
Book An Appointment
Physician Assistants
Physical & Occupational Therapists
KneeMRI ScansNon-OperativePhysiatry
Physical Therapy
Podiatry
Spine
Sports Medicine
TraumaUrgent Care
X-Ray Imaging

Trigger finger, also called stenosing tenosynovitis, happens when a finger or thumb catches, clicks, or locks as you try to bend or straighten it. We explain why it occurs, the most common symptoms, how doctors diagnose it, and the treatment options that help you get back to comfortable hand use.
If you feel a pop in your palm or need to use your other hand to straighten a finger, you are not alone. This condition is common, often treatable without surgery, and very responsive to early care.
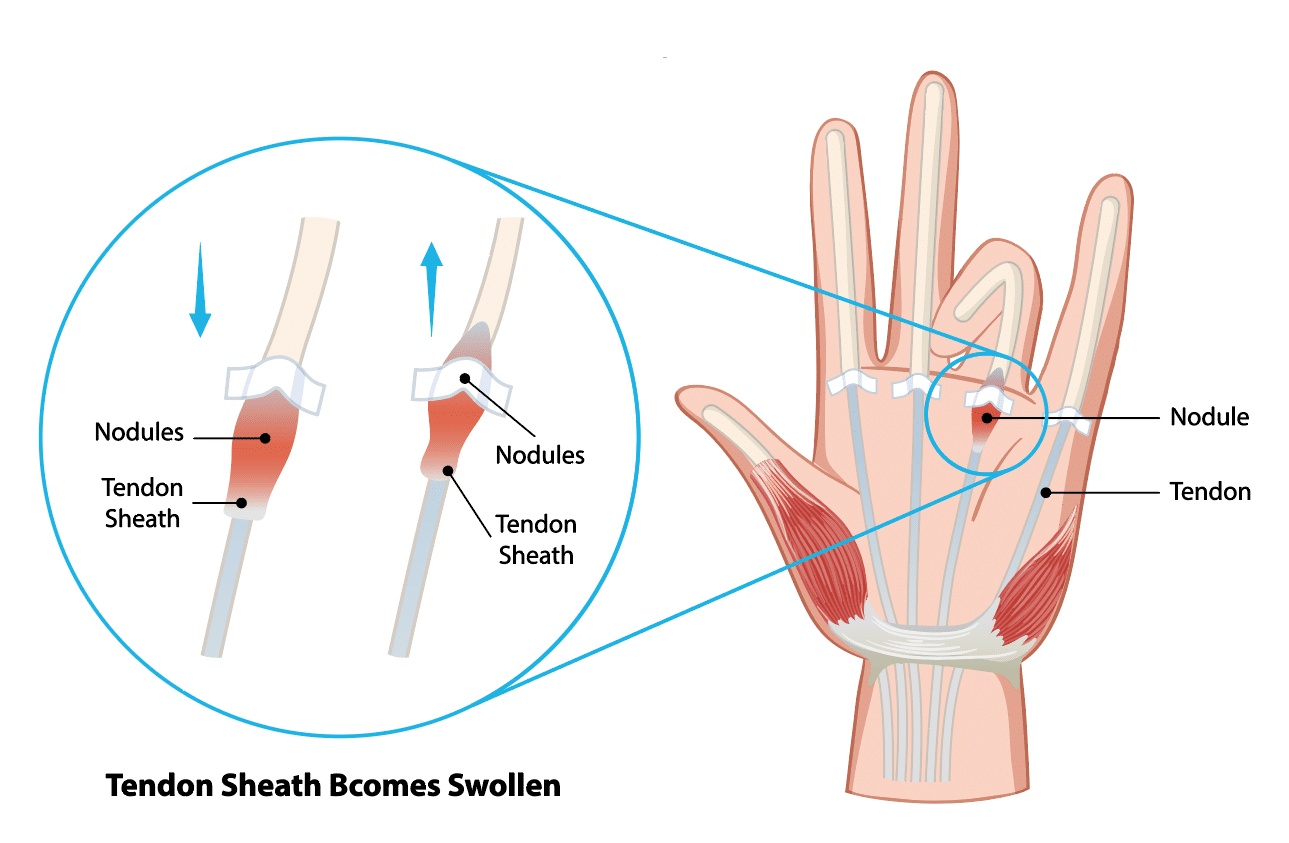
Your flexor tendons glide through tunnels in the palm called pulleys. With trigger finger, the tendon lining and the A1 pulley at the base of the affected finger or thumb become irritated and thickened. That narrowing makes the tendon catch as it moves, which creates clicking or locking.
Most people notice symptoms gradually, developing over days or weeks rather than all at once. At first, you may feel stiffness when you wake up, which improves as you use your hand. You might also notice a dull ache at the base of the finger near the palm, and a tendency for the finger to catch or click as you move it.

Several factors can irritate or swell the tendon and its sheath, which tightens the space the tendon needs to glide.
Diagnosis relies on what you tell the clinician and a careful examination of the hand. The doctor checks for tenderness over the A1 pulley, watches how the finger moves, and may feel a small lump along the tendon. Imaging tests are not usually needed unless the exam is unclear.
Many people improve without surgery, especially when care starts early. The goals are to calm irritation, help the tendon glide smoothly, and reduce stress on the pulley. You may change how you use your hand, rest the affected finger with a removable splint, and work with a therapist. In some cases, a corticosteroid injection helps reduce swelling and catching.
If symptoms persist, the finger locks frequently, or injections and splinting do not help, surgery can be a good option. The procedure is called an A1 pulley release. The surgeon widens the tight opening at the base of the finger so the tendon can glide smoothly again.
Your care plan is tailored to how your hand feels, your medical history, and what you want to return to doing. The plan explains options from less invasive treatments to surgery and describes what to expect at different stages. You and your clinician work together to choose the best path for you.
| Situation | First Steps | If Symptoms Persist |
|---|---|---|
| Mild clicking and morning stiffness | Activity changes, splinting, ice, hand therapy | Consider corticosteroid injection |
| Frequent triggering that interferes with work or self-care | Corticosteroid injection and targeted therapy | Discuss surgical release |
| Locked finger or long-standing symptoms | Prompt evaluation by a hand specialist | Surgical release is often recommended |
After treatment, moving the hand in a steady, gentle way helps the tendon glide smoothly and reduces stiffness. Whether you had nonsurgical care or surgery, follow the recommended exercises and gradually return to daily tasks. Protect the palm from heavy pressure until it feels comfortable and strong again.
Schedule an evaluation if any of the following apply:
Princeton Orthopaedic Associates treats trigger finger with careful evaluation and a plan that fits your goals. The team offers nonoperative options first and uses precise surgical release when needed. If your finger catches, clicks, or locks, you can regain comfortable hand use. Call to schedule an appointment to begin.

Please contact us! We'd love to help.
If you have pain, please contact us and schedule an appointment. We have urgent care facilities all over New Jersey for your convenience.
This blog post is meant to be informative and should not act as a self-diagnosis tool. If you’d like to see one of our doctors, please contact us here.
Shoulder labrum tears can cause deep shoulder pain, clicking, or a sense that the joint might slip. You'll learn what the labrum does, how tears happen, the most common symptoms, how we diagnose the problem, and which treatments can help you return to daily activities and sports safely. By understanding what causes labrum tears and the steps involved in evaluation and treatment, you can ask informed questions, set realistic goals, and participate actively in recovery with your care team.
The shoulder labrum is a rim of cartilage that lines the shallow socket of the shoulder joint, called the glenoid. It deepens the socket, cushions the joint, and helps your ligaments and biceps tendon keep the ball of the shoulder centered.
When the labrum tears, the joint can feel painful or unstable. Some people notice catching, clicking, or a drop in strength when lifting, pushing, or reaching overhead.
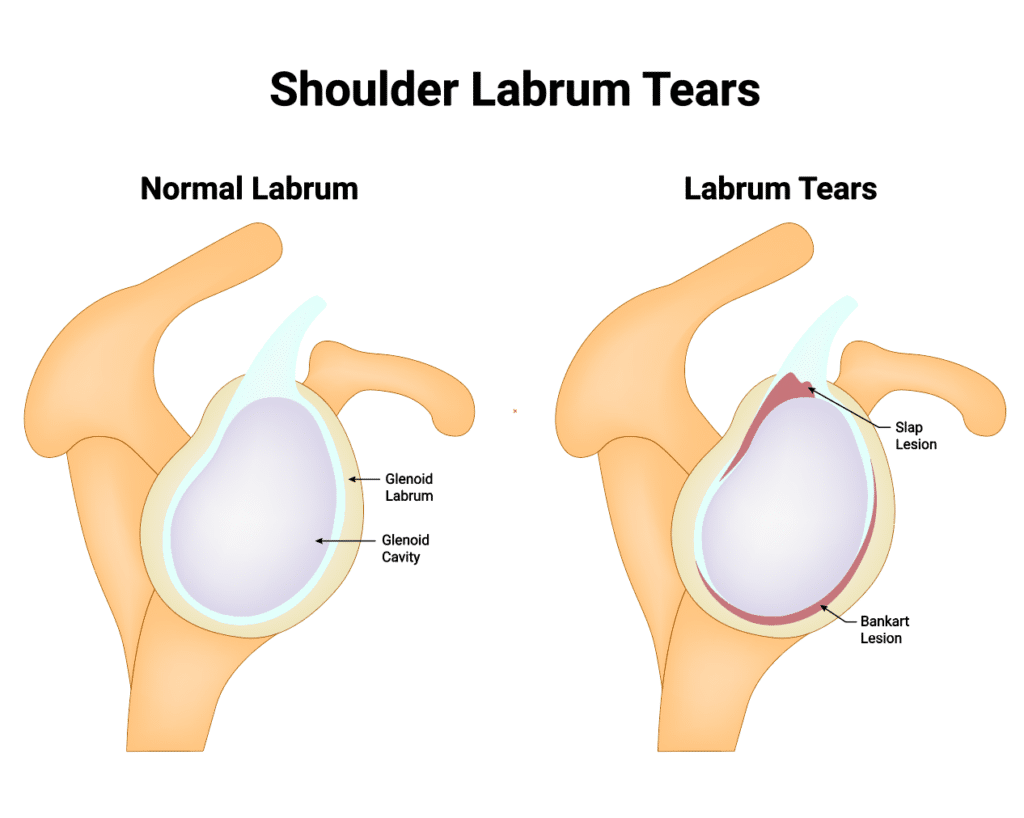
Several patterns of tearing can occur depending on where the labrum is injured and how the injury happened.
| Type | Location | Typical Cause | Common Symptoms | Typical Treatment Approach |
|---|---|---|---|---|
| SLAP Tear (Superior Labrum Anterior to Posterior) | Top of the socket where the biceps tendon attaches | Overhead sports, falls on an outstretched arm, wear-and-tear | Pain with overhead use, clicking, reduced throwing power | Physical therapy, activity modification; arthroscopic repair or biceps procedures when needed |
| Bankart Tear | Front-lower portion of the labrum | Shoulder dislocation or subluxation | Instability, repeated dislocations, apprehension with abduction/external rotation | Rehab to restore control; arthroscopic Bankart repair for recurrent instability |
| Posterior Labral Tear | Back portion of the labrum | Forceful pushing, blocking, falls, repetitive loading | Deep posterior pain, clicking, pain with pushing or bench press | Rehab focused on scapular/rotator cuff control; arthroscopic repair if instability persists |
Symptoms can vary depending on the type of labrum tear and your level of activity, but several signs are common across many cases. People may notice deep shoulder pain during lifting or overhead work, a sensation of catching or grinding within the joint, and reduced strength when pushing or throwing. Some experience night pain or reduced range of motion compared with the other shoulder. These patterns help guide evaluation and treatment choices.
Diagnosis starts with a detailed history and a hands-on exam that includes specific tests to stress different parts of the labrum and shoulder. We assess shoulder blade position, rotator cuff strength, and signs of instability.
Imaging often includes X-rays to evaluate the bones and joint alignment. An MRI, sometimes with a small amount of contrast dye in the joint, can help show the labrum and associated soft-tissue injuries.
Many labrum tears improve without surgery, especially when pain is the main issue and the shoulder is stable.
If pain or instability persists despite focused rehab, arthroscopic surgery may be recommended. Through small incisions, your surgeon can evaluate the labrum and repair or trim damaged tissue as appropriate.
Recovery depends on the type of tear, the procedure performed, and your sport or job demands. The general ranges below are common starting points that your surgeon and therapist will personalize.
| Phase | Typical Timeframe | Focus |
|---|---|---|
| Sling/Protection | 2-4 weeks after debridement; 4-6 weeks after repair | Protect healing tissue, gentle hand/elbow motion, pain control |
| Early Motion | Weeks 2-8 after debridement; Weeks 4-10 after repair | Restore range of motion under guidance, avoid provocative positions |
| Strength & Control | Months 2-4 | Scapular and rotator cuff strength, posture, gradual load |
| Return to Sports/Work | 3-4 months for non-contact after debridement; 4-6+ months after repair | Progressive sport-specific drills; throwing programs may take longer |

If shoulder pain, clicking, or instability is limiting you, we’ll examine your shoulder, review imaging when needed, and create a plan that fits your goals. Most people start with focused rehab, and when surgery is the best path, your team will guide you each step of the way.
Schedule an evaluation with Princeton Orthopaedic Associates to get moving comfortably again.

Please contact us! We'd love to help.
If you have pain, please contact us and schedule an appointment. We have urgent care facilities all over New Jersey for your convenience.
This blog post is meant to be informative and should not act as a self-diagnosis tool. If you’d like to see one of our doctors, please contact us here.
Iliotibial band syndrome, or more commonly called the IT Band, is a common source of aching on the outside of the knee or thigh. Below, you’ll learn what the iliotibial band is, why it gets irritated, how symptoms show up in daily life and sport, and the treatments that help you return to comfortable movement.
Whether you run, cycle, walk for exercise, or spend long hours sitting, this condition can affect how your hip and knee work together. The good news is that most people improve with a plan that reduces irritation and restores strength and mobility around the hip and knee.
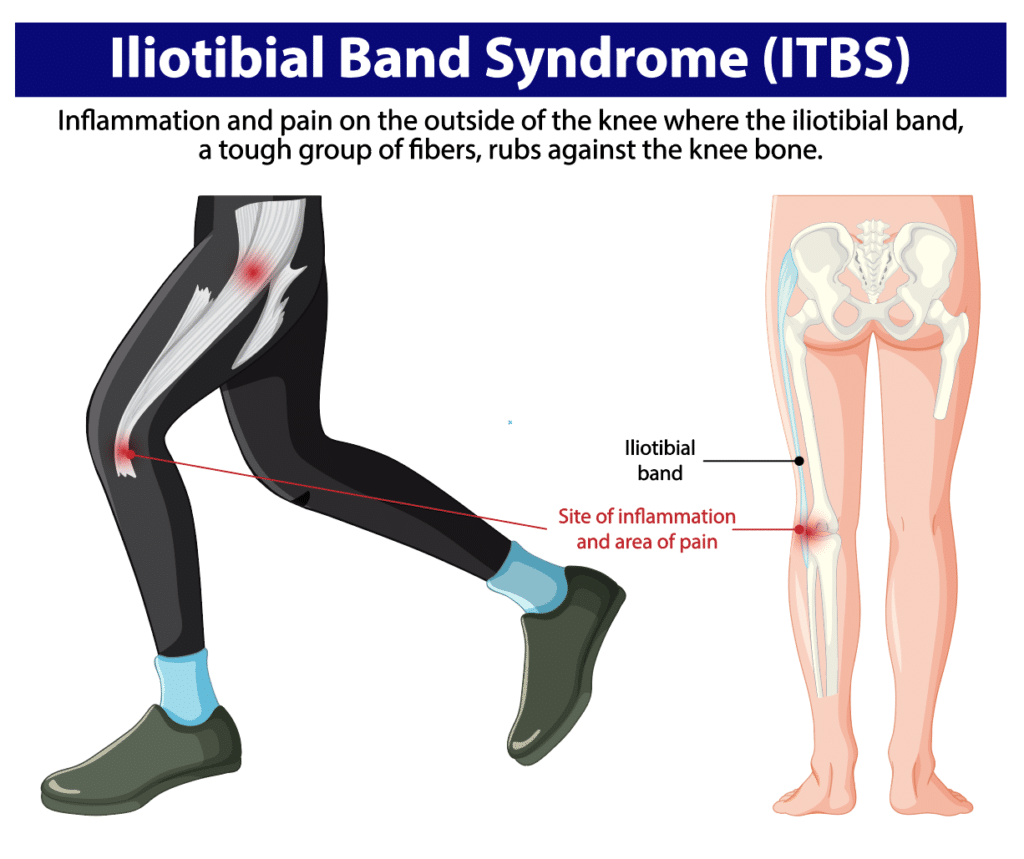
The IT band is a thick, fibrous band that supports the outside of your thigh. It connects muscles near the hip to the shinbone and helps stabilize the knee during walking, running, and standing.
Symptoms arise when tissues deep to the IT band (such as a fat pad or bursa) are compressed against the lateral femoral epicondyle during repetitive knee flexion and extension. This compression leads to irritation and pain on the outer knee, and may be felt higher up the thigh or into the hip.
Symptoms often begin gradually and worsen with repetitive flexion and extension of the knee, such as during running, cycling, or climbing stairs. People commonly describe a mix of pain on the outer knee, tightness along the outside of the thigh, tenderness when the outer knee is touched, and discomfort that changes with movement. The pain can flare with activity but may ease with rest, and occasional stiffness after sitting is not required for the diagnosis.
Symptoms often begin gradually and tend to worsen with repetitive activities. People describe:
IT band irritation usually stems from how the leg moves and how much load it is asked to handle. Multiple factors can combine to create friction near the outer knee.
A sports medicine or orthopaedic clinician typically diagnoses IT band syndrome through your history and a focused exam. They’ll check tender areas along the outer knee and hip, assess hip and core strength, and look for tightness in surrounding muscles.
Imaging is not always needed. X-rays or an MRI may be ordered when symptoms are atypical, severe, or to rule out other causes of outer knee pain such as arthritis, meniscus problems, or stress injuries.
Most people recover with a stepwise approach that calms irritation and corrects the movement issues that caused it.
For persistent pain, a clinician may consider a carefully selected corticosteroid injection in the area of irritation (often image-guided). Injections should be used judiciously as part of a broader rehab plan. Surgery is rarely needed and is considered only when symptoms fail to improve after a thorough course of nonoperative care.
Healing time varies based on how long symptoms have been present, training demands, and how consistently you follow your plan. These general ranges are common:
| Stage | Typical Timeframe | What to Expect |
|---|---|---|
| Early | Several weeks | Pain reduces with activity changes, icing, and basic mobility work. |
| Established | 1 to 3 months | Strength and movement retraining restore tolerance for daily life and sport. |
| Recurrent or Chronic | Longer than 3 months | More comprehensive rehab and training plan adjustments are needed. |
Prevention means keeping movement balanced and building strength around the hip and knee. A simple plan can help avoid flare-ups: gradually increase activity, vary routes, stretch key muscles, and choose footwear that fits your needs. Regular rest breaks and listening to your body are important to prevent irritation from returning.
Schedule an evaluation if pain lasts more than a week, returns when you resume activity, or changes how you walk or run. Early guidance helps you recover faster and reduces the risk of the problem becoming chronic.
| Specialty | Best For | Notes |
|---|---|---|
| Sports Medicine | Activity-related knee and hip pain; nonoperative care | First stop to confirm diagnosis and plan treatment |
| Physiatry | Movement analysis and musculoskeletal pain | Addresses posture, gait, and functional limitations |
| Orthopaedic Surgery | Persistent or complex cases | Coordinates imaging or advanced options if needed |
| Physical Therapy | Strength, flexibility, and gait retraining | Guides a graded return to activity and long-term prevention |
IT band syndrome can interrupt training and make everyday tasks frustrating, but it is highly treatable. With the right mix of activity changes, targeted strengthening, mobility work, and expert guidance, you can ease pain and return to the activities you enjoy.
Foot pain can come from many sources, from irritated tendons and tight fascia to nerve irritation and arthritis. Here, you’ll find a clear overview of why feet hurt, how to tell what might be going on, and the proven ways we help people heal and stay active.
Whether your foot pain is new or has lasted for months, know how your pain acts, where it hurts, and how it changes with walking or standing. This helps you find relief faster. You can start practical steps today and use the medical options we choose when home care does not work.

Your foot has 26 bones, numerous joints, strong ligaments, and powerful tendons. This complex design allows it to absorb shock, stabilize the body, and push you forward with every step.
Problems arise when tissues are overworked, inflamed, worn by arthritis, or irritated by pressure or footwear. The plantar fascia, Achilles tendon, and small nerves between the toes are frequent sources of symptoms.
Use this guide to match common pain locations with frequent causes and typical clues. A precise diagnosis still requires an exam.
| Region | Possible Causes | Typical Clues |
|---|---|---|
| Heel | Plantar fasciitis, Achilles tendinitis, heel spur, stress fracture, bursitis | First-step pain in the morning, pain after sitting, tenderness under the heel or back of heel |
| Arch / Bottom of Foot | Plantar fasciitis, posterior tibial tendon issues, flatfoot strain | Aching along the arch, worse with prolonged standing or long walks |
| Ball of Foot / Toes | Metatarsalgia, Morton neuroma, sesamoiditis, hammertoe irritation | Burning or pebble-like feeling under the forefoot, numbness between toes |
| Top of Foot / Midfoot | Extensor tendinitis, midfoot arthritis, Lisfranc sprain, stress fracture | Pain with lacing shoes tightly, swelling on top, pain with push-off |
| Outer Foot / Ankle | Ankle sprain, peroneal tendinitis | Tenderness along outer ankle or foot, pain on uneven ground |
| Big Toe Joint | Bunion, hallux rigidus, turf toe, gout | Prominent bunion, stiffness or grinding, sudden redness and swelling with gout |
Your specialist begins with a careful history and hands-on exam. We look at where it hurts, when it hurts, your footwear, and how you walk.
The goal is a clear diagnosis, so your treatment targets the true source of pain.
Most foot pain improves with a combination of activity changes, shoe adjustments, focused exercises, and targeted medical care. Your plan will be tailored to your diagnosis and goals.
If foot pain is limiting your day, we’re here to help you find the cause and create a clear plan forward. Schedule an exam with a Princeton Orthopaedic Associates specialist to start moving comfortably again.

Please contact us! We'd love to help.
If you have pain, please contact us and schedule an appointment. We have urgent care facilities all over New Jersey for your convenience.
This blog post is meant to be informative and should not act as a self-diagnosis tool. If you’d like to see one of our doctors, please contact us here.
A strong back line, called the posterior chain, helps you stand tall and move well. It may help protect your spine, and it supports everyday tasks like lifting, climbing stairs, and getting up from a chair. It covers what the posterior chain includes, why it matters for back and knee comfort, easy form cues, and safe exercises you can start today.
We’ll also outline how often to train, common mistakes to avoid, and when it may be helpful to see a clinician at Princeton Orthopaedic Associates for personalized care and safer progress.
Please note that these exercises are listed here as examples. You will absolutely need to consult with a qualified doctor, trainer, or medical professional to decide if this information is right for you. You can cause harm to yourself by doing exercises incorrectly or those that do not align with your body or desired outcomes. Please be careful!

The posterior chain runs along the back of the body and is made of muscles that help keep the spine steady and allow the hips to extend. These muscles work together with many daily activities, such as standing, walking, lifting, and climbing stairs, so keeping them strong can support good posture and ease movement. Keeping this area strong supports your posture and reduces strain during daily activities.
The hip hinge is the foundation of many posterior chain moves. Instead of bending your back, shift your hips back while keeping your spine in a comfortable neutral range so the glutes and hamstrings do the work.
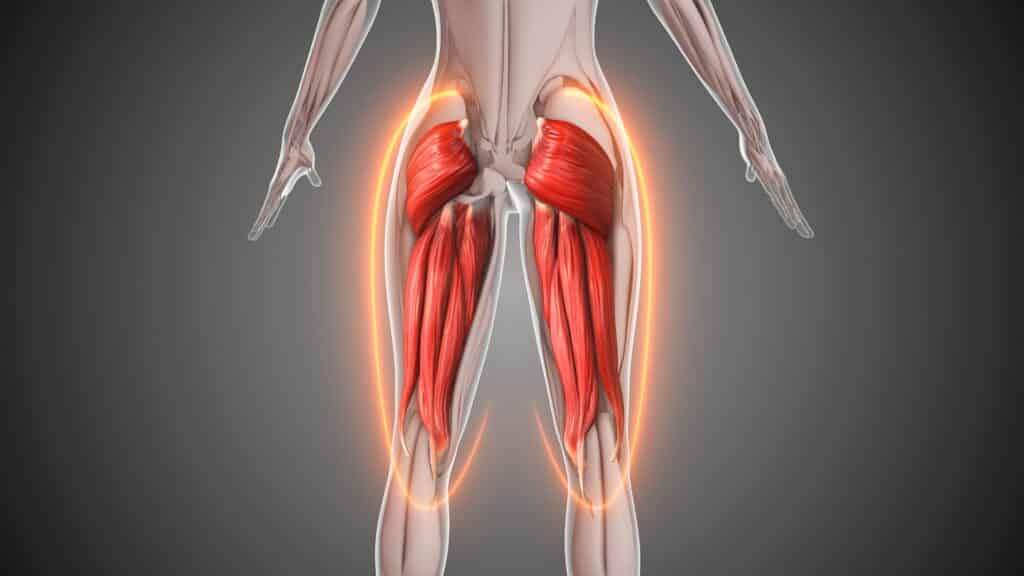
Practice by lightly touching your hips to a wall behind you or sliding your palms down your thighs to learn the pattern.
Choose 3 to 5 movements that feel comfortable and fit your body. Do each with slow, controlled reps and steady breathing. Focus on keeping good muscle control rather than rushing to finish. This careful approach helps you learn the pattern and build strength safely.
| Exercise | Main Muscles | How to Do It | Reps |
|---|---|---|---|
| Glute Bridge | Glutes, hamstrings | Lie on your back, knees bent, feet hip-width. Exhale and lift hips until shoulders, hips, and knees line up. Pause, then lower with control. | 8 to 12 |
| Hip Hinge to Wall | Glutes, hamstrings | Stand a foot from a wall. Push hips back to tap the wall while maintaining a comfortable neutral range in your spine, then stand tall. | 8 to 12 |
| Romanian Deadlift (light dumbbells) | Glutes, hamstrings, back stabilizers | Hold weights by your thighs. Hinge at the hips with soft knees until you feel hamstring tension, then press through heels to stand. | 6 to 10 |
| Hamstring Curl (exercise ball or sliders) | Hamstrings, glutes | Bridge hips, then bend knees to roll the ball or sliders toward you. Keep hips lifted and trunk steady. | 8 to 12 |
| Bird Dog | Spinal stabilizers, glutes | On hands and knees, brace your core. Reach opposite arm and leg long without arching the back. Pause, switch sides. | 6 to 10 each side |
| Step-up | Glutes, calves | Stand a foot from a wall. Push your hips back to tap the wall while maintaining a comfortable neutral spine, then stand tall. | 8 to 12 each side |
Most people benefit from training the posterior chain on nonconsecutive days so the muscles have time to rest and recover. Spacing workouts helps you keep good form and avoid overload. Consistent practice slowly builds strength and control while protecting your knees and back.
| Level | Frequency | Sets x Reps | Notes |
|---|---|---|---|
| Beginner | 2 days per week | 1 to 2 sets of 8 to 12 reps | Prioritize form and slow tempo; stop a rep or two before fatigue changes your form. |
| Intermediate | 2 to 3 days per week | 2 to 3 sets of 6 to 12 reps | Increase load gradually when all reps feel steady and controlled. |
Safety note: Individuals with osteoporosis, acute low back or radicular pain, or recent postoperative status should consult a clinician before hip hinging or deadlifting.
If pain limits your daily activities, you’re unsure about your form, or you have had a recent injury, consider seeing an orthopaedic specialist. Getting advice early can help you avoid delays, keep your movement safe, and build strength steadily. A clinician can check your technique and tailor exercises to your needs.
At Princeton Orthopaedic Associates, we evaluate the way you move, identify which muscles need attention, and create a clear plan to reach your goals. If needed, we coordinate care with physical therapy to help you progress step by step.

Please contact us! We'd love to help.
If you have pain, please contact us and schedule an appointment. We have urgent care facilities all over New Jersey for your convenience.
This blog post is meant to be informative and should not act as a self-diagnosis tool. If you’d like to see one of our doctors, please contact us here.
Knee pain after a run is common, whether you are new to running or building mileage. Below you will find the most frequent causes, how to tell what is driving your pain, simple steps to feel better, and when it is time to schedule an exam with our team at Princeton Orthopaedic Associates.

Use this guide to match your pain pattern with likely sources. An exam is the best way to confirm the diagnosis.
| Location of Pain | Possible Cause | Common Triggers |
|---|---|---|
| Front of the knee or behind the kneecap | Patellofemoral pain syndrome (runner’s knee) | High-impact mileage, prior injuries, and age-related changes |
| Sprinting, jumping, high-load quad work | Iliotibial band syndrome | Downhills, slanted roads, sudden mileage increases |
| Outside of the knee | Patellar tendinopathy | Hills, stairs, prolonged sitting, weakness of the hips or quads |
| Repetitive kneeling, direct pressure, and overuse | Meniscal irritation or tear | Twisting, deep knee bends, uneven terrain |
| Stiffness and swelling after activity | Knee osteoarthritis | Inside line of the knee or catching sensation |
| Warmth or tenderness near the kneecap | Bursitis | Repetitive kneeling, direct pressure, overuse |
Running multiplies the force through your knees with every step. Small issues in strength, flexibility, or form can add up over thousands of strides.
These steps are safe for most runners and are intended to reduce irritation while protecting the knee. Start by reducing hard miles and hills, then gradually resume activity as comfort returns. If pain persists for more than a week despite rest, or if you notice swelling, catching, or weakness, consult a clinician promptly.
These conditions often respond well to targeted rehab and training changes.
| Condition | What It Is | Helpful Strategies |
|---|---|---|
| Patellofemoral pain | Irritation where the kneecap tracks over the femur | Hip and quad strengthening, taping or bracing, cadence work, hill modification |
| Iliotibial band syndrome | Compression/impingement of tissues over the lateral femoral epicondyle and adjacent fat pad (commonly referred to as IT band syndrome). | Gradual loading, eccentric and isometric quad exercises, and manage jumping volume |
| Patellar tendinopathy | Overload of the tendon below the kneecap | Reduce twisting and deep knee bends, progressive strengthening, and imaging if persistent |
| Meniscal irritation | Stress or tearing of shock-absorbing cartilage | Strength, low-impact cardio, weight management, activity modification |
| Knee osteoarthritis | Wear of joint cartilage with age or prior injury | Gradual loading, eccentric and isometric quad exercises, and managing jumping volume |
If knee pain is keeping you from the miles you love, we can help you identify the cause and build a clear plan back to comfortable running.

Please contact us! We'd love to help.
If you have pain, please contact us and schedule an appointment. We have urgent care facilities all over New Jersey for your convenience.
This blog post is meant to be informative and should not act as a self-diagnosis tool. If you’d like to see one of our doctors, please contact us here.
Pain that starts in the lower back or buttocks and travels down one leg is often linked to irritation or pressure on the sciatic nerve. Gentle stretching can help ease tight muscles, calm nerve sensitivity, and support a gradual return to everyday activities.
These stretches are designed to be gentle and accessible. Move slowly, stay within a comfortable range of motion, and focus on steady breathing. If any movement increases pain, tingling, or numbness, it's best to ease off or skip that stretch. Knowing when and how to stretch, along with what to avoid during flareups, can make a big difference in your recovery. If symptoms persist or worsen, it’s important to consult a medical professional.
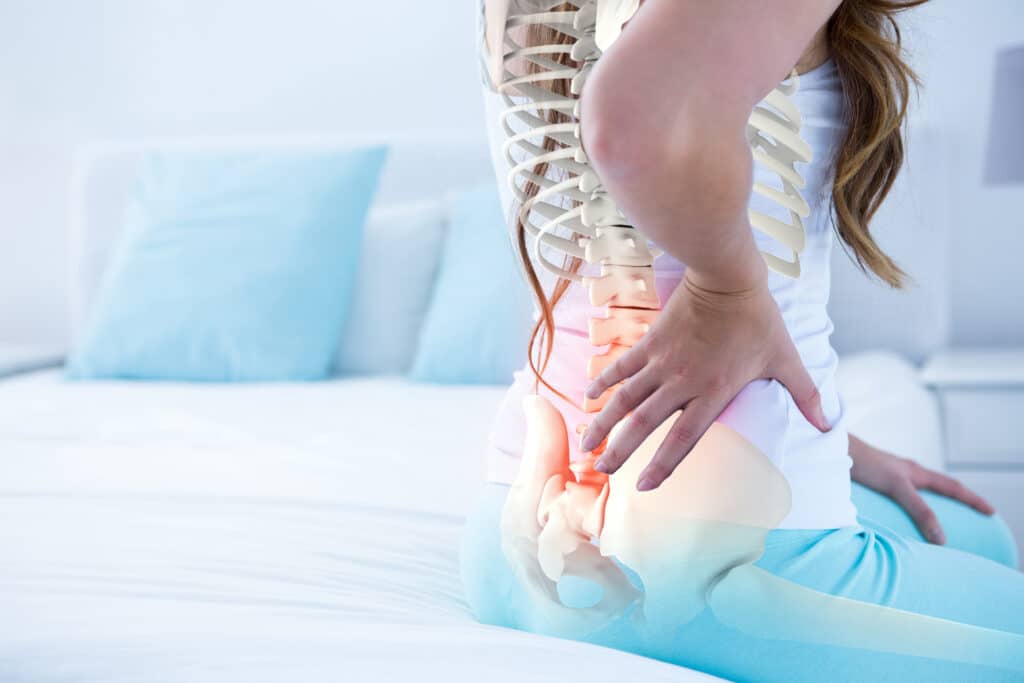
The sciatic nerve is the largest nerve in your body. It forms in the lower spine, travels through the buttock, and runs down the back of each leg. When structures around the nerve get irritated or compressed, pain can spread from the low back or hip into the thigh, calf, or foot.
Causes vary. A lumbar disc can bulge and press on the nerve root. Spinal stenosis narrows the canal that the nerves pass through. Sometimes the deep hip muscles tighten and create local nerve irritation. Your plan should match your diagnosis, which is why an exam is helpful before starting a new routine.

1) Figure-4 Stretch on Back
Lie on your back with knees bent and feet on the floor. Cross the ankle of your painful side over the opposite thigh.
Gently pull the uncrossed thigh toward you until you feel a stretch in the buttock.
Hold 20 to 30 seconds. Repeat 2 to 3 times.

2) Knee to Opposite Shoulder
Lie on your back. Bend the knee on the painful side.
Use both hands to draw the knee across your body toward the opposite shoulder.
Stop at a comfortable stretch in the outer hip. Hold 20 to 30 seconds. Repeat 2 to 3 times.

3) Seated Hamstring Stretch
Sit on the floor with one leg extended straight and the other leg bent, with the sole of the foot resting against the inner thigh of the extended leg. Keep your back straight and shoulders relaxed.
Gently lean forward from your hips, reaching toward your shin, ankle, or foot. Stop when you feel a mild stretch in the back of your thigh. Hold for 15–30 seconds, breathing steadily. Return to upright and switch legs. Repeat 2–3 times on each side.

4) Half-Kneeling Hip Flexor Stretch
Kneel on one knee with the other foot in front. Tuck your tailbone slightly and gently shift your weight forward.
You should feel a stretch in the front of the hip on the kneeling side. Keep your trunk upright.
Hold 20 to 30 seconds. Repeat 2 to 3 times each side.

5) Child's Pose, Comfortable Range
Start on hands and knees. Sit your hips back toward your heels while reaching your arms forward.
Stay where it feels easy to breathe. If you notice leg pain or tingling increases with spinal flexion, reduce the depth or skip this position.
Hold 20 to 30 seconds. Repeat 2 to 3 times.

6) Cat–Cow
On hands and knees, gently arch your back toward the ceiling, then lower your belly toward the floor.
Move slowly with your breath for 30 to 60 seconds. Stop if leg pain increases.

7) Seated Piriformis Stretch
Sit tall. Cross the painful-side ankle over the opposite knee.
Lean forward slightly until you feel a stretch in the buttock. Hold 20 to 30 seconds, repeat 2 to 3 times.
Consistency helps calm sensitive tissues. Use this simple guide to pace your recovery.
| Stage | Frequency | Holds/Reps | Notes |
|---|---|---|---|
| Early pain | 1 to 2 times daily | 20 to 30 second holds, 2 to 3 sets | Stay gentle, avoid positions that trigger leg pain |
| Improving | Daily or every other day | Progress range as comfort allows | Add short walks and easy core work |
| Maintenance | 3 to 5 days per week | Brief routine after activity | Keep flexibility in hips, hamstrings, and low back |
Deep spinal flexion or sustained forward bending if it increases leg symptoms.
Get medical care promptly if any of the following occur:
If sciatic pain is limiting your day, we can help you find the cause and build a plan that fits your life. Our clinicians guide you on safe exercises, posture, and next steps if additional treatment is needed. Schedule an evaluation to get moving comfortably again.

Please contact us! We'd love to help.
If you have pain, please contact us and schedule an appointment. We have urgent care facilities all over New Jersey for your convenience.
This blog post is meant to be informative and should not act as a self-diagnosis tool. If you’d like to see one of our doctors, please contact us here.
Tightness in the front of your hips can make everyday movements like walking, running, or standing up from a chair feel stiff and uncomfortable. Understanding what your hip flexors do, why they become tight, and how to stretch them properly can help improve flexibility and ease discomfort.
The hip flexors are a group of muscles located at the front of the hip that play a key role in lifting the knee and bending at the waist. The iliopsoas and rectus femoris are among the most important of these muscles. Prolonged sitting, repetitive activity, or a sudden increase in physical demand can cause these muscles to become shortened and sore. With gentle, consistent stretching and mindful movement habits, you can usually restore mobility and reduce tightness.
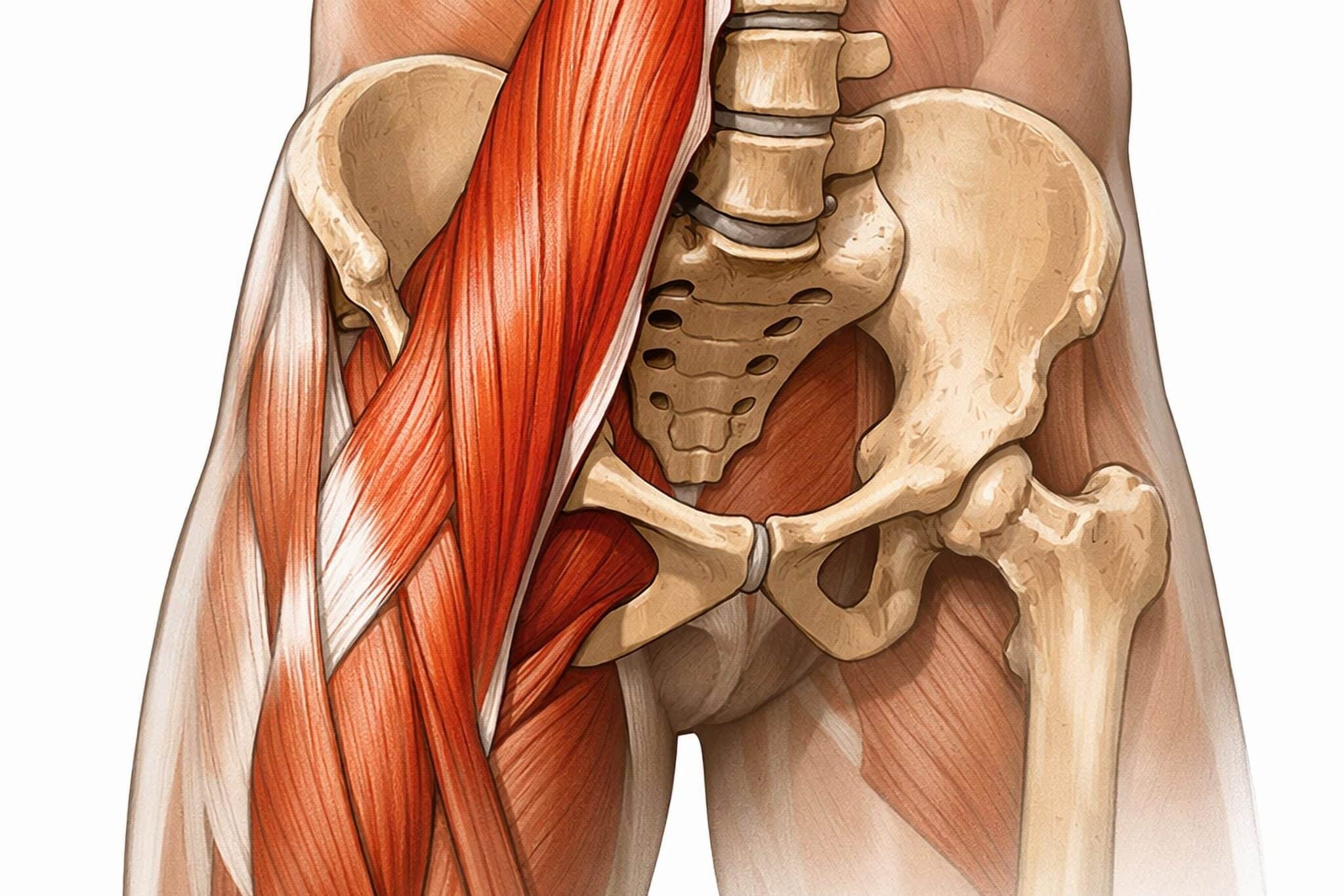
You might notice stiffness in the front of your hip or groin after sitting, or discomfort when you step into a long stride. Other common clues include:

Using the standing lunge with support can help you ease into a hip stretch when kneeling is painful or unstable. This option lets you keep your balance with a chair, table, or counter, which can reduce strain in the knee and back. Start gently, stand tall, and focus on the stretch in the front of the hip. Move slowly and breathe evenly as you feel the stretch deepen.
Good choice if kneeling is uncomfortable or you need extra support.
This position also lengthens the rectus femoris, a front thigh muscle that acts as a hip flexor.
Consistency matters more than intensity when you stretch. A steady, gentle routine helps you move well and stay safe. Use the guide below to build a simple plan that fits your day. Start small with short holds and few days per week, then build up as you feel comfortable and your mobility improves.
| Goal | Time | Frequency | Notes |
|---|---|---|---|
| General flexibility | 20 to 30 seconds per hold | 1 to 2 times daily | 2 to 4 rounds per side |
| Warm up | 5 to 10 seconds gentle holds | Before activity | Prioritize movement quality and posture |
| Mobility maintenance | 20 seconds | 3 to 5 days per week | Pair with hip and core strengthening |
Before sports or vigorous activity, prioritize dynamic warm-ups (e.g., marching, leg swings, hip circles). If you include static stretches, keep them brief and gentle.
Schedule an evaluation at Princeton Orthopaedic Associates if any of the following apply:
We can confirm the cause of your symptoms, teach you the right technique, and build a plan that combines stretching with strength and movement training so your progress lasts.
Hip flexor stretches work best when they’re gentle, well aligned, and consistent. Start with the half-kneeling stretch, focus on pelvic position, and progress to standing or wall variations as you improve. If pain persists, our team is here to help you move with confidence again.

Please contact us! We'd love to help.
If you have pain, please contact us and schedule an appointment. We have urgent care facilities all over New Jersey for your convenience.
This blog post is meant to be informative and should not act as a self-diagnosis tool. If you’d like to see one of our doctors, please contact us here.
f the outside of your knee or hip feels tight or sore, your iliotibial band (IT band) may be involved. You can safely reduce that tension with targeted stretches, proper use of foam rolling, and consistent practice for meaningful relief.
Follow step-by-step stretches that target the muscles connected to the IT band, try a quick 10-minute routine, and be aware of common mistakes to avoid. It’s also important to know when it’s time to see a specialist at Princeton Orthopaedic Associates.
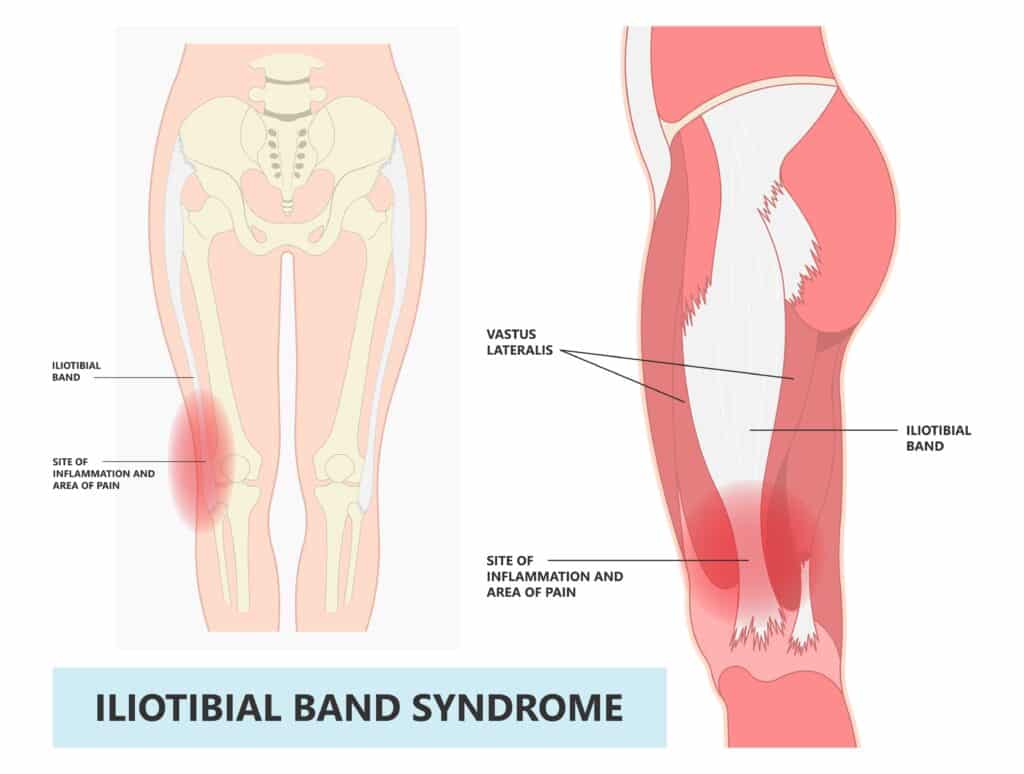
The IT band is a strong band of tissue on the outside of your thigh from your hip to just below the knee. It helps steady the knee while you move. Because it’s not a muscle, you can’t stretch the IT band itself like a hamstring or quad. Instead, you’ll get relief by improving mobility in the muscles that connect to it: the tensor fasciae latae (TFL), glutes, quadriceps, and hamstrings.

Use this quick reference to build a consistent routine. Aim for most days of the week.
| Area | Stretch | Hold | Reps/Side | Frequency |
|---|---|---|---|---|
| TFL/Outer Hip | Standing cross-over lean | 20 to 30 sec | 2 to 3 | 5 to 7 days/week |
| Glutes | Seated figure-4 | 20 to 30 sec | 2 to 3 | 5 to 7 days/week |
| Hip Flexor | Half-kneel with side reach | 20 to 30 sec | 2 to 3 | 5 to 7 days/week |
| Quadriceps | Standing quad stretch | 20 to 30 sec | 2 to 3 | 5 to 7 days/week |
| Hamstring | Supine strap stretch | 20 to 30 sec | 2 to 3 | 5 to 7 days/week |
Foam rolling can help ease soreness and improve movement around the IT band. Focus on the muscles that affect the IT band instead of pressing directly on the band itself. Move slowly, breathe normally, and stop if anything sharp or lingering hurts. This simple tool can make it easier to glide through stretches and daily activities with less tension in the area.
Having balanced strength around your hips and core helps protect the IT band. When the hips and trunk are strong, less stress reaches the outer thigh, and symptoms are less likely to come back. Add simple movements a few days a week to build support and stability for your legs and lower back.
If any of these signs show up, pause your stretches and seek a checkup. A quick evaluation can stop a small issue from turning into a longer lasting problem. Listening to your body now may save you from more pain later.
If you’re unsure which stretches are best for you, our team can help. Sports medicine specialists and physical therapists at Princeton Orthopaedic Associates can tailor a plan to your goals and activity level.

Please contact us! We'd love to help.
If you have pain, please contact us and schedule an appointment. We have urgent care facilities all over New Jersey for your convenience.
This blog post is meant to be informative and should not act as a self-diagnosis tool. If you’d like to see one of our doctors, please contact us here.
If your neck or back feels tight, daily tasks like work, sleep, and exercise can become more difficult. This simple guide offers safe stretches to ease stiffness, improve posture, and help you move more comfortably. You'll learn when to stretch, how long to hold each stretch, and when it might be time to consult a clinician or physical therapist.


These movements target common areas of tightness that can contribute to neck pain, tension headaches, and poor posture.
Tight chest muscles can pull the shoulders forward, which can increase neck strain.
These stretches focus on the upper and lower back, hips, and the muscles that support your spine.
The prone press up can help ease stiffness in the lower back for some people. If you feel more pain in your legs, numbness, tingling, or a change in how your legs or feet feel during the move, stop right away. Do not push through nerve symptoms, and talk with your clinician before trying again.
Doing stretches regularly matters more than doing long, hard sessions. If you practice a little every day, you are more likely to keep your joints flexible and your back strong. Use the chart below to plan how often you stretch, how long to hold each stretch, and how many times to repeat.
| Goal | Frequency | Hold Time | Repetitions |
|---|---|---|---|
| Ease stiffness | Daily or 5 days per week | 15 to 30 seconds | 2 to 4 per side |
| Posture support | Daily micro‑breaks | 5 to 10 seconds for resets | Little and often throughout the day |
| Warm up | Before activity | Gentle, shorter holds | 8 to 10 easy reps of mobility moves |
If your pain lasts more than a week or two despite trying home care, or if it wakes you at night or keeps you from daily tasks, you should seek an evaluation. Call if you notice numbness, tingling, weakness, or new changes in bowel or bladder control, as these need urgent attention.
Our team can diagnose the source of pain, tailor a stretching and strengthening plan, and coordinate physical therapy when needed.
If your neck or back pain keeps returning, a personalized plan usually helps most. Schedule an exam with Princeton Orthopaedic Associates so we can identify what is driving your symptoms and guide you through the right exercises for long‑term relief.

Please contact us! We'd love to help.
If you have pain, please contact us and schedule an appointment. We have urgent care facilities all over New Jersey for your convenience.
This blog post is meant to be informative and should not act as a self-diagnosis tool. If you’d like to see one of our doctors, please contact us here.
© 2025 Princeton Orthopaedic Associates. The contents of PrincetonOrthopaedic.com are licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. Copying without permission is strictly forbidden. Privacy Policy | Accessibility