
Book An Appointment
Physician Assistants
Physical & Occupational Therapists
KneeMRI ScansNon-OperativePhysiatry
Physical Therapy
Podiatry
Spine
Sports Medicine
TraumaUrgent Care
X-Ray Imaging

We get it. We like our acronyms! Orthopaedic Surgeons, and doctors in general, often go around saying groups of letters as if everyone is going to get it.
That’s why we’ve created a comprehensive list to serve as a clear and reliable reference for our patients. Whether you’re reviewing test results, discussing a diagnosis with your physician, or reading about your recovery plan, this list can help you make sense of the medical language being used. Our goal is to empower patients with knowledge so that every conversation about your health is less intimidating and more productive.

| Acronym | Full Title | Description |
|---|---|---|
| MD | Doctor of Medicine | Completed allopathic medical training. Focuses on traditional biomedical model and is licensed for full scope medical and surgical practice. |
| DO | Doctor of Osteopathic Medicine | Completes the same training as MDs with added emphasis on holistic care and musculoskeletal system. Licensed for full medical and surgical practice in the U.S. |
| PA-C | Physician Assistant, Certified | Graduate-level provider trained in diagnosis, treatment, and minor surgery. Works under physician supervision but can prescribe and manage care. |
| NP | Nurse Practitioner | Advanced practice registered nurse with graduate-level training. Provides diagnosis, treatment, and prescribing, often with a holistic emphasis. |
| DNP | Doctor of Nursing Practice | Highest clinical nursing degree with focus on evidence-based practice and leadership. Functions as an NP but with expanded academic and clinical training. |
| CRNA | Certified Registered Nurse Anesthetist | Advanced practice nurse specializing in anesthesia. Provides anesthesia independently or alongside anesthesiologists in surgery and trauma settings. |

Learn why knees sometimes pop, when it’s usually harmless, and when it may signal a problem. Common causes include gas bubbles or tendons snapping, but popping can also point to joint issues. Explore simple at-home steps that may help, and know when it’s time to see a clinician.
If you hear occasional popping without pain, it is usually not serious. But if popping comes with pain, swelling, instability, or locking, you should seek evaluation so we can find the cause and plan treatment.
Sometimes popping is simply noise from normal joint movement. A few common benign reasons include:
Painless popping alone is not known to cause arthritis; however, if popping is accompanied by pain, swelling, instability, or limits on function, you should have it evaluated.
Popping that comes with other symptoms may point to an underlying injury. Watch for these signs:
Those symptoms suggest we should examine the joint to look for cartilage injuries, meniscal tears, ligament strain, loose fragments, or significant joint inflammation.
If any of the following occur after a pop, get urgent or emergency care rather than waiting for a routine appointment:
Several common issues can cause painful popping. These include damage to soft tissues, cartilage problems, and mechanical irritation around the joint.
Your clinician will take a careful history and perform a focused exam to check motion, stability, and areas of tenderness. That helps narrow down likely causes.
Imaging and tests are selected based on the history and exam. X-rays are often first-line after trauma to assess for fracture and alignment; X-rays do not show soft tissues. MRI is ordered when the exam or history suggest soft tissue injury such as meniscus or ligament tears, cartilage damage, or when mechanical symptoms persist. Ultrasound can be useful for dynamic snapping and for evaluating superficial tendon or bursal problems.
| Test | What it shows |
|---|---|
| X-ray | Bone alignment, fracture, and evidence of arthritis; does not show soft tissues |
| MRI | Soft tissues like meniscus, ligaments, and cartilage; used when exam or history suggest soft tissue injury or persistent mechanical symptoms |
| Ultrasound | Tendon or bursa irritation near the knee and useful for dynamic snapping |
If popping is mild and not accompanied by the concerning signs above, try conservative care while watching symptoms. Small changes often help.
Contact us for an evaluation if you have persistent pain, swelling, catching or locking, repeated giving way, or if symptoms prevent daily tasks. Early assessment helps us treat the cause and reduce the chance of longer term issues.
| Specialty | Why you would see them |
|---|---|
| Sports Medicine | Non surgical evaluation for tendon, ligament, and meniscal problems |
| Orthopaedic Surgeon | Persistent mechanical symptoms or when surgery may be needed |
| Physical Therapist | Rehabilitation to improve strength, control, and movement patterns |
Treatment depends on the diagnosis. Many causes improve with a planned rehab program that reduces pain, restores motion, and strengthens supporting muscles. When structural damage is severe, surgical options may be discussed.
If you want to discuss symptoms, we make it easy to schedule an exam. A focused visit helps us determine what is normal and what needs treatment so you can get back to your routine with confidence.

Please contact us! We'd love to help.
If you have pain, please contact us and schedule an appointment. We have urgent care facilities all over New Jersey for your convenience.
This blog post is meant to be informative and should not act as a self-diagnosis tool. If you’d like to see one of our doctors, please contact us here.
Whether you’re just trying to stay active, chasing after your kids, or if it's your teen pushing through practices and games, shin splints can stop you in your tracks. That aching, sometimes sharp pain along the front of the leg isn’t only for athletes running marathons, it’s surprisingly common in everyday life. Kids in fall sports like soccer, football, and cross-country often run into it, but parents and adults who spend long hours on their feet or squeeze in workouts can feel it too. What starts as a dull soreness after activity can quickly turn into a daily frustration, making simple things like walking, climbing stairs, or enjoying playtime harder than they should be. Shin splints don’t just interrupt sports; they interrupt life. This post explains what causes shin splints, how they feel, how we diagnose them, and practical steps you can take to feel better. We cover common triggers, home care, when to see a specialist, and what recovery usually looks like.

You’ll learn why shin splints happen, what symptoms to watch for, which everyday habits make them worse, and how we at Princeton Orthopaedic Associates approach treatment and recovery.
Shin splints is a common name for pain along the shin bone that starts with activity. Classic shin splints most commonly refer to medial tibial stress syndrome, or MTSS, which presents as a diffuse aching along the posteromedial, or inner, border of the lower tibia near the distal half of the shin. Persistent pain over the front of the shin is less typical for MTSS and may indicate a tibial stress fracture or exertional compartment syndrome, so those symptoms should be evaluated.
MTSS is not just simple surface inflammation. It sits on a bone stress continuum where repeated overload affects the tibial cortex and the periosteum, and traction from muscles such as the soleus and tibialis posterior contributes to symptoms. We keep explanations simple but want you to know the pain often reflects mechanical overload of bone and the tissues attached to it.
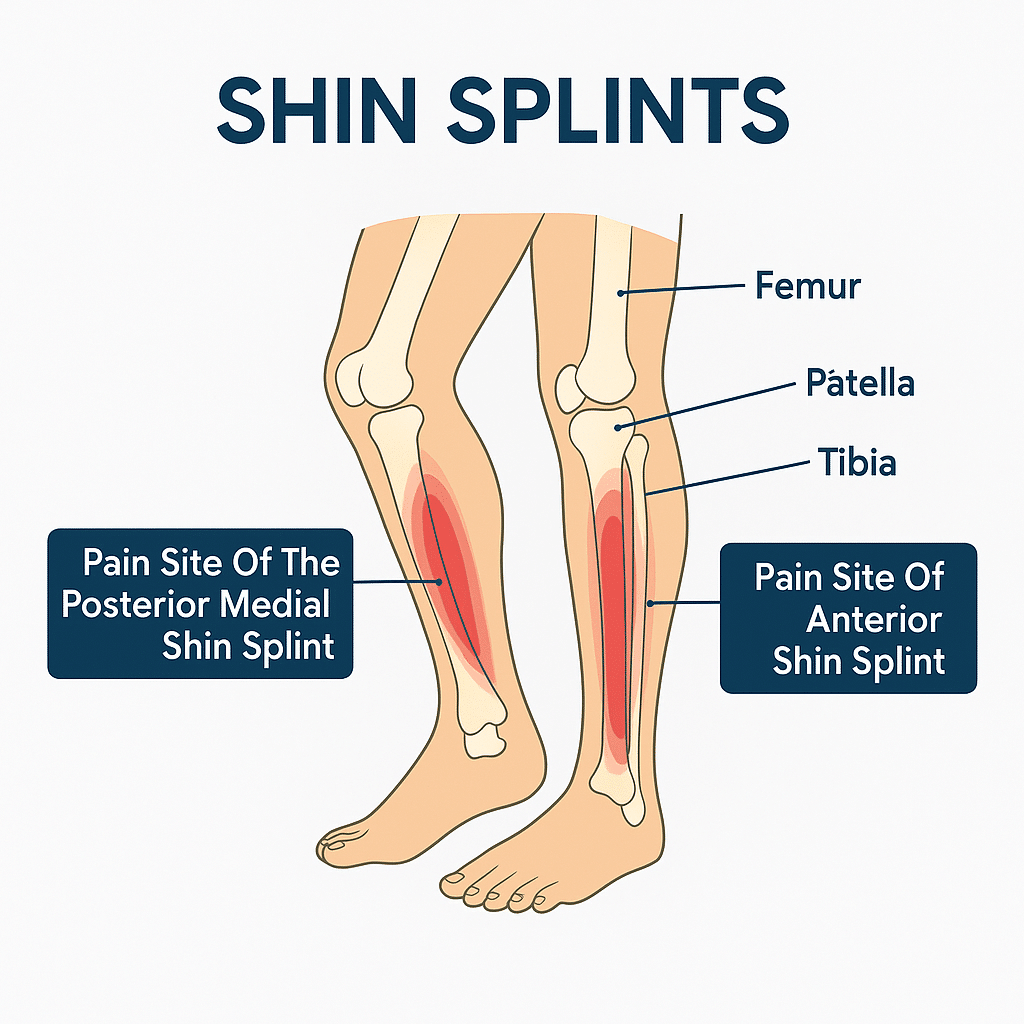
Symptoms of shin splints usually start as a dull, aching pain along the inner edge of the lower leg, often felt during activity and easing with rest early on. The pain typically covers a broader segment along the posteromedial tibia rather than a single sharp spot.
By contrast, a tibial stress fracture more often causes focal point tenderness, a small spot that is exquisitely painful to press. Exertional compartment syndrome may produce tightness, cramping, numbness, or weakness during activity. If your pain is sharp, highly localized, wakes you at night, or makes it hard to walk, see a clinician promptly to check for these possibilities.
Shin splints come from repetitive stress on the lower leg. You don’t have to be a runner to get them; they happen with many forms of exercise and work that increase load on the shin.
Diagnosis starts with a careful history and a physical exam. We check the pattern of pain, how it changes with activity, and look at your foot and ankle mechanics. The exam helps distinguish shin splints from a focal stress fracture or from exertional compartment syndrome.
If needed, imaging can help rule out a stress fracture or other conditions when symptoms are severe, very focal, or not improving with appropriate rest. X-rays are often the first test but can be normal early on. If concern persists, an MRI is more sensitive and can confirm a bone stress injury.

Gently stretching tight calves and working on ankle mobility can help. Do not push through sharp pain during exercises. If symptoms suggest a stress fracture or compartment syndrome, stop the aggravating activity and seek evaluation.
If symptoms persist, physical therapy is often the next step. A therapist will guide you through strengthening and flexibility work to correct the forces that stress the shin and help you return to activity safely.
Recovery time varies based on severity and how quickly you address the cause. The table below gives a general idea.
| Severity | Typical Recovery | Notes |
|---|---|---|
| Mild | 2 to 4 weeks | Relative rest, icing, and gradual return usually helps. |
| Moderate | 4 to 8 weeks | Often needs formal rehab and footwear changes. |
| Severe or Persistent | 8 weeks or more | May require imaging and a structured rehab plan to avoid stress fracture risk. |
Seek care if pain is severe, gets worse despite rest, or you cannot put weight on the leg. Also see a clinician if pain wakes you at night, if you have marked swelling, or if you have new numbness or weakness.
Be alert for signs that need prompt or urgent evaluation, including:
| Specialty | Why You'd See Them | Notes |
|---|---|---|
| Sports Medicine | Non-surgical diagnosis and treatment of overuse injuries | Good first stop for activity-related shin pain |
| Physical Therapy | Guided rehabilitation and return-to-activity plans | Focuses on strength, flexibility, and movement patterns |
| Foot and Ankle Specialist | When foot mechanics, orthotics, or surgical options are considered | Helpful if foot structure contributes to repeat problems |
Return to activity should be gradual and guided by pain. Increase load slowly and stop if symptoms flare. A simple progression to consider is pain-free walking, then a pain-free single-leg hop, then light jogging. If those steps are comfortable, gradually increase duration and intensity while continuing strengthening and mobility work.
If you are unsure whether your pain is caused by shin splints or something more serious, schedule an exam so we can check you and recommend the right next steps.

Please contact us! We'd love to help.
If you have pain, please contact us and schedule an appointment. We have urgent care facilities all over New Jersey for your convenience.
This blog post is meant to be informative and should not act as a self-diagnosis tool. If you’d like to see one of our doctors, please contact us here.
You don’t have to be a marathon runner to feel that nagging ache on the outside of your knee. The important thing? It might not actually be your knee. It might be a tight IT band, and unlike joint injuries, it requires a different kind of treatment focused on mobility and muscle balance.
Maybe it starts during your daily walk, or when you’re going up stairs. Perhaps it flares up when you get up from your desk or out of the car. It might even wake you up at night, pulsing in your outer thigh or hip, making it impossible to get comfortable. It doesn’t feel like an injury yet, the pain keeps coming back.
If this sounds familiar, there’s a good chance your iliotibial band (IT band) is involved. And the condition you might be dealing with is called IT Band Syndrome, a common cause of outer knee and hip pain that affects far more than just athletes.
Let’s walk through what’s happening in your body, why it hurts, and most importantly, what you can do to start feeling better.
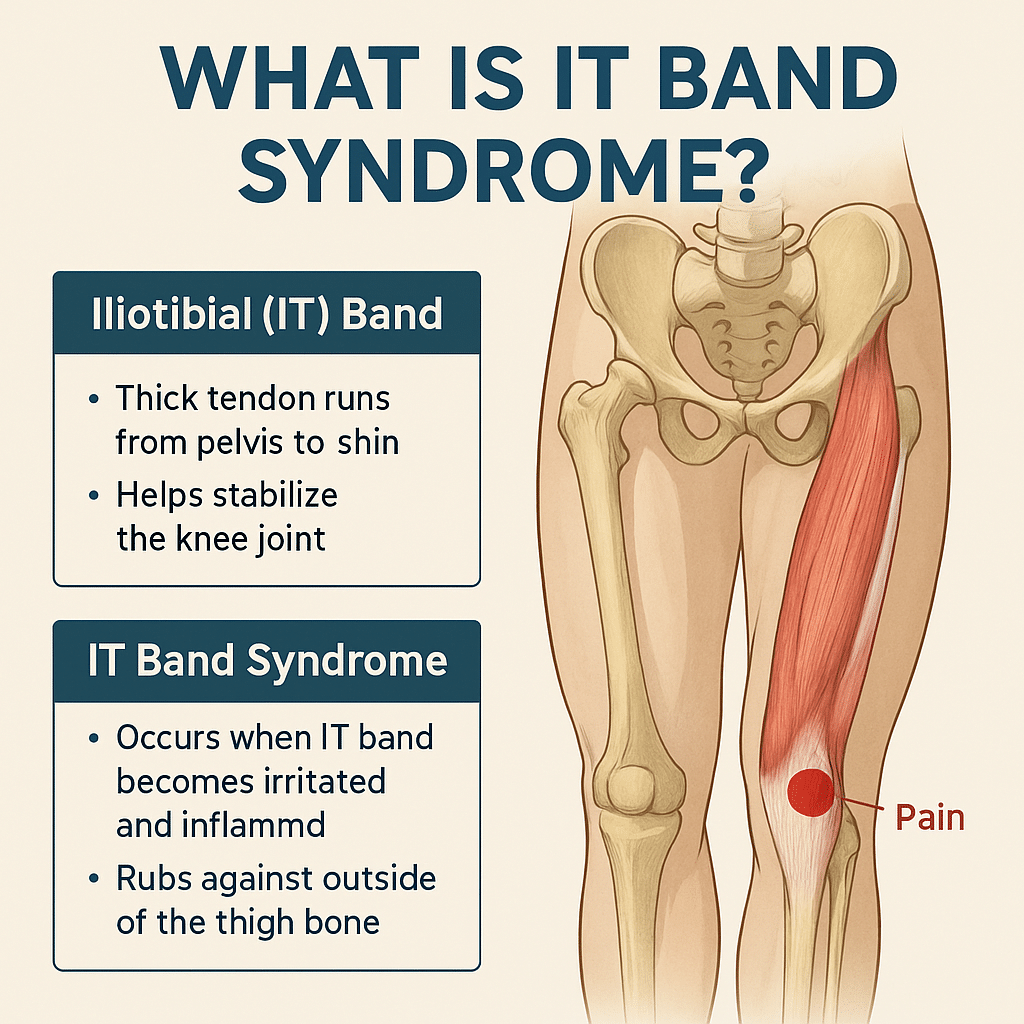
The iliotibial (IT) band is a thick, fibrous band of connective tissue that runs down the outside of your leg, from your hip to just below your knee. Think of it as a support strap that helps stabilize your knee and assist with hip movement.
When the IT band gets too tight, often due to repetitive movement, muscle imbalances, or poor posture, it can rub against the bone at the outer knee. This creates irritation, inflammation, and pain, commonly known as IT Band Syndrome (ITBS).
And while it’s often associated with athletes, it’s just as common in walkers, desk workers, parents, nurses, retail workers, and anyone who’s on their feet a lot, or not enough.
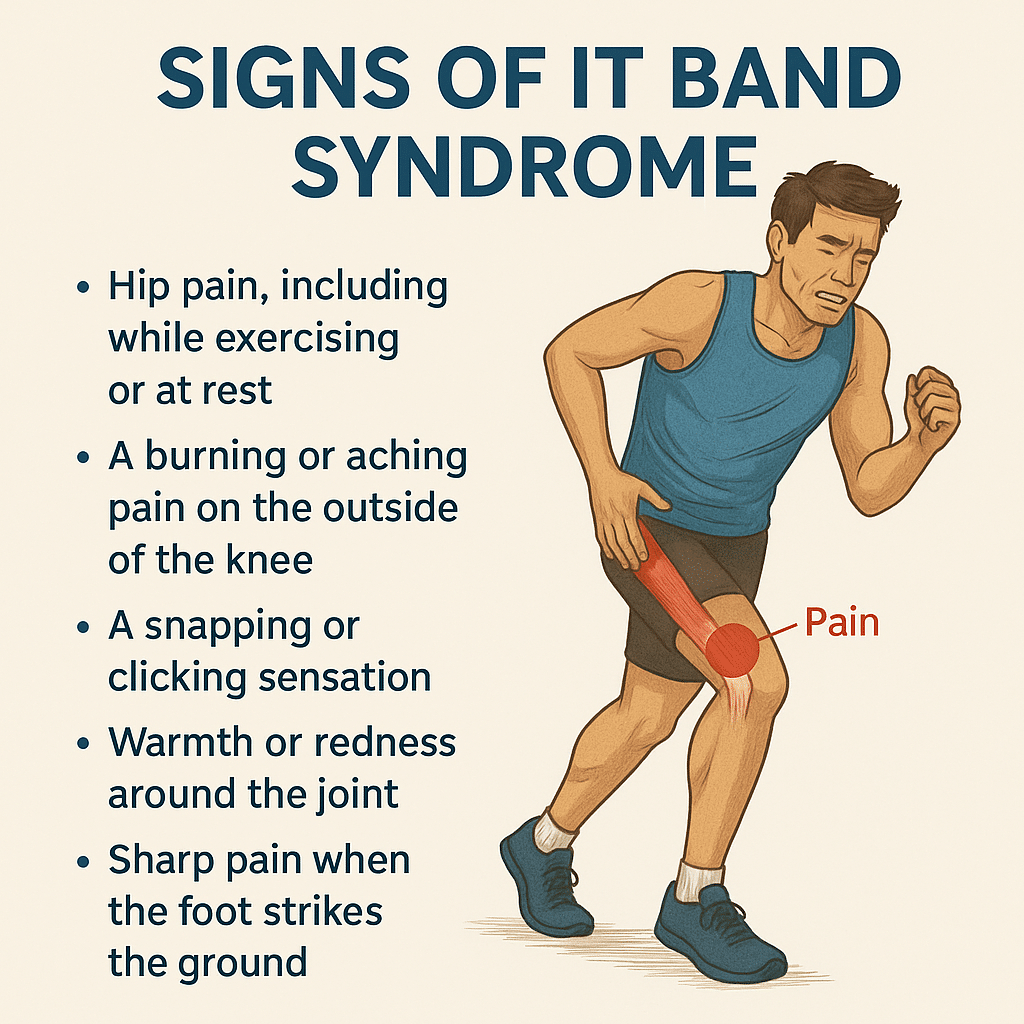
Here are common, real-world symptoms of IT Band Syndrome in everyday life:
These symptoms often start mild, but become more consistent if left unaddressed.
Even without intense training, everyday habits can contribute to ITBS:
While the core problem is the same (tightness and friction along the IT band), athletes often develop ITBS due to training volume and biomechanics. Common athletic triggers include:
IT Band Syndrome is common among:
💡 Tip for athletes:
Strengthen your hips and glutes, cross-train, and make sure your recovery matches your training load
.
The IT band isn’t a muscle, it’s actually connective tissue. That means:
Over time, the friction and inflammation can become chronic and much harder to treat.
Treatment focuses on reducing inflammation, improving mobility, and correcting muscle imbalances.
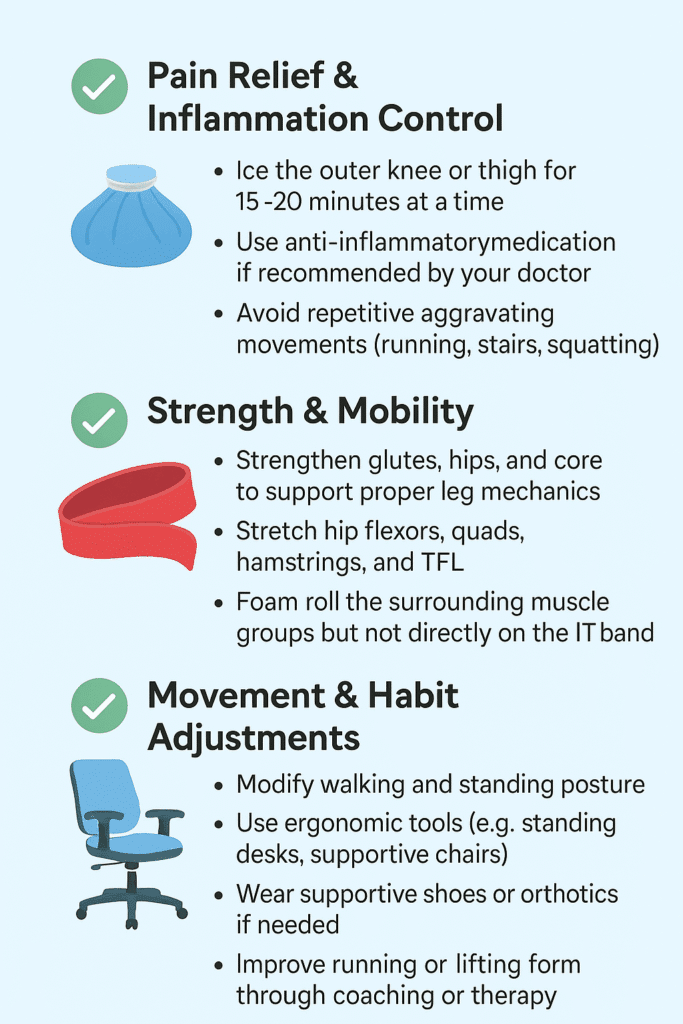
✅ Pain Relief & Inflammation Control
The length of time to recover from IT Band Syndrome depends on how long you've had symptoms and whether you're treating the root cause:
2-3 Weeks
Rest and stretching may help quickly if caught early
4-6 Weeks
Requires active rehab including movement correction
2+ Months
Long-standing tightness or inflammation takes time to unwind
IT Band Syndrome doesn't just show up during workouts; it can quietly interfere with our daily routine, mobility, and overall comfort. Without treatment, ITBS can impact your:
And for athletes, it can put your training on pause or create a cycle of recurring injuries.
If you have been experiencing symptoms of IT Band Syndrome and you haven't found relief, you should consult with a specialist. Especially if:
At Princeton Orthopaedic Associates, we have physicians from multiple specialties that can help you get to the root of your tight IT band and help set you off on the path to recovery.
-Trained to treat soft tissue overuse injuries like ITBS
- Can differentiate between joint issues and soft tissue problems
- Often the best first stop for a non-surgical, comprehensive evaluation
- Focuses on functional movement and musculoskeletal pain
- Great at managing chronic pain or postural imbalances
-Ideal for cases involving compensations, gait issues, or mobility problems
- Best if ITBS has persisted or if you need advanced imaging or diagnostics
- Also helpful if you suspect other structural issues like meniscus, arthritis, or leg length discrepancy
- A physical therapist is often the next step after diagnosis for hands-on treatment and long-term recovery.
Our specialists will identify the root cause of your tightness, guide you through targeted corrective exercises, and help you improve how you move—not just mask the symptoms.
Whether you're training for a race or just trying to get through the workday without pain, IT Band Syndrome can be disruptive, but it's absolutely treatable. The key isn’t just stretching or resting, it's understanding why the IT band is tight and retraining your body to move in a healthier, more balanced way.

Please contact us! We'd love to help.
If you have pain, please contact us and schedule an appointment. We have urgent care facilities all over New Jersey for your convenience.
This blog post is meant to be informative and should not act as a self-diagnosis tool. If you’d like to see one of our doctors, please contact us here.
You were mid-pivot, chasing a ball or turning to grab something behind you, when a sharp pop hit your knee. Not loud, but distinct. You paused, unsure if it was serious. Maybe just a tweak, you thought. But within hours, the swelling crept in, the joint stiffened, and walking suddenly felt unfamiliar. That small twist? It turned into something much bigger.
That moment likely marked the beginning of a meniscus tear—a common yet disruptive injury affecting the cartilage in your knee. Whether it's from a sudden injury or years of wear and tear, the result is often the same: pain, limited movement, and questions about what comes next.
Inside each of your knees are two rubbery, wedge-shaped pieces of cartilage: the medial and lateral menisci. These act like shock absorbers between your thighbone and shinbone, helping to distribute weight and stabilize movement. A tear occurs when this cartilage is damaged—usually from twisting motions or degeneration over time.
You don't have to be an athlete for this to happen. A quick squat, an awkward turn, even standing up too fast with pressure on the joint can be enough, especially if the cartilage is already weakened with age.
There are two primary culprits behind a torn meniscus:
Both scenarios are incredibly common. Lifting a heavy box incorrectly or kneeling on a hard surface for too long can be all it takes.
The first few hours after the tear are often the most telling. At first, discomfort may be the only symptom of a meniscus tear you might feel. Or, the only symptoms of a meniscus tear present at first are just a dull, persistent ache, made worse by movement. You might feel fine while sitting, but as soon as you try to walk or bend, your knee doesn't cooperate. Some describe it as a "stuck" sensation, where the joint feels like it won't fully extend or flex without pain or resistance. But then the pain deepens, swelling begins, and your range of motion shrinks even more.
Clicking, popping, or catching during movement can also indicate a torn flap of cartilage catching in the joint. Check out this post to read more about the Types of Meniscus Tears.
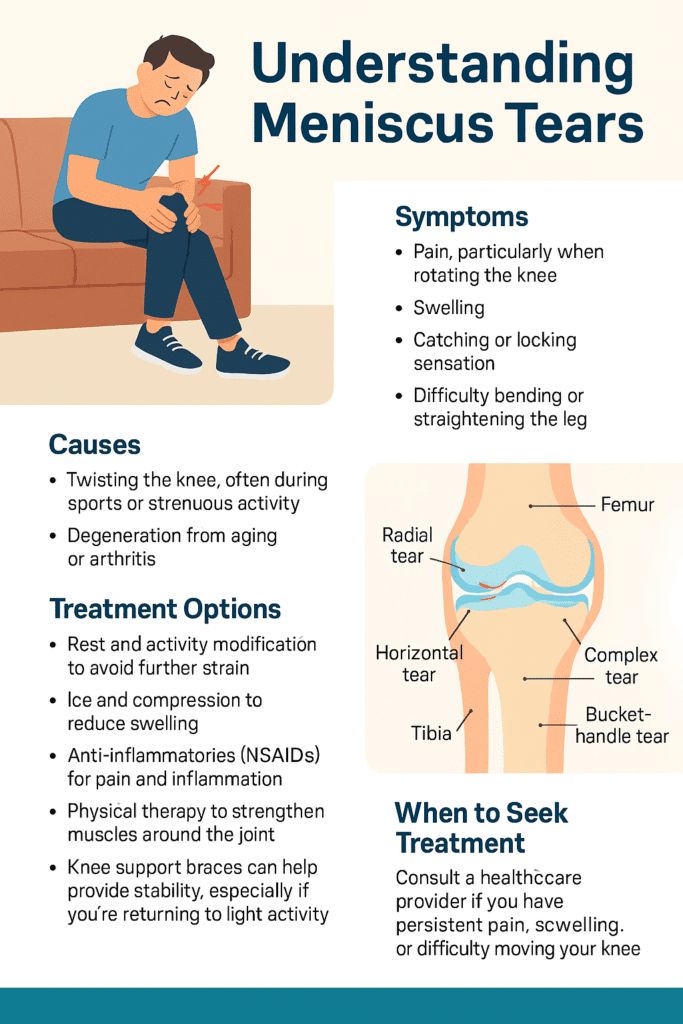
If you're looking for clarification on the symptoms of a meniscus tear, you are not alone. Many people deal with a torn meniscus and don't realize the seriousness until the stiffness and pain don't go away.
If you're hoping it will just go away, consider this: untreated meniscus tears can worsen over time, leading to more pain and even long-term joint issues like osteoarthritis.
Seek professional help if:
Ignoring it risks further tearing or cartilage breakdown. Early diagnosis often means better, less invasive treatment options.
A physical exam can often provide early clues. A clinician will test your range of motion and apply gentle pressure or rotation to identify pain points. In many cases, imaging, like an MRI, is used to confirm the diagnosis and pinpoint the severity and location of the tear.
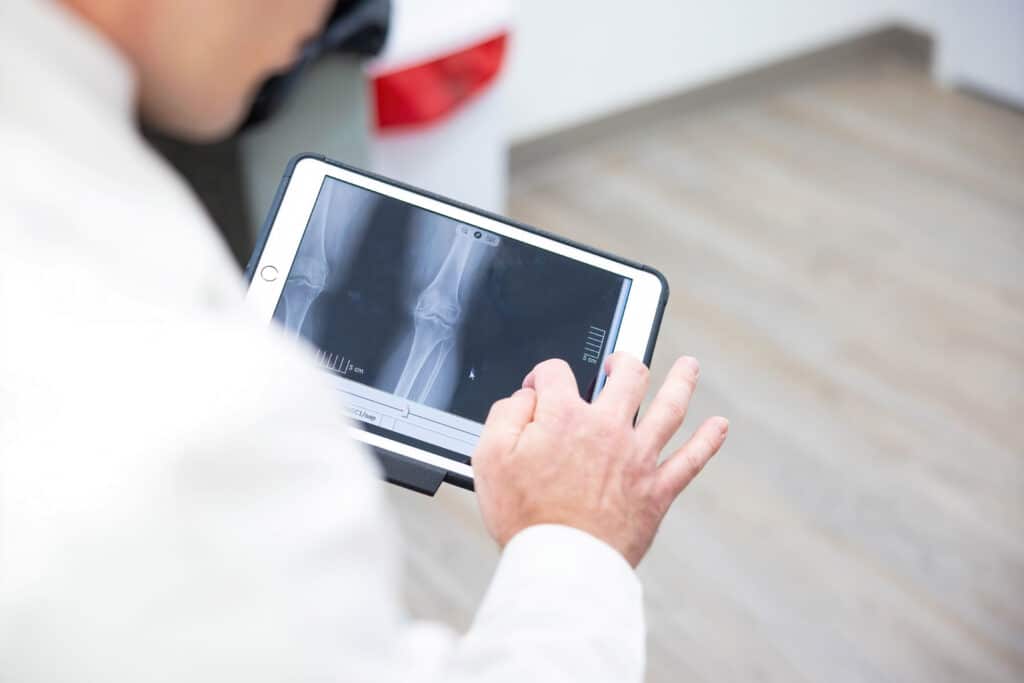
Not all meniscus tears require surgery. If you're looking for a meniscus tear remedy, treatment depends on the type of tear, location, and severity of the tear, as well as your activity level and age.
Small tears near the outer edge, where the blood supply is richer, often heal with conservative care.
If the tear is large, causes locking, or doesn't improve, arthroscopic surgery may be recommended. Options include:
Surgery is more likely in younger, active individuals or when the tear is in a critical area.
How long it takes a torn meniscus to heal depends entirely on the treatment path and your consistency with rehab. Below is a general idea of recovery times based on the type of treatment - this is for reference only and not a diagnosis and treatment.
Conservative (rest, PT)
4-8 weeks
Partial Meniscectomy
4-6 weeks
Arthroscopic Repair
3-6 months
So, how long does it take for a meniscus tear to heal? It may take time to regain strength and trust in your knee even after healing.
Yes—but that doesn't mean you should. Many people are able to walk with a torn meniscus, especially if the pain is mild. But without proper treatment, walking on a torn meniscus can cause further damage or transform a minor tear into a more serious one.
If you must stay mobile, supportive bracing and avoiding twisting motions is essential.
Despite the pain and swelling, a torn meniscus often doesn't present visible signs like bruising or discoloration. That's why if you're looking for answers to "what does a torn meniscus look like on the outside," the truth is, it doesn't look like much so you won't find much. The damage is internal; symptoms often show through movement limitations and experienced pain, not appearance.
Prevention of a meniscus tear isn't just about avoiding sports injuries—it's about daily movement, posture, and support.
While it's no guarantee you'll avoid having a torn meniscus, there are some smart prevention strategies! Some strategies include:
You don't need to be an athlete to tear your meniscus—and you don't need to live with the pain either. Even activities like walking the dog or playing with your kids carry risk if you're not mindful of sudden directional changes! With awareness, early action, and proper care, recovery is possible and often complete. Pain-free movement starts with taking your symptoms seriously, getting the right diagnosis, and committing to healing fully.
If it feels wrong, it probably is. Trust your body, and give it what it needs to bounce back. Contact us today to schedule with one of our specialists.
This blog post is meant to be informative and should not act as a self-diagnosis tool. If you’d like to see one of our doctors, please contact us here.
You’re bending over to tie your shoe, or maybe you just lifted a laundry basket off the floor—and suddenly, something shifts. A sharp, electric jolt shoots through your lower back and radiates down your leg. Within days, sitting becomes excruciating. You feel tingling in your foot. Or worse—your leg feels weak, like it might buckle underneath you.
It's not just a sore back. You could be dealing with a herniated disc—a spine condition that can disrupt your daily life, mobility, and comfort. But the good news? It’s treatable, and in many cases, you can fully recover without surgery.
Your spine is made up of 33 vertebrae, and between most of them are intervertebral discs—soft, cushion-like pads that absorb shock and allow flexibility in your back.
Each disc has two parts:
A herniated disc, also known as a ruptured disc or colloquially as a “slipped disc”, occurs when the inner core pushes out through a crack or tear in the outer shell. This herniation can press against nearby nerves, triggering pain, numbness, tingling, or weakness—depending on the location and severity of the compression.
Slipped disc vs. herniated disc: While the term "slipped disc" is commonly used, nothing actually “slips” out of place. The disc material bulges or leaks, which is more accurately described as a herniation.
| Herniated Disc | Bulging Disc | |
|---|---|---|
| What it is | The disc's inner gel-like material breaks through a tear in the tough outer layer. The outer wall is torn or ruptured. | The disc extends outward beyond its normal boundary, usually evenly around the disc's circumference. The outer wall remains intact but stretched out. |
| Severity | Typically, more severe than a bulging disc. Especially if it compresses nearby nerves. | Often considered less severe than a herniated disc and can often be asymptomatic. |
| Symptoms | Sharp pain, sciatica, numbness, tingling, or weakness in the limbs. | Mild back pain or none at all. Sometimes asymptomatic. |
| Causes | Trauma, heavy lifting, or progression of a bulging disc. | Degeneration from aging, posture, and repetitive stress. |
| Treatment | May need physical therapy, injections, or even surgery if conservative care fails. | Often responds to conservative care and lifestyle changes. |
Symptoms of a herniated disc depend on the location of the herniation and which nerves are affected. In general, the most common areas are the lumbar (lower back) and cervical (neck) spine.
In many cases, herniated discs heal without surgical intervention. Your body has the ability to reabsorb the protruding disc material and reduce inflammation around the affected nerve.
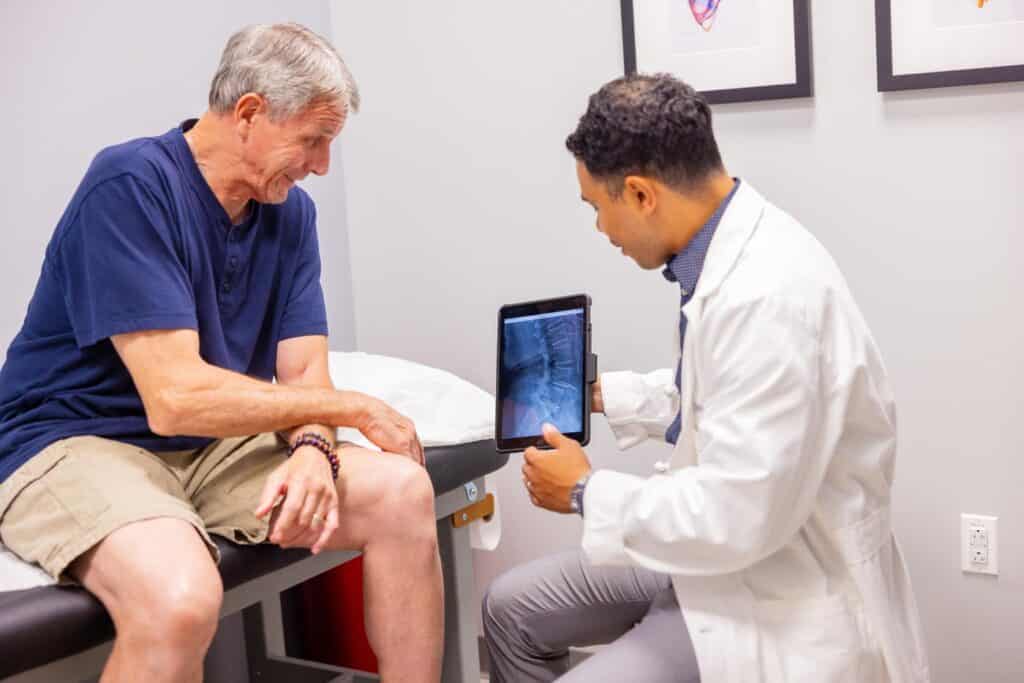
The recovery timeline depends on the severity of the herniation and the treatment used. It can take time and varies depending on your health, age, and activity level:
| Severity | Differentiator | Recovery Timeframe |
|---|---|---|
| Mild-Moderate | Responds to rest, physical therapy, and medication. | 4-6 weeks |
| Persistent | Involves nerve compression or recurrent flare-ups. | 8-12+ weeks |
| Chronic or Severe | Presents with significant neurological symptoms. | Extensive treatment or surgical intervention |
The most common causes of a herniated disc can include:
If you experience sudden back or neck pain along with radiating symptoms, take the following steps:
Stop any strenuous activity: Avoid lifting, twisting, or bending.
Apply cold packs (for the first 48 hours): Reduces inflammation and pain.
Switch to heat after 2–3 days: Relaxes tight muscles and improves circulation.
Over-the-counter medications: NSAIDs (like ibuprofen) help reduce swelling and pain.
Stay mobile—lightly: Short walks are better than prolonged bed rest, which can weaken muscles and delay healing.
Track your symptoms: Take note of any numbness, tingling, or weakness.
If you suspect you have a herniated disc, don’t wait. If you have any of the following symptoms you should seek care as soon as possible:
For the best outcomes, consult with an orthopaedic specialist. At POA, these may include:
Every person is unique so every treatment approach and plan is tailored for your specific needs.
A typical diagnosis can include a review of your medical history such as prior injuries, sumptom patterns, lifestyle, and your work habits. It also involves a physical exam which may include reflex testing, muscle strength, raings of motion, and nerve response.
Imaging may also be ordered to assist in a comprehensive evaulation.
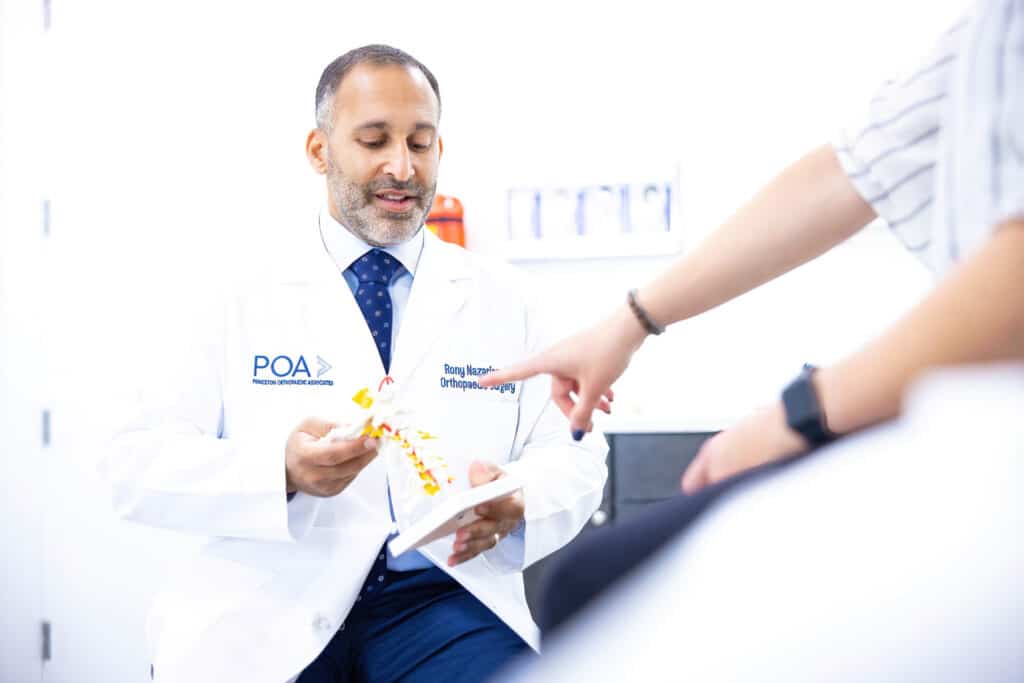

At POA, we specialize in restoring comfort, strength, and movement—without rushing to surgery.
✅ Board-certified spine specialists with years of experience in both conservative and advanced surgical care.
✅ Personalized treatment plans: Tailored to your body, lifestyle, and goals.
✅ Commitment to conservative care first: We explore every non-surgical option before recommending surgery.
✅ Multidisciplinary approach: Orthopaedic surgeons, physical therapists, and pain specialists collaborate on your care.
✅ Advanced diagnostics: Immediate access to imaging and nerve studies for fast, accurate diagnosis
Whether you’re newly injured or have struggled with back pain for months, POA’s spine experts can help you get your life back on track.
A herniated disc can feel like a life-altering injury, but it doesn’t have to be. With the right care team and a focused treatment plan, recovery is not only possible—it’s probable. Don’t wait in pain! Schedule with one of our Orthopaedic Spine Specialists today and take your first step toward relief and recovery.

Please contact us! We'd love to help.
If you have pain, please contact us and schedule an appointment. We have urgent care facilities all over New Jersey for your convenience.
This blog post is meant to be informative and should not act as a self-diagnosis tool. If you’d like to see one of our doctors, please contact us here.
You know the pain well. As you rise from bed every morning, you place your feet on the floor, only to be greeted with a sharp, stabbing sensation in your heel. It's like a jolt that reminds you that the pain isn't gone yet. After walking around for a few minutes, the discomfort may ease. Still, it always comes back when you've been on your feet too long, especially after resting or sleeping. This is a daily struggle for those living with plantar fasciitis – a condition that affects your ability to walk comfortably and can take a toll on your overall quality of life.
Plantar fasciitis occurs when a thick connective tissue running from your heel to your toes along the bottom of your foot (plantar fascia) becomes irritated and inflamed. The plantar fascia supports the foot's arch and is essential for proper foot movement and support while walking. Excessive strain or overstretching can cause tiny tears in the fascia, triggering inflammation and discomfort, particularly in the heel.
While plantar fasciitis is frequently seen in physically active individuals, it can affect anyone. Symptoms tend to worsen in the morning when the tissue tightens during sleep, causing significant discomfort with the day's first steps.
If you’ve ever felt a sharp, stabbing pain in your heel when you step out of bed in the morning, you may be dealing with plantar fasciitis—one of the most common causes of heel pain. This condition affects millions of people each year, but it’s not random. Certain groups are more likely to develop it based on lifestyle, footwear choices, and physical activity.
People who run regularly or participate in high-impact sports are among the most common groups to experience plantar fasciitis symptoms. Repetitive motion, especially without proper stretching or supportive footwear, can cause microtears in the plantar fascia. Increasing mileage too quickly, running on hard surfaces, or using worn-out shoes can all contribute to heel pain in runners.
Working a job that keeps you on your feet for hours at a time can put you more at risk for developing plantar fasciitis. Teachers, nurses, warehouse workers, and retail staff often experience chronic foot and heel pain due to the constant pressure on their feet—especially if they’re standing on hard surfaces like concrete or not wearing cushioned shoes.
Carrying extra weight puts more pressure on your feet and heels, making it harder for your plantar fascia to do its job. This is especially true during long periods of walking or standing. Losing even a modest amount of weight can often reduce pain and prevent further damage.
Your natural foot shape or the way you walk could be behind your chronic heel pain. People with flat feet, high arches, or those who overpronate (roll their feet inward too much) often experience more strain on the plantar fascia, leading to irritation and inflammation. Tight calf muscles or a limited range of motion in your Achilles tendon can also increase your risk.
Unfortunately, age is another common factor. Middle-aged adults are more likely to develop plantar fasciitis due to natural wear and tear. The connective tissue in our bodies loses elasticity as we age, making us more prone to injury from overuse or poor support.
Let’s talk about your footwear! Flip-flops, ballet flats, high heels, and worn-out sneakers all share the same issue, they offer little to no arch support. Wearing these types of shoes regularly can increase your risk of developing plantar fasciitis, especially if you're walking long distances or spending hours on your feet.
Several contributing factors can lead to plantar fasciitis. Understanding these causes of plantar fasciitis can help prevent the condition or reduce the risk of recurrence:
Overuse and repetitive stress
Plantar fasciitis is often caused by repetitive activity that stresses the plantar fascia. High-impact activities like running or jumping can overstrain this tissue, especially if done incorrectly or without proper footwear.
Improper footwear
Shoes that lack adequate arch support, cushioning or are worn-out can exacerbate heel pressure. High heels, flip-flops, or shoes with flat soles may contribute to this strain.
Foot structure abnormalities
People with flat feet, high arches, or abnormal gait patterns may place excessive stress on the plantar fascia. The added strain causes the tissue to become overstretched, leading to inflammation and pain.
Obesity or excess weight
Extra weight puts additional pressure on the feet, making them more susceptible to injury and strain. Over time, this additional weight can cause microtears in the plantar fascia, leading to plantar fasciitis.
Tight calf muscles or Achilles
Having tightness in the calves or Achilles tendon can affect how pressure distributes across your feet. This adds stress to the plantar fascia, increasing the likelihood of inflammation and discomfort.
Aging
As you age, the plantar fascia loses some elasticity and shock-absorbing properties. This makes the tissue more prone to tears and inflammation, leading to plantar fasciitis, especially in people over 40.

Please contact us! We'd love to help.
If you have pain, please contact us and schedule an appointment. We have urgent care facilities all over New Jersey for your convenience.
You can usually manage plantar fasciitis with at-home treatments. Still, sometimes, certain situations warrant a visit to an orthopedic specialist.
Here are several strategies you can use at home to help relieve the pain and inflammation associated with plantar fasciitis:
Giving your foot time to heal is essential. Avoid activities that involve running, jumping, or standing for long periods, as these can further irritate the plantar fascia.
Applying an ice pack to your heel for 15-20 minutes several times throughout the day can help reduce inflammation and pain.
Medications like ibuprofen or naproxen can reduce inflammation and relieve pain. Be sure to follow the recommended dosage and consult a doctor if needed.
Stretching your calf muscles, Achilles tendon, and the plantar fascia can help alleviate your pain and prevent stiffness. Simple exercises like towel stretches or calf stretches can improve your flexibility and reduce the strain on your foot.
Wearing supportive shoes with proper arch support and cushioning can reduce pressure on your plantar fascia. Orthotic insoles may also help distribute pressure more evenly across your foot.
Wearing night splints can help maintain a light stretch of the plantar fascia while you sleep. This helps prevent the fascia from tightening during the night and reduces morning pain.
Preventing plantar fasciitis is possible but it involves making adjustments to your daily habits and lifestyle.

Wear proper footwear – Select footwear that provides the right arch support, cushioning, and stability for your heels. Avoid walking barefoot on hard surfaces and limit prolonged use of high heels to reduce strain on your feet.
Regular Stretching – Regularly stretch your calves, Achilles tendons, and feet to improve flexibility and reduce the risk of strain on the plantar fascia.
Maintain a healthy weight – Keeping your weight within a healthy range will help to reduce the strain on your feet, decreasing your chances of developing plantar fasciitis.
Take breaks to rest – If you stand or walk for long periods, take breaks to rest your feet and alleviate pressure. If you can't take breaks, alternating between sitting and standing can also help prevent overuse.
Strengthen your feet and lower legs – Exercises that strengthen your calf muscles, foot muscles, and ankle stabilizers can help prevent plantar fasciitis by improving foot mechanics and reducing excessive strain.
Towel Stretch – Sitting on the floor with your legs stretched out in front of you, wrap a towel around the ball of your foot. Gently pull your foot toward you, feeling a stretch along the bottom of your foot and the back of your leg.
Calf Stretch – Stand arm's length facing a wall and step back with one leg. Keep your back leg straight and your heel planted on the ground. Place your hands on the wall at the height of your shoulders and lean forward, stretching your calf and Achilles tendon of your back leg.
Foot Roll – To help massage the plantar fascia and relieve built-up tension, you can use a tennis ball or similar ball under the arch of your foot. Once you place it, slowly roll it back and forth.
Toe Stretch – While sitting with your legs extended, reach for your toes and gently pull them toward your body. This stretch helps loosen the plantar fascia and should be held for 15-30 seconds before repeating.
Heel Raises – Stand with the balls of your feet on the edge of a step. Slowly lift yourself onto your toes, then lower your heels past the level of the step to stretch your calves and the bottom of your feet.

Whether you're a runner, a retail worker, or someone who loves their flip-flops a little too much, plantar fasciitis can sneak up on you. Knowing your risk factors is half the battle. With the right footwear, regular stretching, and paying attention to heel pain symptoms, you can take steps (literally!) to protect your feet.
Plantar fasciitis doesn't have to be a permanent issue. You can effectively manage and treat this painful condition with proper care, early intervention, and lifestyle adjustments. If your at-home treatments aren't bringing you relief or if your symptoms are worsening, Princeton Orthopaedic Associates is here to help. Our team of specialists can provide targeted therapies, advanced treatments, and personalized care to help you get back on your feet and live pain-free.
This blog post is meant to be informative and should not act as a self-diagnosis tool. If you’d like to see one of our doctors, please contact us here.

You wake up with a stiff neck, thinking you just slept in an odd position. But as the day goes on, the pain doesn't go away. Instead, it radiates down your shoulder and into your arm. Simple tasks like turning your head, reaching for your phone, or even sitting at your desk become uncomfortable. You think, maybe you just slept weird and it will feel better tomorrow, except the pain doesn't improve, it continues for days, even weeks. This is what living with a pinched nerve in the neck can feel like—persistent discomfort that affects your daily life.
A pinched nerve in the neck, also known as cervical radiculopathy, occurs when excessive pressure is applied to a nerve root in the cervical spine (neck area). This pressure can come from surrounding structures such as bones, cartilage, muscles, tendons, or swollen tissues, leading to nerve irritation or compression. This compression disrupts the nerve's normal function and can lead to pain, tingling, weakness, or numbness in your neck.
The symptoms you experience from a pinched nerve in the neck can vary from person to person, but generally speaking, the most common symptoms often involve a discomfort that radiates beyond your neck. You may experience a sharp or burning pain that extends into the shoulder, arm, or even down to the fingers, sometimes worsening with certain movements or prolonged positions. With the pain, there may be an unusual tingling or buzzing sensation, almost like the affected area has "fallen asleep," which can become persistent or intermittent. You may also notice weakness in their grip or find it harder to perform tasks requiring fine motor skills, as the nerve's ability to send signals to the muscles is compromised. In more severe cases, prolonged compression can lead to a feeling of numbness or loss of sensation in certain areas, making it difficult to tell if you're touching something or feeling temperature changes properly.
The causes of a pinched nerve in the neck can vary from person to person, but generally speaking, they stem from excessive pressure or irritation affecting the nerves in your spine in the neck. In many cases, age-related changes in the spine, such as degenerating discs or bone spurs, gradually narrow the space where nerves exit, leading to compression. Injuries, like sudden whiplash from a car accident or repetitive strain from poor posture, can also cause misalignments or inflammation that presses on the nerve. For some people, long hours spent looking down at a phone or sitting at a desk with improper ergonomics contribute to chronic strain, gradually leading to nerve irritation. Inflammatory conditions, like arthritis, or acute issues, such as a herniated disc leaking fluid onto nearby nerves, can also increase pressure, intensifying symptoms over time.
Pain persists for several weeks despite home treatments.
Weakness in your arms or hands affects daily tasks.
Loss of coordination or balance signals nerve damage beyond just discomfort.
Symptoms worsen over time, even with rest and self-care.
Loss of bowel or bladder control can sometimes happen and may indicate a more serious spinal condition requiring immediate attention.

A pinched nerve can cause discomfort ranging from mild tingling to sharp, radiating pain that disrupts daily life. Whether it’s in your neck, back, or another area, this condition occurs when surrounding tissues—such as muscles, tendons, or bones—put excess pressure on a nerve. While severe cases may require medical attention, many pinched nerves can be relieved at home with simple, effective treatments.
Preventing a pinched nerve in the neck starts with maintaining good posture, keeping muscles strong and flexible, and avoiding repetitive strain. Poor posture, prolonged screen time, and sleeping in awkward positions can all contribute to nerve compression, leading to pain, stiffness, and discomfort. By making small adjustments—such as improving ergonomics, incorporating regular stretching, and strengthening the neck and shoulders—you can reduce the risk of nerve irritation and keep your neck healthy and pain-free.
When dealing with a pinched nerve, gentle movement and stretching can help alleviate pressure, improve mobility, and promote healing.
Purpose: Strengthens the deep neck flexors, improves posture, and reduces strain on the cervical spine.
How to Do It:
Tip: Avoid tilting your head up or down—think of sliding your head straight back.
Purpose: Stretches the muscles along the sides of your neck to reduce tension.
How to Do It:
Tip: Keep your shoulders down and relaxed to get the full benefit of the stretch.
Purpose: Increases flexibility and reduces stiffness in the neck.
How to Do It:
Tip: Move slowly and avoid forcing the stretch. If you feel pain, stop immediately.
Purpose: Relieves tension in the shoulders and neck, improving blood flow.
How to Do It:
Tip: Perform this exercise slowly and deliberately, focusing on releasing tension in your upper back and neck.
Purpose: Helps release tightness in the upper shoulders and neck, which can contribute to nerve compression.
How to Do It:
Tip: Keep your opposite shoulder relaxed and down to maximize the stretch.
Perform these exercises gently—never force a stretch.
Consistency is key; do them daily for best results.
If you experience sharp pain or worsening symptoms, stop immediately and consult a healthcare provider.
A pinched nerve in your neck can make daily activities difficult, but you don't have to live with chronic pain. You can find relief and restore normal function with proper care, treatment, and lifestyle adjustments. Our spine specialists here at Princeton Orthopaedics Associates are here to help if your symptoms persist or worsen. Reach out today for expert care and personalized treatment options to get you back to living pain-free.
This blog post is meant to be informative and should not act as a self-diagnosis tool. If you’d like to see one of our doctors, please contact us here.
Peroneal tendonitis is a common yet also misunderstood condition affecting the outer portion of your ankle; it can cause you significant discomfort and interfere with your daily activities if left untreated. This condition often arises due to overuse, sudden changes in physical activity, or biomechanical issues that strain the peroneal tendons. While athletes and active individuals are particularly susceptible, anyone can develop peroneal tendonitis if the tendons are subjected to excessive stress. Understanding the anatomy, causes, symptoms, and appropriate care is crucial for effective management and prevention.
Understanding peroneal tendonitis, its anatomy, common causes, symptoms, treatment options, and how to prevent it can help you recover and get out of pain!
Peroneal tendonitis, also known as peroneal tendinopathy, can also be referred to by other names, including:
Peroneal tendonitis refers to irritation or inflammation of the peroneal tendons, which run along the outer side of your ankle. These tendons are important for stabilizing your ankle joint and facilitating foot movement. When these tendons become inflamed, they can cause pain, swelling, and reduced mobility. This condition is most frequently seen in individuals who engage in repetitive ankle movements, but it can also arise from acute injuries or biomechanical abnormalities.
Peroneal tendonitis typically develops due to overuse, resulting in micro-tears and inflammation within the tendons. This condition can occur in one ankle (unilateral) or, less commonly, in both ankles (bilateral).
Peroneal tendonitis can result from various causes, often related to repetitive motion or biomechanical stress. Identifying and addressing these underlying causes is key to both treatment and prevention.
Athletes who engage in activities involving repetitive ankle movement (e.g., running, hiking, or sports requiring quick lateral motions) are at greater risk. Over time, repetitive stress can lead to micro-tears in the tendons, causing inflammation and pain.
If you have a rapid increase in exercise intensity or frequency, it can strain your peroneal tendons. For instance, starting a new running regimen or abruptly increasing training volume can place excessive stress on the tendons.
If you wear shoes that lack proper support, they can increase stress on the peroneal tendons. Poor arch support or insufficient cushioning can alter your foot mechanics and contribute to the irritation of your tendons.
High arches or an abnormal gait can increase tendon strain. Individuals with these anatomical variations are more prone to overloading the peroneal tendons.
A past ankle injury, like an ankle sprain, can increase your risk of developing peroneal tendonitis. If you have a history of ankle sprains or instability, you can be more susceptible because these injuries can weaken the tendons, making them more prone to inflammation.
Weakness or poor coordination in the ankle can contribute to stress on the tendons.
Abnormalities in the way the foot moves (like flat feet or high arches) can lead to additional stress on the tendons.
Underlying conditions, such as inflammatory arthritis or connective tissue disorders, can also weaken the tendons or increase inflammation, predisposing people to peroneal tendonitis.
These are the common symptoms of peroneal tendonitis:
Experiencing pain along the outer side of your ankle: This pain is usually located behind the bump on the outside of your ankle, the lateral malleolus, and may worsen with movement.
Ankle Swelling and tenderness: The affected area of your ankle may become swollen, and the tendons themselves may also be tender to the touch.
Ankle pain that worsens with physical activity and improves with rest: Activities such as walking, running, or standing for long periods typically aggravate symptoms, but they reduce after rest and avoiding said activities.
A sensation of ankle instability or a snapping feeling: In some cases, the tendons may slip out of their normal position, causing a noticeable snapping sensation.
Stiffness or weakness: Individuals may experience stiffness when moving the ankle, as well as weakness during activities requiring ankle stability.

If you suspect you have peroneal tendonitis, early intervention with home care is essential for symptom management and recovery. Consistent and proactive home care can prevent the condition from worsening and promote healing. Consider the following steps:
While mild cases of peroneal tendonitis may resolve with home care, we recommend you seek medical attention right away if you experience:
Treatment depends on the severity of the condition and may include:
Proactive measures can reduce the risk of developing peroneal tendonitis, especially for those prone to ankle injuries. Consider incorporating the following strategies:
Strengthening Exercises for Peroneal Tendonitis: Targeting the ankle and foot muscles enhances stability and reduces strain. Examples include:
Supportive Footwear: Choose shoes with enough arch support and cushioning, especially for high-impact activities. Custom orthotics may also be beneficial if you have high arches or foot misalignment.
Gradual Progression: Increase physical activity levels gradually to prevent overuse. Sudden increases in intensity or duration should be avoided.
Stretching Routine: Regularly stretch the calf muscles and ankles to maintain flexibility. Flexible tissues are less prone to injury and inflammation.
If you're experiencing persistent ankle pain or instability, it's essential to seek professional care. The specialists at Princeton Orthopaedic Associates are here to provide expert diagnosis and personalized treatment plans. Schedule a consultation today to get back to the activities you love with confidence.

Please contact us! We'd love to help.
If you have pain, please contact us and schedule an appointment. We have urgent care facilities all over New Jersey for your convenience.
If you're experiencing hand cramps, or muscle cramps in your hands, it can significantly affect your daily activities. Whether you're typing on a keyboard, cooking a meal, or simply opening a bag or a jar, hand cramps can make these simple, everyday tasks frustrating and sometimes painful. For some people, hand cramps may start subtly—a slight stiffness or discomfort that comes and goes. Over time, the cramps may become more intense and frequent, interfering with work, hobbies, and everyday routines.
Hand cramps are a common yet bothersome issue that can affect anyone. These sudden, involuntary muscle contractions in the hands can cause discomfort, disrupt daily routines, and strike at the most inconvenient times. Understanding why you're experiencing hand cramps is the first step toward finding relief and preventing future episodes.
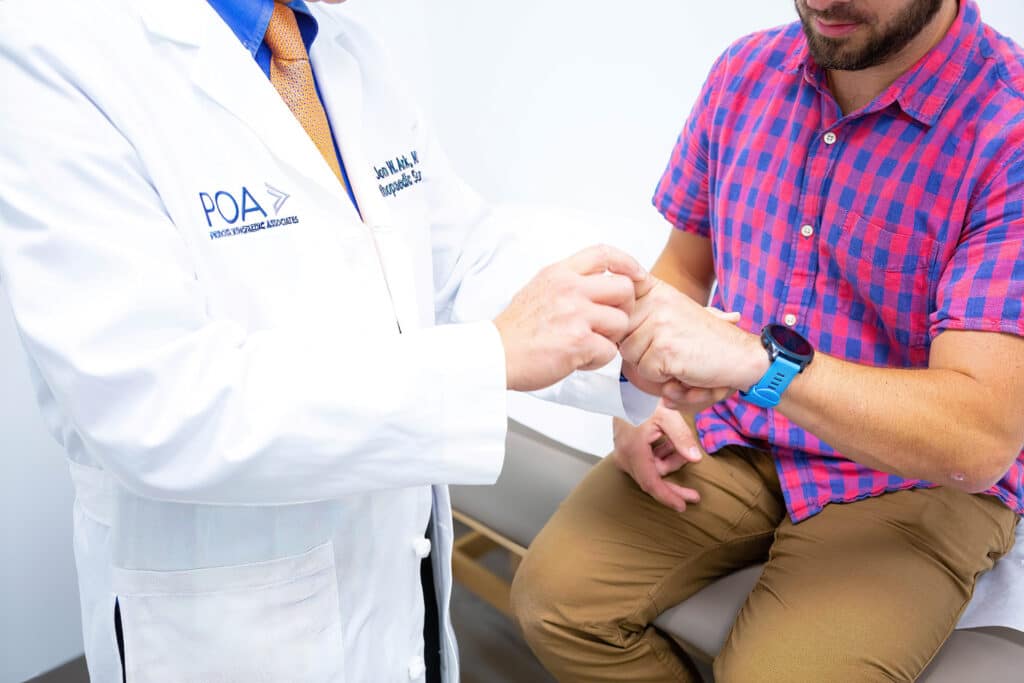
Hand cramps are involuntary muscle spasms or contractions in your hands and fingers. They can appear gradually and range from mild twitching to intense pain and stiffness. Initially, you may notice a mild tightening or twitching sensation in your fingers or palm. As the cramps progress, the stiffness can become more pronounced, sometimes accompanied by sharp or throbbing pain. You might experience involuntary muscle spasms, making it difficult to control fine motor movements.
They can last a few seconds or persist for several minutes and worsen without intervention, making it difficult to use your hands comfortably. Occasional hand cramps may be harmless, but persistent or severe cramping could indicate an underlying health issue that needs attention.
It can be easy to ignore or push away the issues you are having with hand cramps, but recognizing the symptoms of when hand cramps are an issue can help you identify and manage them effectively.
While the individual intensity and duration of cramps can vary, the following symptoms are common:
Sudden Muscle Contractions:
Experiencing sudden, involuntary tightening or spasms in the hand muscles that occur unexpectedly and range from mild to severe.
Tingling or Numbness:
Experiencing a prickling sensation or temporary loss of feeling, often caused by poor circulation or nerve compression, may accompany you hand cramps.
Stiffness:
Reduced flexibility in the hands and fingers can make movement difficult and impede the completion of daily tasks.
Pain and Discomfort:
It's common to experience mild to severe aching or sharp pain accompanying muscle cramps; this pain may also linger after the cramp subsides.
Tightness or Swelling:
Experiencing a sensation of fullness or visible swelling in the affected area can indicate muscle strain or fluid retention, further contributing to discomfort.
Fingers Curling or Locking:
Temporary and involuntary bending of the fingers, causing temporary stiffness or difficulty straightening them.
Difficulty Gripping Objects:
Struggling to hold or carry items due to hand stiffness, weakness, or sudden cramps.
Certain daily activities can increase the likelihood of experiencing hand cramps due to muscle strain or fatigue. Identifying your specific triggers can help you make changes to reduce the frequency and intensity that you experience issues with your hands cramping.
Frequent Typing and Desk Work: Extended periods of typing or using a mouse can strain hand muscles. Poor ergonomics and repetitive movements increase the risk of muscle fatigue, leading to cramps. If you spend hours working on a computer without adequate breaks, your hand muscles may become overworked and become prone to spasms.
Lifting Heavy Objects: Frequent lifting or gripping heavy items can overwork the hand muscles, causing painful cramps and muscle tightness. This is particularly common in professions requiring manual labor or during intensive household tasks.
Waking Up From Sleep: Sleep positions that restrict blood flow or place pressure on the hands can lead to morning hand cramps. You may experience a tight, clenched sensation upon waking up, especially if your hands were in an awkward position during the night.
Cooking and Food Preparation: Repetitive hand motions like chopping, cutting, and stirring can cause muscle strain, resulting in sudden cramping sensations. Prolonged food preparation sessions without breaks can exacerbate the issue.
Sports and Physical Activity: Activities that require repeated or forceful hand movements, such as tennis, golf, or weightlifting, can cause cramping due to muscle overuse. Athletes and fitness enthusiasts who push their muscles without sufficient recovery time are particularly vulnerable.

Several physical factors can contribute to hand cramps. Identifying the underlying cause is crucial for effective treatment and prevention.
Here are the most common causes:
Muscle Overuse and Fatigue: Repetitive hand movements without adequate rest can fatigue the muscles, causing cramps. This is common in individuals who type extensively, play musical instruments, or perform manual labor. Overuse can lead to muscle strain, which increases the likelihood of involuntary contractions.
Dehydration: Insufficient hydration can disrupt the balance of electrolytes like potassium and magnesium, leading to muscle cramps. Muscles rely on proper fluid levels to contract and relax efficiently, so staying well-hydrated is essential to maintain optimal muscle function.
Poor Circulation: Conditions that impair blood flow, such as Raynaud's disease or carpal tunnel syndrome, can cause hand cramps by limiting oxygen delivery to muscles. Restricted circulation reduces the availability of essential nutrients, increasing the risk of cramping.
Nutrient Deficiencies: A lack of essential minerals, particularly magnesium, potassium, and calcium, can increase the likelihood of muscle cramps. These nutrients play a vital role in muscle contraction and nerve function, and a deficiency may lead to frequent spasms.
Underlying Medical Conditions: Chronic health issues like arthritis, diabetes, and thyroid dysfunction can affect nerve and muscle health, leading to frequent hand cramps. Neuromuscular conditions can interfere with the normal function of your muscles and cause persistent cramping.
If you want to get rid of muscle cramps in your hands, several strategies can provide immediate relief and help prevent future occurrences. Implementing these techniques can reduce the severity and frequency of cramps:
Stretching and Gentle Exercise: Perform regular hand and finger stretches to maintain flexibility and reduce muscle tension. Gentle stretching increases blood flow, helps muscles relax, and alleviates cramps while preventing future occurrences.
Stay Hydrated: Ensure you drink plenty of water throughout the day to prevent dehydration and maintain proper electrolyte balance. Hydrated muscles are less likely to cramp, especially during periods of physical activity.
Warm Compress: Applying a warm compress or soaking your hands in warm water can soothe cramped muscles and enhance blood flow, relieving stiffness and discomfort. Heat therapy can be particularly effective when cramps are caused by poor circulation or muscle fatigue.
Massage Therapy: Gently massaging the cramped muscles improves circulation and promotes muscle relaxation. Apply light pressure to the affected area using your opposite hand to ease tension and encourage blood flow.
Ergonomic Adjustments: Optimize your workstation with ergonomic tools to reduce strain on your hands. Use a comfortable chair, position your keyboard properly, and take regular breaks to stretch. These adjustments can prevent repetitive strain and muscle fatigue.
Dietary Supplements: If you have a confirmed nutrient deficiency, consider taking magnesium or potassium supplements after consulting with a healthcare professional. These minerals play a crucial role in muscle relaxation and nerve signaling, which can prevent future cramps.
While occasional hand cramps are usually harmless, persistent or severe cramps may indicate an underlying medical condition. You should consult an orthopaedic hand specialist if you experience:
Our hand specialists can diagnose the cause of your hand cramps and recommend appropriate treatments, such as physical therapy, medication, or specialized care.
If you are prone to experiencing hand cramps, you can reduce the frequency and intensity of hand cramps by taking proactive measures.
Similar to treatment for hand cramps but not quite the same, here are some prevention tips:
Experiencing hand cramps can be uncomfortable and disruptive to your daily functioning. Understanding their causes and adopting preventive measures can help you manage and reduce their occurrence. However, if you are dealing with persistent symptoms, seeking medical advice is essential to identify and address any underlying health conditions and set you down the right treatment path.

Please contact us! We'd love to help.
If you have pain, please contact us and schedule an appointment. We have urgent care facilities all over New Jersey for your convenience.
This blog post is meant to be informative and should not act as a self-diagnosis tool. If you’d like to see one of our doctors, please contact us here.
© 2025 Princeton Orthopaedic Associates. The contents of PrincetonOrthopaedic.com are licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. Copying without permission is strictly forbidden. Privacy Policy | Accessibility
