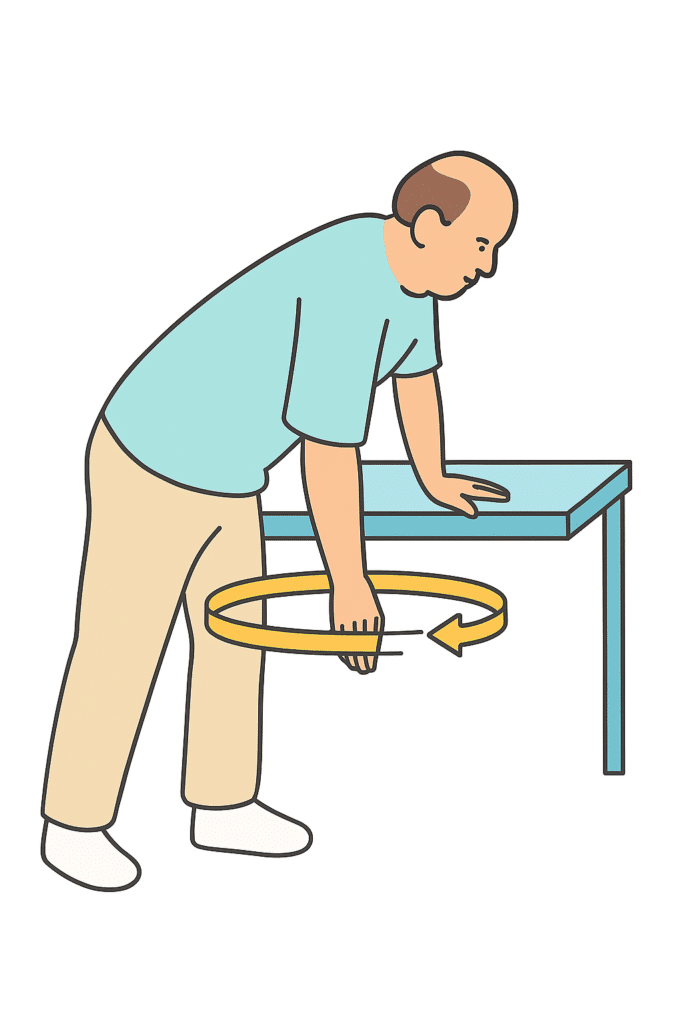
Shoulder replacement surgery removes damaged parts of the joint and replaces them with an artificial joint, called a prosthesis. This procedure is designed to ease pain and help you use your arm more comfortably. It has a strong track record for safety and reliable outcomes when paired with good preparation and rehabilitation. An orthopedic surgeon, a specialist who treats bone and joint conditions, will recommend surgery only if it aligns with your long-term needs. Be open about your daily activities, goals, and concerns so your care plan can be tailored to fit your life. The most common reason for shoulder replacement is arthritis, which occurs when the smooth cartilage cushioning the joint wears away. As cartilage breaks down, bone rubs on bone, causing the joint to become stiff and painful. Common causes include: Other conditions can also harm the joint. A severe fracture can shatter the ball of the shoulder (humeral head). Avascular necrosis occurs when the bone loses its blood supply, which can cause the bone to die and collapse. The shoulder is a ball-and-socket joint. The rounded top of your upper arm bone (the humeral head) fits into a shallow cup on your shoulder blade (the glenoid). This design allows a wide range of motion for lifting, reaching, and rotating. Cartilage, a smooth, rubbery layer, covers the ball and lines the socket, letting the joint glide without friction. The rotator cuff—a group of four muscles and their tendons—keeps the joint stable and powers your arm movements. With osteoarthritis, cartilage cracks and thins, causing bone surfaces to become rough. This can lead to bone spurs, grinding, and stiffness. Inflammatory arthritis can make the joint warm, swollen, and painful. A large rotator cuff tear can allow the joint to slip out of position, damaging cartilage and causing persistent pain. In cases of avascular necrosis, the lack of blood flow leads to bone collapse. Osteoarthritis is joint wear and tear. Cartilage cracks and thins, and bone rubs on bone. This leads to roughened bone and growths called bone spurs. The joint is stiff and painful. It may catch when it moves. Inflammatory (rheumatoid) arthritis is a chronic joint disease. Cartilage is slowly destroyed. The joint becomes warm, swollen, and painful. Over time, the joint may stiffen and weaken. A shoulder fracture can occur due to trauma, such as a car crash or bad fall. The ball may break off or end up in pieces. Avascular necrosis occurs when the blood supply to the bone is cut off. Without blood, the bone dies and collapses. A large rotator cuff tear lets the joint slip out of place. This can lead to cartilage damage and weakness and pain in the joint. Your surgeon will examine your shoulder, review your medical history, and order imaging tests such as X-rays, a CT scan, or an MRI to get a detailed look at your bones and soft tissues. These findings guide the best treatment plan for you. Nonsurgical options are often tried first, including rest, anti-inflammatory medicines, cortisone injections, and physical therapy. If these treatments no longer provide relief and your quality of life is affected, your surgeon may recommend shoulder replacement. Being an informed partner in your care is crucial. Ask questions to understand your options, including the benefits, risks, and limitations of the procedure. Discuss your goals and which activities may need to be modified after surgery. You may need lab tests, a chest X-ray, and an ECG to confirm you are ready for surgery. Work with your primary care provider to manage any health issues like diabetes or high blood pressure. Be sure to treat any active infections before your surgery date. Tell your surgeon about all medicines and supplements you take. You will likely need to stop taking blood thinners, aspirin, and anti-inflammatory drugs (like ibuprofen) before surgery to reduce bleeding risk. Also, finish any necessary dental work to prevent bacteria from traveling from your mouth to your new joint. After surgery, you will wear a sling and have limits on lifting and reaching. A little planning can make your home safer and more comfortable. On the day of surgery, follow your team's instructions about when to stop eating and drinking. At the hospital, you will meet your anesthesiologist to discuss the plan to keep you comfortable, which often includes general anesthesia and a nerve block to numb your arm for pain control during and after the procedure. You and your surgeon will choose the implant that best matches your anatomy and condition. Anatomic shoulder prosthesis replaces the head of the arm bone (humeral head) with a metal ball attached to a stem. The stem fits into the arm bone. If needed, a plastic cup is placed onto the shoulder socket. A reverse prosthesis may be used for certain injuries or conditions. The humeral head is replaced by a metal and plastic socket attached to a stem. A metal ball is placed onto the shoulder socket. Reverse replacement: For rotator cuff arthropathy or other conditions, a reverse prosthesis may be used. For this, the humeral head is removed and a stem topped by a plastic cup is put into the arm bone. A metal ball is placed over the glenoid. After surgery, arm muscles other than the rotator cuff can take over moving and stabilizing the joint. Total replacement: If both the humeral head and glenoid are worn, both the ball and the socket may be replaced. For this, the humeral head is removed. The stem is placed into the arm bone and the metal ball secured to it. The plastic cup is secured in place on the glenoid. Partial (hemi) replacement: If the humeral head is damaged but the glenoid is not, only the ball may be replaced. Most often, the humeral head is removed. The stem is placed into the arm bone and a metal ball is secured to the stem. In certain cases, the natural head stays in place and is covered with a metal cap. After surgery, you will wake up in the recovery area with your arm in a sling. Some patients go home the same day, while others stay one night. Your shoulder will be swollen and bruised, and your care team will manage your pain with medication. To help prevent blood clots, you will be encouraged to move your ankles and feet and may wear compression boots. A physical therapist will show you how to perform gentle exercises, such as pendulum swings, to begin restoring motion while protecting the new joint. Your active participation is key to a successful recovery. Follow your team's instructions carefully. The pendulum is an exercise you may learn soon after surgery. Do this exercise as often as your therapist prescribes. To do it: Stand next to a table or other support. Bend slightly forward and hold on to the support with the hand of your unoperated arm. Let your operated arm hang down. Slowly swing the arm in a circle. Contact your surgeon's office immediately if you experience: Call 911 for any signs of a medical emergency, such as chest pain or difficulty breathing. Do not drive until your surgeon clears you to do so, and never drive while taking opioid pain medication. Your return to work will depend on the physical demands of your job. Let all healthcare providers, including your dentist, know you have a shoulder replacement. You may need to take antibiotics before certain procedures to prevent infection. With proper care and by avoiding high-impact activities, your new shoulder can provide you with years of pain relief and improved function. Shoulder replacement can relieve pain and help you return to the activities you enjoy. By sharing your goals with your team and taking an active role in your care, you can work toward the best possible result.Your Guide to Shoulder Replacement Surgery

Quick-Start Checklist
What is Shoulder Replacement Surgery?

Why a Shoulder May Need Replacement
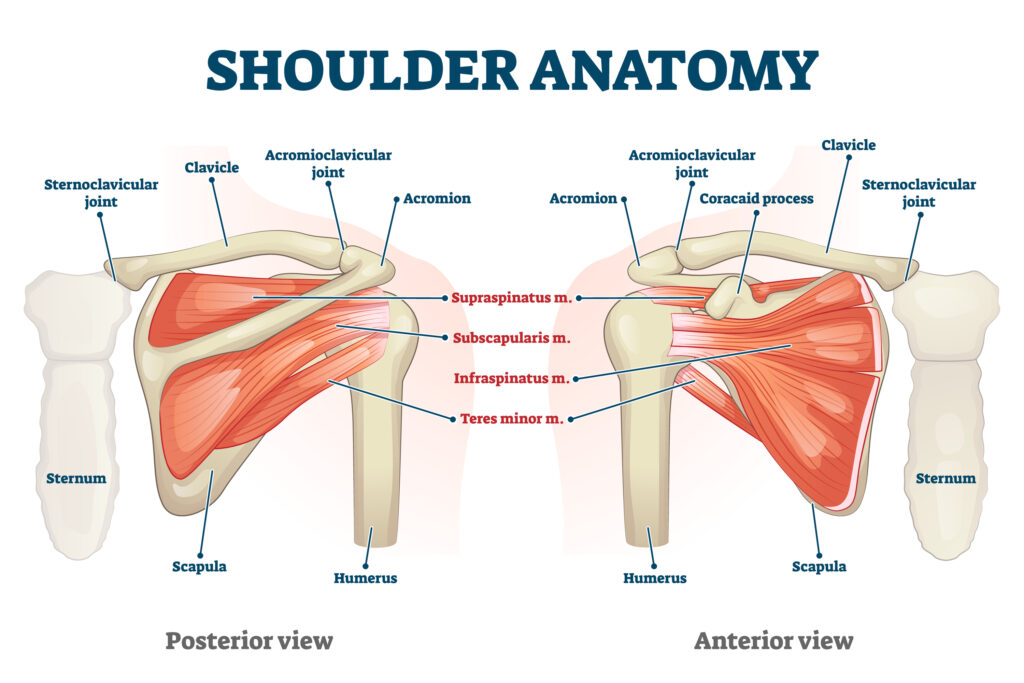
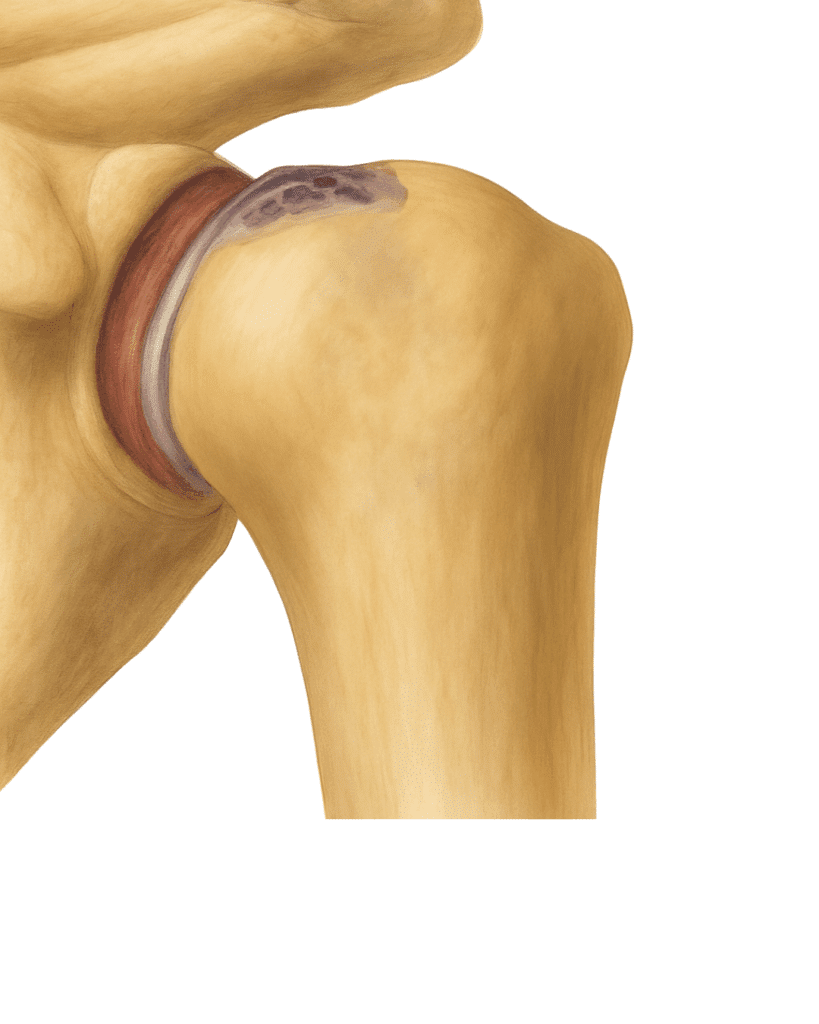
Understanding How Your Shoulder Works
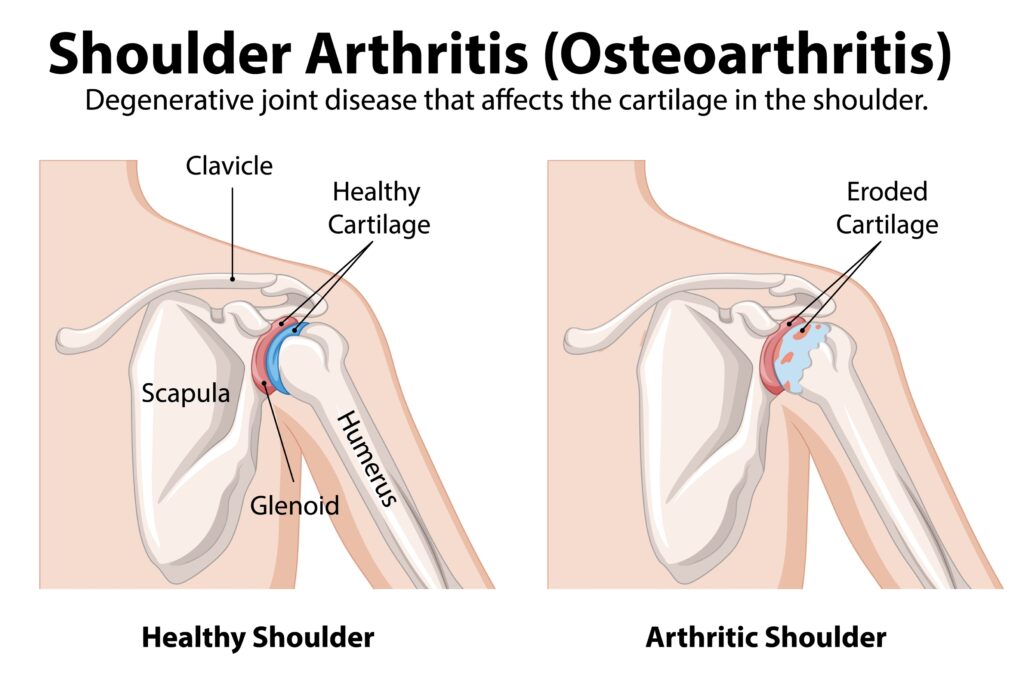
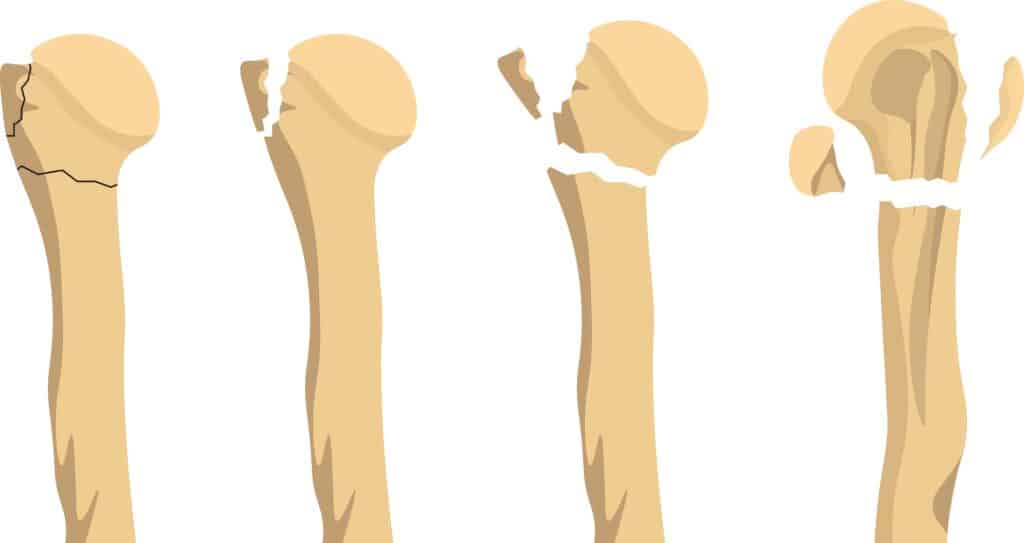
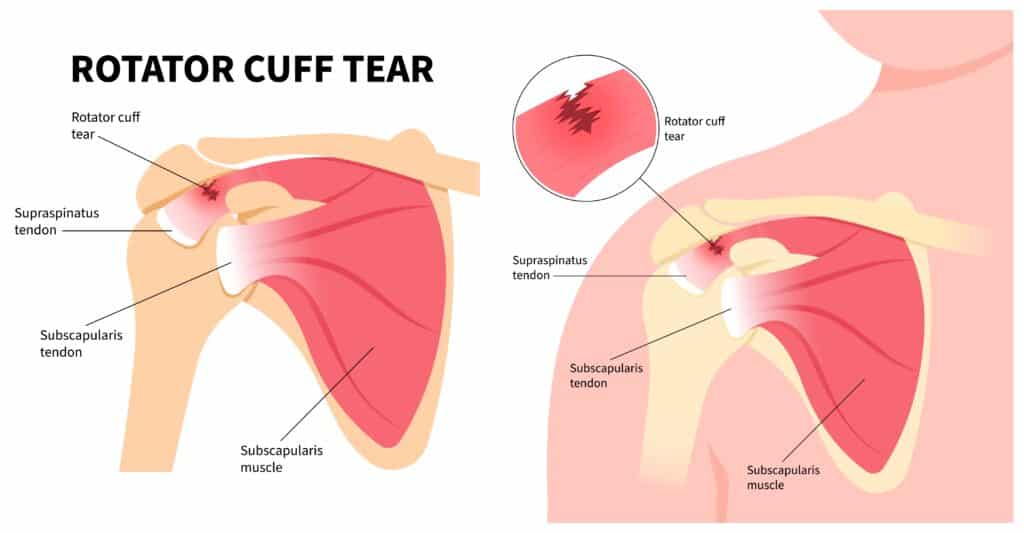
When the Shoulder is Damaged
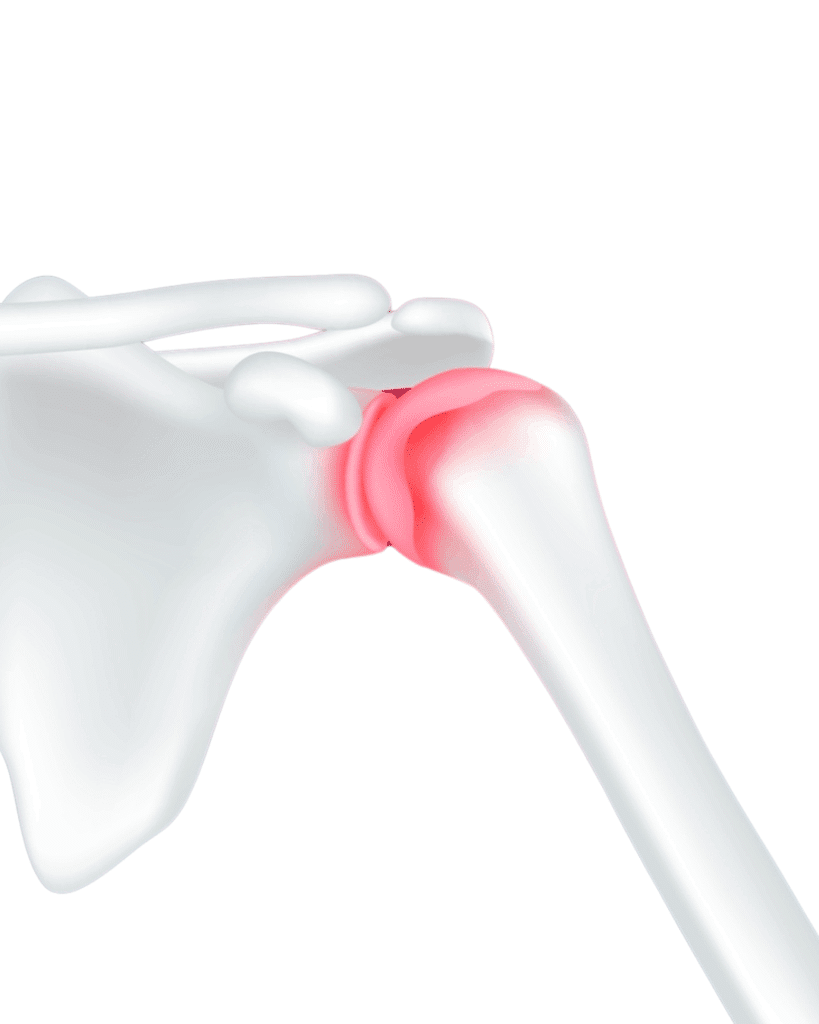
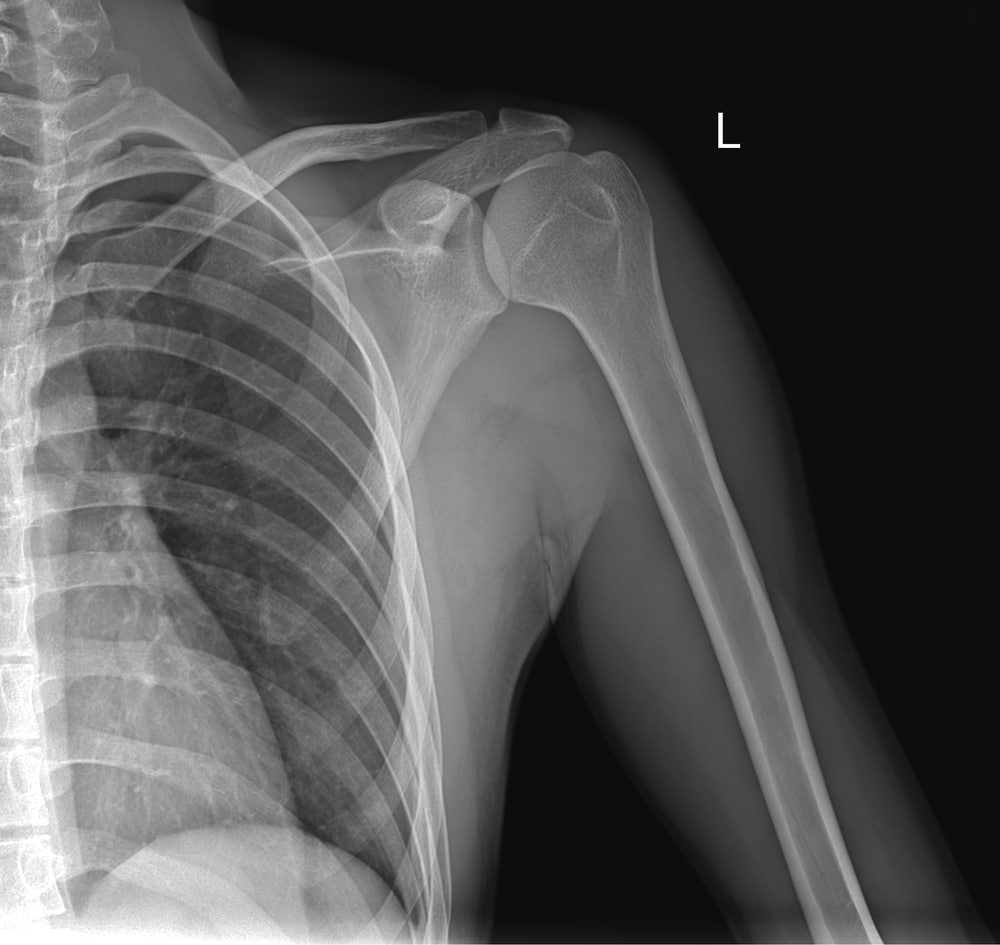
Is Surgery the Right Choice for You?
Benefits You Can Expect
Risks and Possible Complications

Preparing for Your Surgery
Prepare Your Home and Support System
The Surgical Procedure
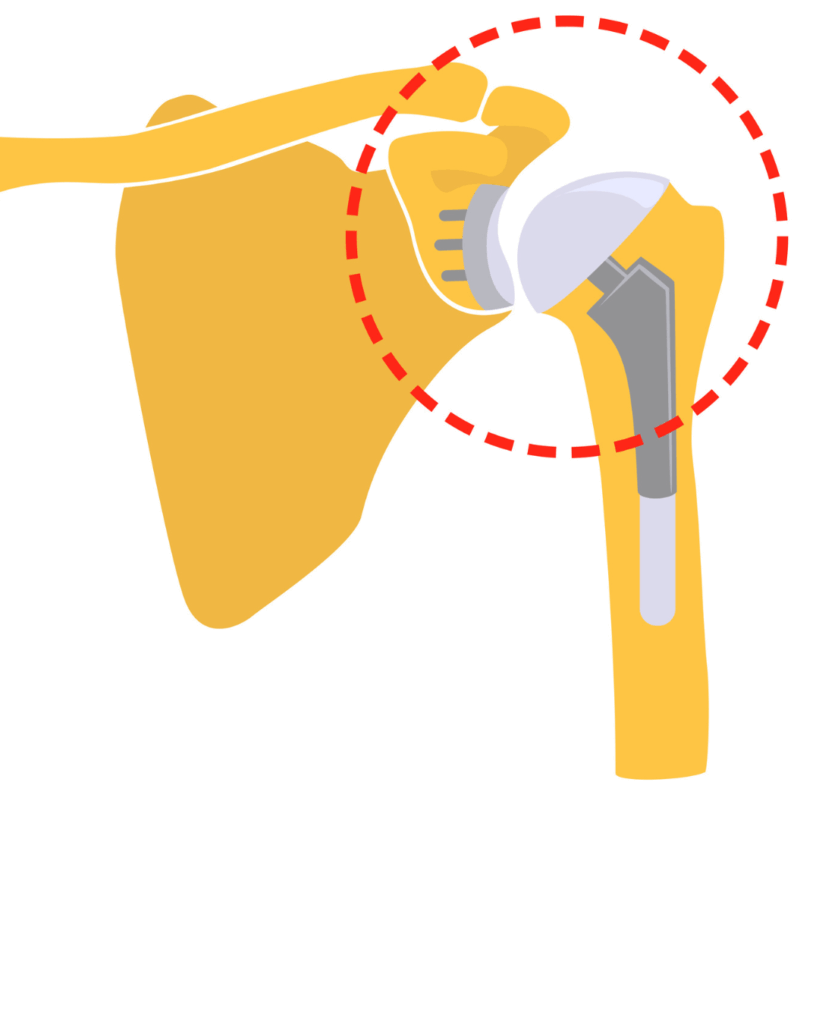
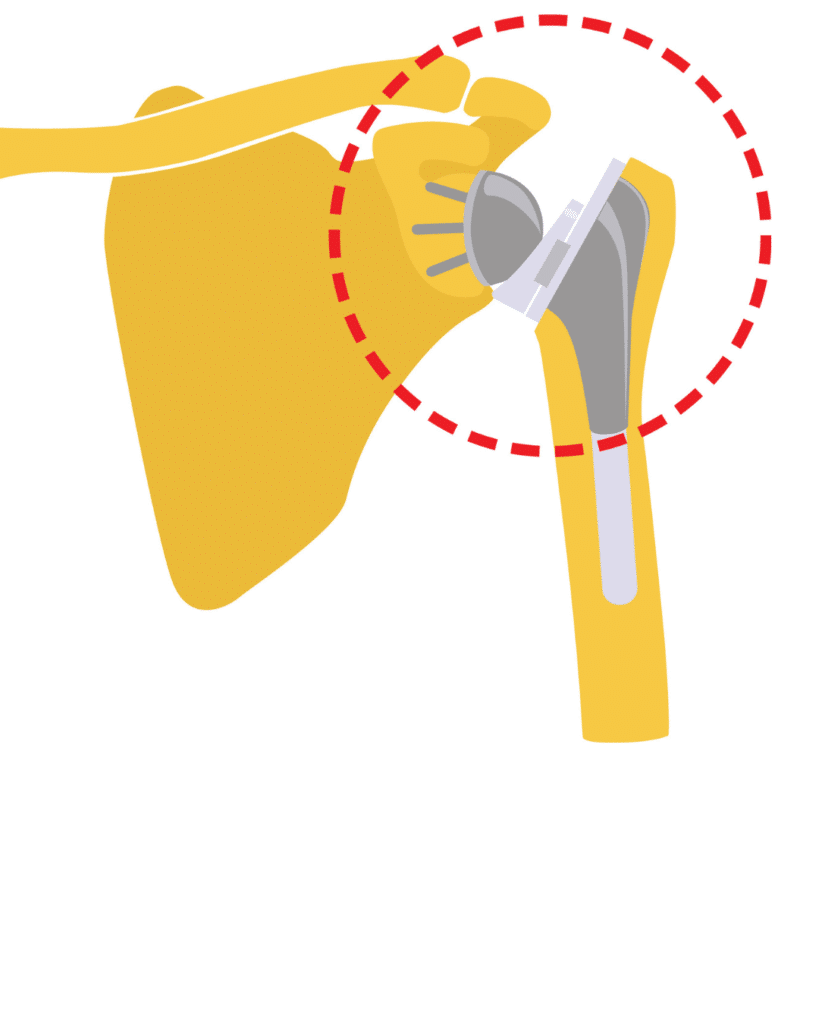
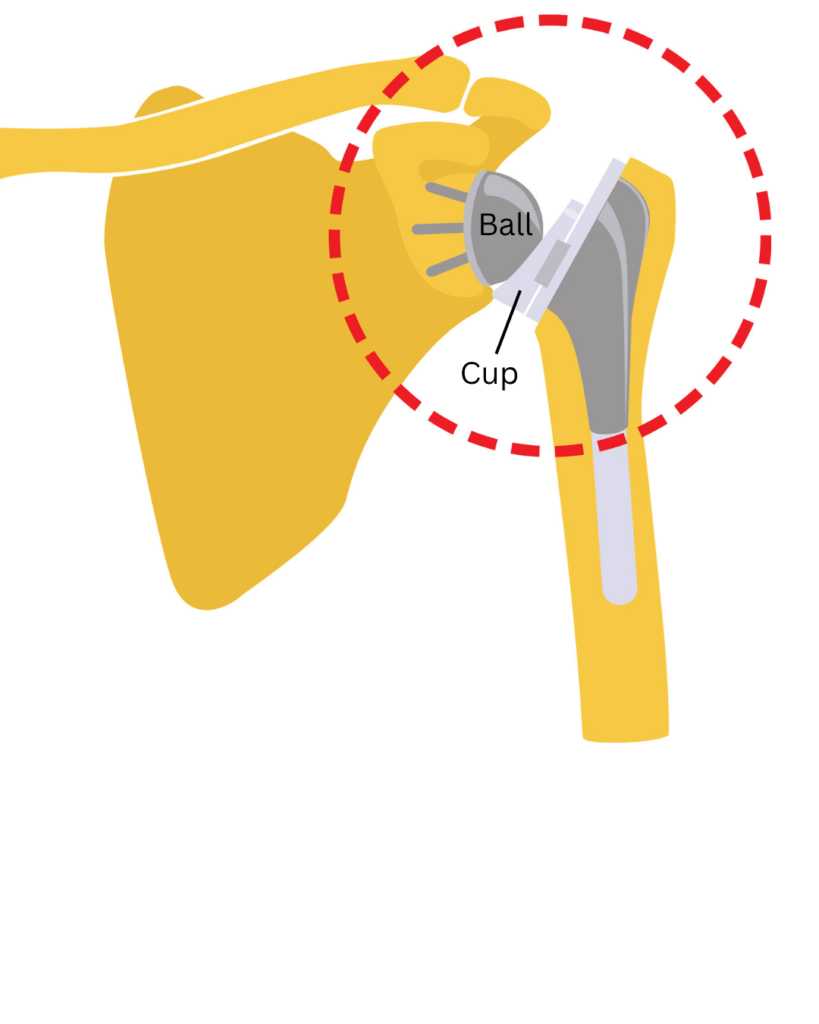
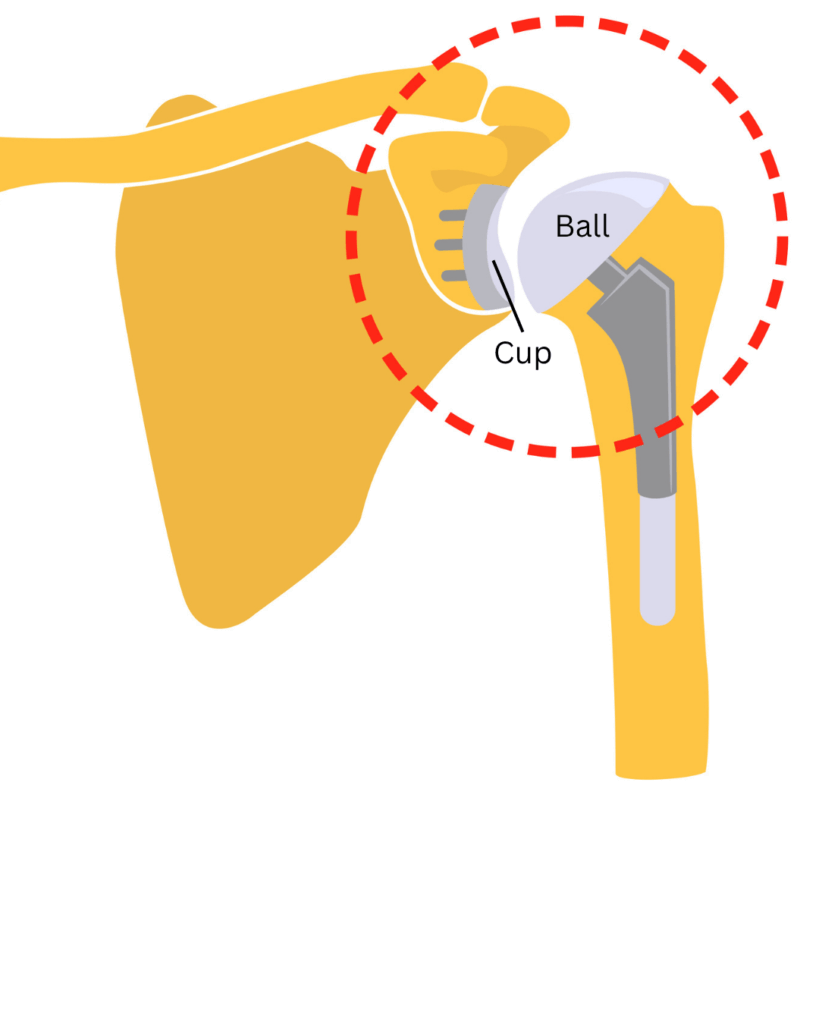
Your Implant Options
Your Recovery Journey

Recovering at Home
When to Call Your Surgeon
Living Well with Your New Shoulder

Quick Summary
© 2025 Princeton Orthopaedic Associates. The contents of PrincetonOrthopaedic.com are licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. Copying without permission is strictly forbidden. Privacy Policy | Accessibility