
Book An Appointment
Physician Assistants
Physical & Occupational Therapists
KneeMRI ScansNon-OperativePhysiatry
Physical Therapy
Podiatry
Spine
Sports Medicine
TraumaUrgent Care
X-Ray Imaging

Iliotibial band syndrome, or more commonly called the IT Band, is a common source of aching on the outside of the knee or thigh. Below, you’ll learn what the iliotibial band is, why it gets irritated, how symptoms show up in daily life and sport, and the treatments that help you return to comfortable movement.
Whether you run, cycle, walk for exercise, or spend long hours sitting, this condition can affect how your hip and knee work together. The good news is that most people improve with a plan that reduces irritation and restores strength and mobility around the hip and knee.
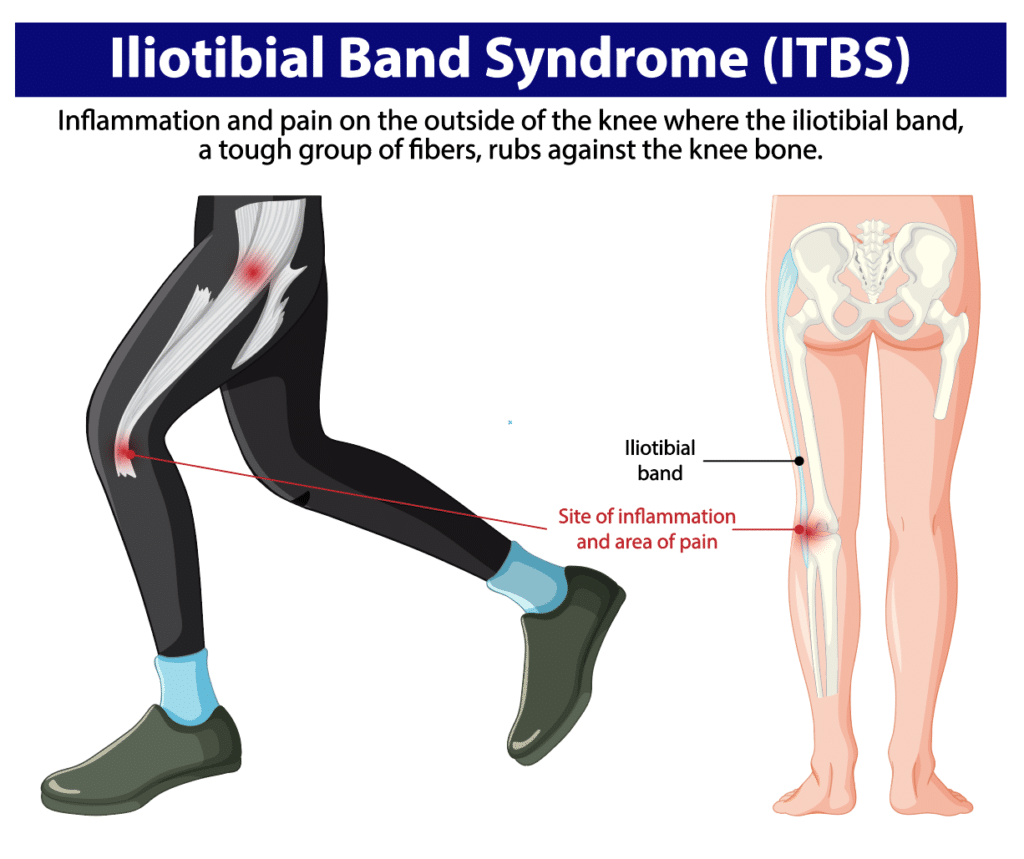
The IT band is a thick, fibrous band that supports the outside of your thigh. It connects muscles near the hip to the shinbone and helps stabilize the knee during walking, running, and standing.
Symptoms arise when tissues deep to the IT band (such as a fat pad or bursa) are compressed against the lateral femoral epicondyle during repetitive knee flexion and extension. This compression leads to irritation and pain on the outer knee, and may be felt higher up the thigh or into the hip.
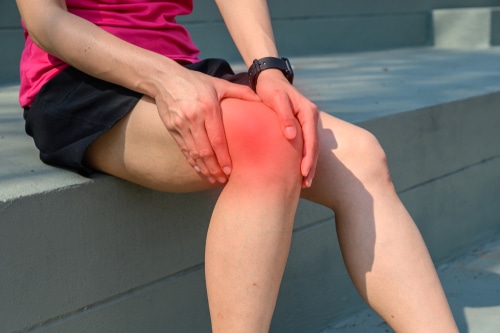
Symptoms often begin gradually and worsen with repetitive flexion and extension of the knee, such as during running, cycling, or climbing stairs. People commonly describe a mix of pain on the outer knee, tightness along the outside of the thigh, tenderness when the outer knee is touched, and discomfort that changes with movement. The pain can flare with activity but may ease with rest, and occasional stiffness after sitting is not required for the diagnosis.
Symptoms often begin gradually and tend to worsen with repetitive activities. People describe:
IT band irritation usually stems from how the leg moves and how much load it is asked to handle. Multiple factors can combine to create friction near the outer knee.
A sports medicine or orthopaedic clinician typically diagnoses IT band syndrome through your history and a focused exam. They’ll check tender areas along the outer knee and hip, assess hip and core strength, and look for tightness in surrounding muscles.
Imaging is not always needed. X-rays or an MRI may be ordered when symptoms are atypical, severe, or to rule out other causes of outer knee pain such as arthritis, meniscus problems, or stress injuries.
Most people recover with a stepwise approach that calms irritation and corrects the movement issues that caused it.
For persistent pain, a clinician may consider a carefully selected corticosteroid injection in the area of irritation (often image-guided). Injections should be used judiciously as part of a broader rehab plan. Surgery is rarely needed and is considered only when symptoms fail to improve after a thorough course of nonoperative care.
Healing time varies based on how long symptoms have been present, training demands, and how consistently you follow your plan. These general ranges are common:
| Stage | Typical Timeframe | What to Expect |
|---|---|---|
| Early | Several weeks | Pain reduces with activity changes, icing, and basic mobility work. |
| Established | 1 to 3 months | Strength and movement retraining restore tolerance for daily life and sport. |
| Recurrent or Chronic | Longer than 3 months | More comprehensive rehab and training plan adjustments are needed. |
Prevention means keeping movement balanced and building strength around the hip and knee. A simple plan can help avoid flare-ups: gradually increase activity, vary routes, stretch key muscles, and choose footwear that fits your needs. Regular rest breaks and listening to your body are important to prevent irritation from returning.
Schedule an evaluation if pain lasts more than a week, returns when you resume activity, or changes how you walk or run. Early guidance helps you recover faster and reduces the risk of the problem becoming chronic.
| Specialty | Best For | Notes |
|---|---|---|
| Sports Medicine | Activity-related knee and hip pain; nonoperative care | First stop to confirm diagnosis and plan treatment |
| Physiatry | Movement analysis and musculoskeletal pain | Addresses posture, gait, and functional limitations |
| Orthopaedic Surgery | Persistent or complex cases | Coordinates imaging or advanced options if needed |
| Physical Therapy | Strength, flexibility, and gait retraining | Guides a graded return to activity and long-term prevention |
IT band syndrome can interrupt training and make everyday tasks frustrating, but it is highly treatable. With the right mix of activity changes, targeted strengthening, mobility work, and expert guidance, you can ease pain and return to the activities you enjoy.
© 2026 Princeton Orthopaedic Associates. The contents of PrincetonOrthopaedic.com are licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. Copying without permission is forbidden. HIPAA Notice of Privacy Practices | Privacy Policy | Accessibility
