
Book An Appointment
Physician Assistants
Physical & Occupational Therapists
KneeMRI ScansNon-OperativePhysiatry
Physical Therapy
Podiatry
Spine
Sports Medicine
TraumaUrgent Care
X-Ray Imaging

This information is provided as-is and is not medical advice. If you are curious about an orthopaedic consult, please contact us.
Osteoarthritis (OA) is the most prevalent kind of arthritis. It's a distressing disease that results from wear and tear of cartilage inside a joint over time. The majority of this deterioration is caused by usage over many years, with people developing it when they reach age 50 or older. Younger individuals, on the other hand, may develop the condition early as a result of a joint injury. Osteoarthritis of the hand is also known as post-traumatic arthritis. It occurs after a trauma, such as a fracture, dislocated shoulder, or torn rotator cuff.
Wearing causes damage and eventual degeneration of the cartilage that covers the bones where they join in the joint. Because bone begins to rub directly against bone, this loss of protective cartilage results in osteoarthritis, which causes an inflammation of the joints.
Cartilage is a rubbery, sponge-like tissue that covers the ends of bones where they come together to form joints. Cartilage in elbows, knees, shoulders, ankles, and knuckles serves as a shock absorber cushioning the bones and preventing their ends from clashing during movement. It allows for a lot of twisting, bending, turning, and movement. The cartilage in our joints deteriorates with age – especially those joints that we use the most. It's similar to how automobile brake pads wear down with time. When cartilage degeneration occurs, the bones aren't adequately cushioned, leading to damage in the joint.
Osteoarthritis most often affects big weight-bearing joints, such as the hips or knees. The following are the most common joints that suffer from osteoarthritis:
Pain is the most common OA symptom, followed by stiffness. Pain typically gets worse during activity and improves with rest. Some people with OA, on the other hand, may experience a sense of stiffness in the morning or after lengthy periods of inactivity.This symptom (also known as "gel phenomenon" or "gelling phenomenon") is caused by a brief thickening (or "gelling") of natural fluids within the joint. When a person resumes activity, it generally subsides in less than 20 minutes.
Crepitus is a cracking or grinding sound that may be heard when the joint is moved. Some patients with OA experience little or no pain for unknown reasons. The intensity of each person's pain may vary depending on a variety of factors such as: the disease's stage and how a person's brain processes pain messages, as well as cultural, gender, and psychological differences.
The following are the three essential elements to obtaining a correct diagnosis for osteoarthritis:
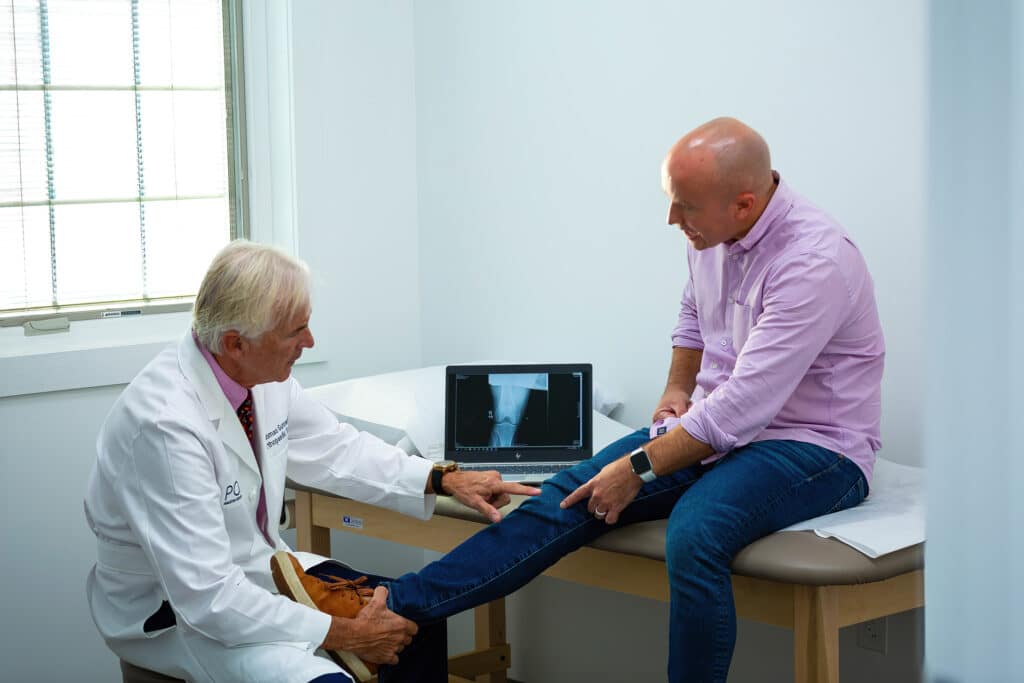

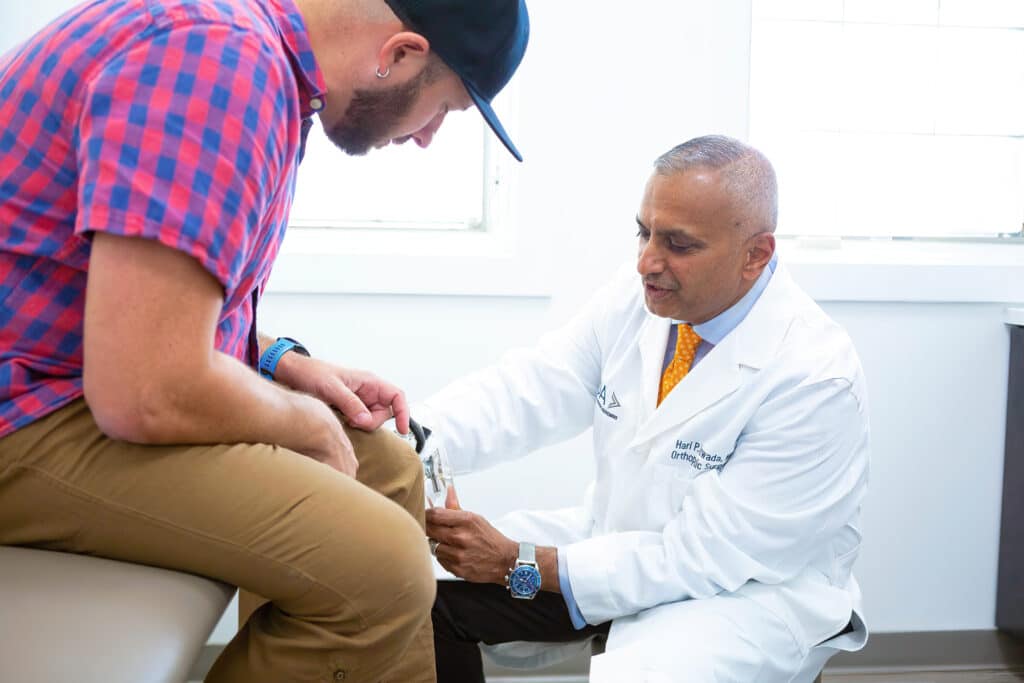
Labs are beneficial for diagnosing OA since they may be used to rule out various types of inflammatory arthritis with similar symptoms, such as rheumatoid arthritis. In other words, if you have joint ailment and your lab tests are normal, you have OA.
These exams may include:
If your blood tests come back normal or negative, this is generally because you have osteoarthritis. It should be noted, nevertheless, that as people grow older, they occasionally acquire a low-level positive rheumatoid factor titer and/or increased sedimentation rate without displaying any obvious symptoms. This is why doctors do not use laboratory tests alone to establish a possible diagnosis of osteoarthritis.
The extraction and analysis of synovial fluid from the joint is another laboratory test that might assist with confirmation. Synovial fluid is a liquid present in all joints. It helps to nourish and moisturize joints while also providing them with essential lubrication. When certain types of arthritis are present, synovium fluid will, however, alter.
White blood cell count is usually normal in osteoarthritis, and the fluid is clear (similar to water). Rather than osteoarthritis, higher white cell counts should point to an inflammatory condition or infection. Extracting synovial fluid this way may assistance in confirming the diagnosis. It might help to relieve pain and inflammation if the fluid is causing irritation. Furthermore, the fluid might be tested to detect uric acid crystals (which is present in gout) or calcium pyrophosphate crystals (seen in pseudogout or chondrocalcinosis). The measurement of additional biological indicators is still under study.
Your doctor will create an individualized treatment plan based on your unique circumstances, such as:
Early-stage osteoarthritis, when possible, may be treated nonoperatively using physical and occupational therapy. NSAIDs (nonsteroidal anti-inflammatory medicines) can assist in many cases, while corticosteroid injections can delay the need for surgery. P
Osteoarthritis can be treated effectively with non-steroidal anti-inflammatory medications (NSAIDs), such as ibuprofen (Advil), naproxen (Aleve) and celecoxib (Celebrex). Duloxetine is a medication used to treat anxiety and depression, but it has been observed to relieve pain in some cases — like with osteoarthritis. It's usually used as a second line treatment for people who have tried but failed to get relief from NSAIDs.
For people with osteoarthritis, it is critical to remain active and avoid becoming sedentary. Movement might help to reduce discomfort and prevent it from getting worse. However, the best and safest forms of activity differ from patient to patient. Getting an appropriate “movement prescription” necessitates obtaining a correct, precise diagnosis and making sure that all members of the healthcare team (orthopedists, physical therapists, etc.) are aware of each patient's specific condition.
To help with the symptoms of early-stage knee arthritis, it's critical to strengthen thigh muscles to assist the joint. It is also beneficial to have a balanced diet and maintain a healthy weight. These techniques will help to decrease knee discomfort and boost function by decreasing the amount of pressure on the knee joints.
When the conservative measures above are insufficient, and pain in a specific joint makes it difficult for you to move, joint replacement surgery may help you regain your comfort and resume normal activities. Hip replacement and knee replacement have become standard therapies for regaining mobility and alleviating pain after suffering from hip or knee arthritis.
Some people with hip or knee arthritis may be able to have more minimally invasive hip arthroscopy or knee arthroscopy operations. For those who have arthritis in their shoulder, elbow, wrist, or ankle joints, joint replacement surgery might be an option.
If non-operative therapy hasn't worked, you're generally a good candidate for surgery if you experience a substantial interruption in some activity of daily life – for example, if you can't walk more than a city block or if you awake from sleep with discomfort in the hurting joint. If you have arthritis, you are at a higher risk of developing osteoarthritis. Surgery will provide excellent outcomes if your pain goes away in the afflicted joint. The sort of operation you receive will be determined by your age, level of activity, and the afflicted joint.
Please note, Princeton Orthoapaedic Associates may not offer the service you see here. This information is provided as-is and for your information purposes only. This is not medical advice. If you are curious about an orthopaedic consult, please contact us.
© 2025 Princeton Orthopaedic Associates. The contents of PrincetonOrthopaedic.com are licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. Copying without permission is strictly forbidden. Privacy Policy | Accessibility