
Book An Appointment
Physician Assistants
Physical & Occupational Therapists
KneeMRI ScansNon-OperativePhysiatry
Physical Therapy
Podiatry
Spine
Sports Medicine
TraumaUrgent Care
X-Ray Imaging

Foot pain can come from many sources, from irritated tendons and tight fascia to nerve irritation and arthritis. Here, you’ll find a clear overview of why feet hurt, how to tell what might be going on, and the proven ways we help people heal and stay active.
Whether your foot pain is new or has lasted for months, know how your pain acts, where it hurts, and how it changes with walking or standing. This helps you find relief faster. You can start practical steps today and use the medical options we choose when home care does not work.

Your foot has 26 bones, numerous joints, strong ligaments, and powerful tendons. This complex design allows it to absorb shock, stabilize the body, and push you forward with every step.
Problems arise when tissues are overworked, inflamed, worn by arthritis, or irritated by pressure or footwear. The plantar fascia, Achilles tendon, and small nerves between the toes are frequent sources of symptoms.
Use this guide to match common pain locations with frequent causes and typical clues. A precise diagnosis still requires an exam.
| Region | Possible Causes | Typical Clues |
|---|---|---|
| Heel | Plantar fasciitis, Achilles tendinitis, heel spur, stress fracture, bursitis | First-step pain in the morning, pain after sitting, tenderness under the heel or back of heel |
| Arch / Bottom of Foot | Plantar fasciitis, posterior tibial tendon issues, flatfoot strain | Aching along the arch, worse with prolonged standing or long walks |
| Ball of Foot / Toes | Metatarsalgia, Morton neuroma, sesamoiditis, hammertoe irritation | Burning or pebble-like feeling under the forefoot, numbness between toes |
| Top of Foot / Midfoot | Extensor tendinitis, midfoot arthritis, Lisfranc sprain, stress fracture | Pain with lacing shoes tightly, swelling on top, pain with push-off |
| Outer Foot / Ankle | Ankle sprain, peroneal tendinitis | Tenderness along outer ankle or foot, pain on uneven ground |
| Big Toe Joint | Bunion, hallux rigidus, turf toe, gout | Prominent bunion, stiffness or grinding, sudden redness and swelling with gout |
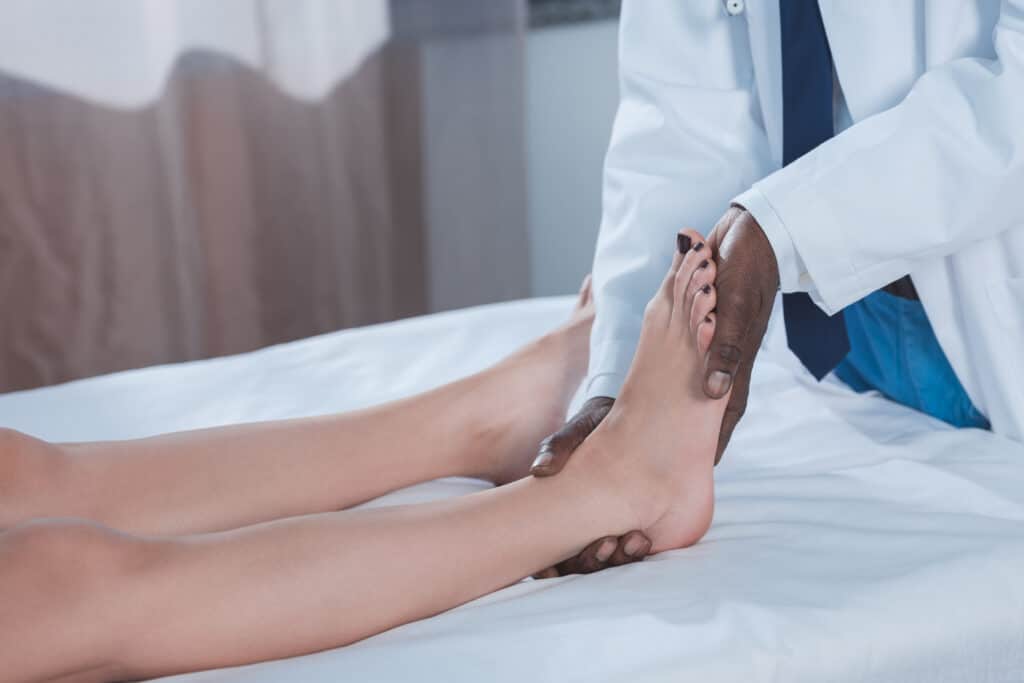
Your specialist begins with a careful history and hands-on exam. We look at where it hurts, when it hurts, your footwear, and how you walk.
The goal is a clear diagnosis, so your treatment targets the true source of pain.
Most foot pain improves with a combination of activity changes, shoe adjustments, focused exercises, and targeted medical care. Your plan will be tailored to your diagnosis and goals.
If foot pain is limiting your day, we’re here to help you find the cause and create a clear plan forward. Schedule an exam with a Princeton Orthopaedic Associates specialist to start moving comfortably again.

Please contact us! We'd love to help.
If you have pain, please contact us and schedule an appointment. We have urgent care facilities all over New Jersey for your convenience.
This blog post is meant to be informative and should not act as a self-diagnosis tool. If you’d like to see one of our doctors, please contact us here.
A strong back line, called the posterior chain, helps you stand tall and move well. It may help protect your spine, and it supports everyday tasks like lifting, climbing stairs, and getting up from a chair. It covers what the posterior chain includes, why it matters for back and knee comfort, easy form cues, and safe exercises you can start today.
We’ll also outline how often to train, common mistakes to avoid, and when it may be helpful to see a clinician at Princeton Orthopaedic Associates for personalized care and safer progress.
Please note that these exercises are listed here as examples. You will absolutely need to consult with a qualified doctor, trainer, or medical professional to decide if this information is right for you. You can cause harm to yourself by doing exercises incorrectly or those that do not align with your body or desired outcomes. Please be careful!

The posterior chain runs along the back of the body and is made of muscles that help keep the spine steady and allow the hips to extend. These muscles work together with many daily activities, such as standing, walking, lifting, and climbing stairs, so keeping them strong can support good posture and ease movement. Keeping this area strong supports your posture and reduces strain during daily activities.
The hip hinge is the foundation of many posterior chain moves. Instead of bending your back, shift your hips back while keeping your spine in a comfortable neutral range so the glutes and hamstrings do the work.
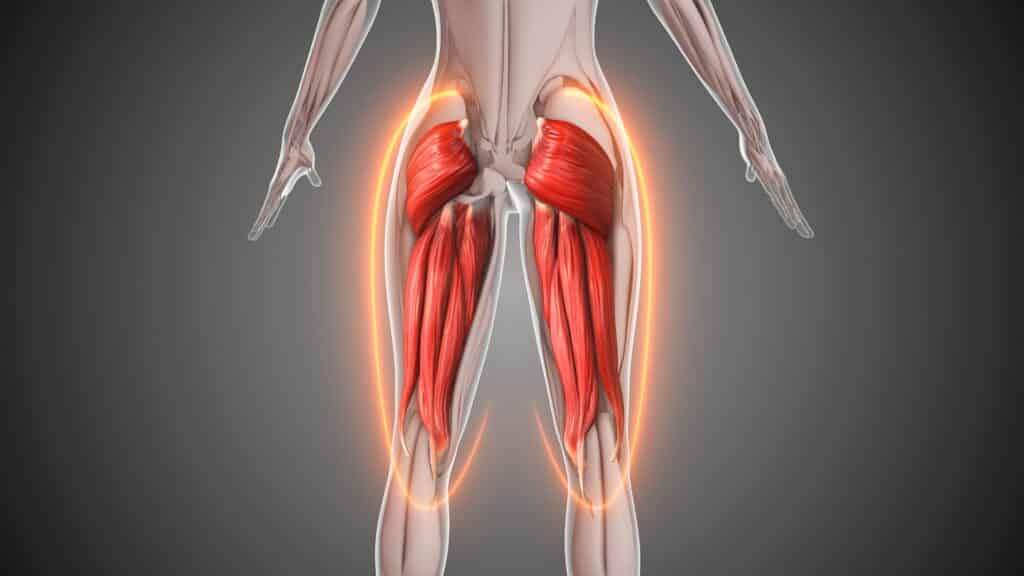
Practice by lightly touching your hips to a wall behind you or sliding your palms down your thighs to learn the pattern.
Choose 3 to 5 movements that feel comfortable and fit your body. Do each with slow, controlled reps and steady breathing. Focus on keeping good muscle control rather than rushing to finish. This careful approach helps you learn the pattern and build strength safely.
| Exercise | Main Muscles | How to Do It | Reps |
|---|---|---|---|
| Glute Bridge | Glutes, hamstrings | Lie on your back, knees bent, feet hip-width. Exhale and lift hips until shoulders, hips, and knees line up. Pause, then lower with control. | 8 to 12 |
| Hip Hinge to Wall | Glutes, hamstrings | Stand a foot from a wall. Push hips back to tap the wall while maintaining a comfortable neutral range in your spine, then stand tall. | 8 to 12 |
| Romanian Deadlift (light dumbbells) | Glutes, hamstrings, back stabilizers | Hold weights by your thighs. Hinge at the hips with soft knees until you feel hamstring tension, then press through heels to stand. | 6 to 10 |
| Hamstring Curl (exercise ball or sliders) | Hamstrings, glutes | Bridge hips, then bend knees to roll the ball or sliders toward you. Keep hips lifted and trunk steady. | 8 to 12 |
| Bird Dog | Spinal stabilizers, glutes | On hands and knees, brace your core. Reach opposite arm and leg long without arching the back. Pause, switch sides. | 6 to 10 each side |
| Step-up | Glutes, calves | Stand a foot from a wall. Push your hips back to tap the wall while maintaining a comfortable neutral spine, then stand tall. | 8 to 12 each side |
Most people benefit from training the posterior chain on nonconsecutive days so the muscles have time to rest and recover. Spacing workouts helps you keep good form and avoid overload. Consistent practice slowly builds strength and control while protecting your knees and back.
| Level | Frequency | Sets x Reps | Notes |
|---|---|---|---|
| Beginner | 2 days per week | 1 to 2 sets of 8 to 12 reps | Prioritize form and slow tempo; stop a rep or two before fatigue changes your form. |
| Intermediate | 2 to 3 days per week | 2 to 3 sets of 6 to 12 reps | Increase load gradually when all reps feel steady and controlled. |
Safety note: Individuals with osteoporosis, acute low back or radicular pain, or recent postoperative status should consult a clinician before hip hinging or deadlifting.
If pain limits your daily activities, you’re unsure about your form, or you have had a recent injury, consider seeing an orthopaedic specialist. Getting advice early can help you avoid delays, keep your movement safe, and build strength steadily. A clinician can check your technique and tailor exercises to your needs.
At Princeton Orthopaedic Associates, we evaluate the way you move, identify which muscles need attention, and create a clear plan to reach your goals. If needed, we coordinate care with physical therapy to help you progress step by step.

Please contact us! We'd love to help.
If you have pain, please contact us and schedule an appointment. We have urgent care facilities all over New Jersey for your convenience.
This blog post is meant to be informative and should not act as a self-diagnosis tool. If you’d like to see one of our doctors, please contact us here.
Knee pain after a run is common, whether you are new to running or building mileage. Below you will find the most frequent causes, how to tell what is driving your pain, simple steps to feel better, and when it is time to schedule an exam with our team at Princeton Orthopaedic Associates.

Use this guide to match your pain pattern with likely sources. An exam is the best way to confirm the diagnosis.
| Location of Pain | Possible Cause | Common Triggers |
|---|---|---|
| Front of the knee or behind the kneecap | Patellofemoral pain syndrome (runner’s knee) | High-impact mileage, prior injuries, and age-related changes |
| Sprinting, jumping, high-load quad work | Iliotibial band syndrome | Downhills, slanted roads, sudden mileage increases |
| Outside of the knee | Patellar tendinopathy | Hills, stairs, prolonged sitting, weakness of the hips or quads |
| Repetitive kneeling, direct pressure, and overuse | Meniscal irritation or tear | Twisting, deep knee bends, uneven terrain |
| Stiffness and swelling after activity | Knee osteoarthritis | Inside line of the knee or catching sensation |
| Warmth or tenderness near the kneecap | Bursitis | Repetitive kneeling, direct pressure, overuse |
Running multiplies the force through your knees with every step. Small issues in strength, flexibility, or form can add up over thousands of strides.
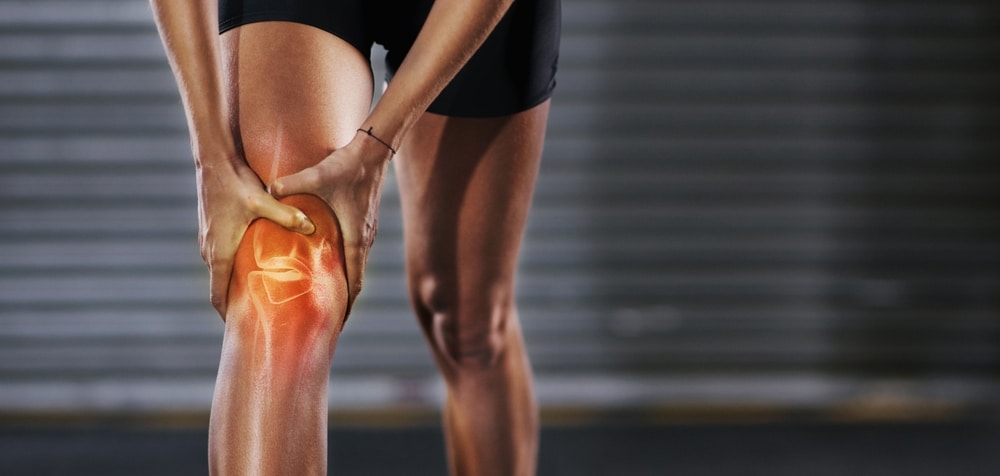
These steps are safe for most runners and are intended to reduce irritation while protecting the knee. Start by reducing hard miles and hills, then gradually resume activity as comfort returns. If pain persists for more than a week despite rest, or if you notice swelling, catching, or weakness, consult a clinician promptly.
These conditions often respond well to targeted rehab and training changes.
| Condition | What It Is | Helpful Strategies |
|---|---|---|
| Patellofemoral pain | Irritation where the kneecap tracks over the femur | Hip and quad strengthening, taping or bracing, cadence work, hill modification |
| Iliotibial band syndrome | Compression/impingement of tissues over the lateral femoral epicondyle and adjacent fat pad (commonly referred to as IT band syndrome). | Gradual loading, eccentric and isometric quad exercises, and manage jumping volume |
| Patellar tendinopathy | Overload of the tendon below the kneecap | Reduce twisting and deep knee bends, progressive strengthening, and imaging if persistent |
| Meniscal irritation | Stress or tearing of shock-absorbing cartilage | Strength, low-impact cardio, weight management, activity modification |
| Knee osteoarthritis | Wear of joint cartilage with age or prior injury | Gradual loading, eccentric and isometric quad exercises, and managing jumping volume |
If knee pain is keeping you from the miles you love, we can help you identify the cause and build a clear plan back to comfortable running.

Please contact us! We'd love to help.
If you have pain, please contact us and schedule an appointment. We have urgent care facilities all over New Jersey for your convenience.
This blog post is meant to be informative and should not act as a self-diagnosis tool. If you’d like to see one of our doctors, please contact us here.
© 2025 Princeton Orthopaedic Associates. The contents of PrincetonOrthopaedic.com are licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. Copying without permission is strictly forbidden. Privacy Policy | Accessibility
